Lab 12: Staphylococcus and Streptococcus
- Page ID
- 24060
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)DAY 1:
How do we identify gram-positive Staphylococcus and Streptococcus bacteria?
In this lab we will conduct experiments to identify the following species:
- Staphylococcus aureus: the most pathogenic for humans; can cause skin infections and food poisoning but is also found in microbiota of nasopharynx
- Staphylococcus epidermidis: part of the normal flora of our skin but can cause opportunistic infections
- Staphylococcus saprophyticus: causes urinary tract infections
- Staphylococcus simulans: part of the normal flora of our skin but can cause opportunistic infections
- Streptococcus pyogenes: can be found on human skin and can cause various infections (sore throat, skin)
- Streptococcus pneumoniae: found in microbiota of nasopharynx, can cause pneumonia and meningitis
- Streptococcus agalactiae: found in microbiota of gastrointestinal and genitourinary tract, can cause neonatal infections
MANNITOL SALT AGAR PLATE (MSA)
 Selective for gram-positive bacterium (e.g. Staphylococcus). Mannitol fermentation by pathogenic staphylococci, such as S. aureus and S. simulans. is indicated by the agar media changing from red to yellow.
Selective for gram-positive bacterium (e.g. Staphylococcus). Mannitol fermentation by pathogenic staphylococci, such as S. aureus and S. simulans. is indicated by the agar media changing from red to yellow.
SELECTIVE AGENT: NaCl (salt)
DIFFERENTIAL AGENT: mannitol sugar fermentation
INDICATOR: Phenol red
ISOLATE BACTERIA FROM YOUR NOSE: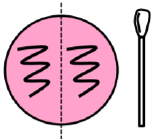
In this lab, you will be asked to isolate various species of bacteria from different parts of your body. Subsequent biochemical testing will demonstrate the variability seen among the microbiota of your body. In this session, you will isolate Staphylococci bacteria from your nose and Streptococcus from your throat.
1. Working with your lab partner collect two MSA plates (plate 1 for nose samples, plate two for provided bacterial species)
2. Use a sterile cotton tipped swab to collect a sample DEEP in your nose. 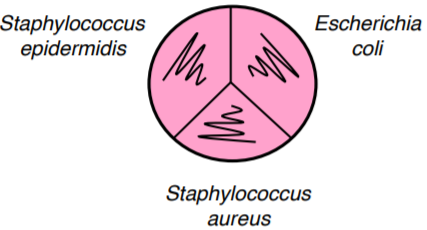
3. Aseptically streak your nose sample (NOT SFIC, NOT LAWN) on your half of the first MSA plate. Incubate at 37°C
4. Using a loop, aseptically streak (NOT SFIC, NOT LAWN) the provided three bacterial species on MSA plate #2. Incubate at 37°C.
Note
You will be comparing the growth between the three sections so make sure your streaks are of equal size.
BLOOD AGAR PLATE (BAP)
 Nutrient-rich; used for recovery of bacteria and fungi from samples and can determine hemolytic patterns. Our plates are made with sheep’s blood.
Nutrient-rich; used for recovery of bacteria and fungi from samples and can determine hemolytic patterns. Our plates are made with sheep’s blood.
SELECTIVE AGENT: none
DIFFERENTIAL AGENT: hemolysis (ability to digest/breakdown RBCs)
α-hemolysis will only cause partial lysis of the red blood cells and will appear greenish brown with no halo. Alpha hemolysis is caused by hydrogen peroxide produced by the bacteria, oxidizing hemoglobin to green methemoglobin (e.g. Streptococcus viridans and S. pneumoniae)
β-hemolytic activity will show lysis and complete digestion of red blood cell contents surrounding the colony, most are pathogenic (e.g. Streptococcus pyogenes)
γ-hemolysis is non-hemolytic (Streptococcus salivarius)
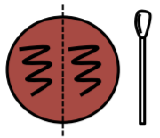
6. Collect a single BAP plate.
7. Divide a BAP plate into half. Using a sterile swab, collect a sample from your partner's throat and aseptically streak on one side of the plate.
8. Your partner will then collect a sample from your throat and aseptically streak it on to the other side of the plate. Incubate at 37°C.
THE FOLLOWING PORTION YOU WILL DO AS A TABLE:
9. Divide three BAP plates in half and using a sterile swab aseptically make a lawn of the bacterial species on each side as pictured below.
10. Place the appropriate antibiotic disc on each plate. Incubate at 37°C.
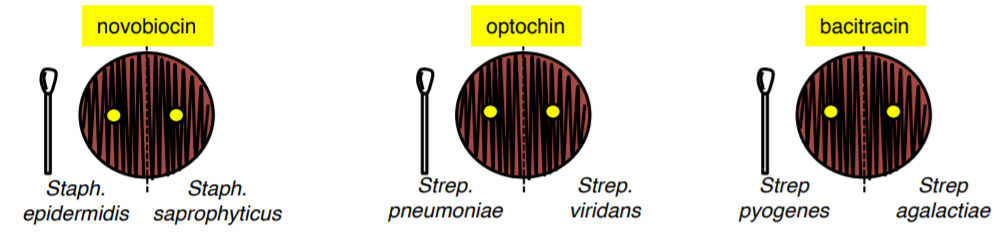
11. Using a loop, aseptically streak (NOT SFIC, NOT LAWN) the provided three bacterial species on a blood agar plate. Incubate at 37°C.
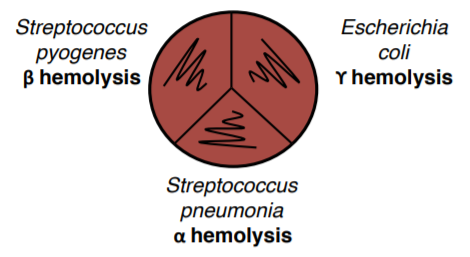
CAMP TEST

Used to differentiate Streptococcus agalactiae CAMP-positive from Streptococcus pyogenes CAMP-negative. The β-lysin produced by β-hemolytic
Staphylococcus aureus acts synergistically with Streptococcus agalactiae to create enhanced hemolysis in the region between the two cultures. The
synergistic zone is not observed in other Streptococcus.
CAMP TEST:
12. Make sure you label each of your streaks on your BAP plate for the CAMP test. The bacteria that you will need for this assay are on a rack at the front of each table. With a loop, streak Staphylococcus aureus in a straight line down the center of a BAP plate.
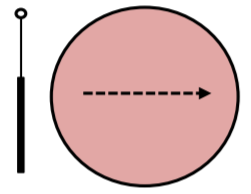
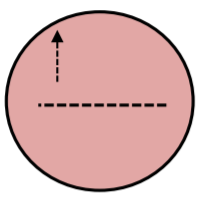
13. With a loop, streak Streptococcus agalactiae as a control perpendicularly to S. aureus streak but do not touch.
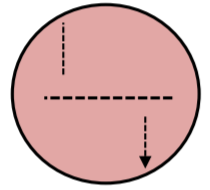
14. With a loop, streak Streptococcus pyogenes on the other side in a similar manner and incubate at 37°C (no CO2).
DAY 2:
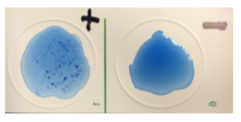
RABBIT PLASMA TEST
 It is used to distinguish between pathogenic and nonpathogenic members of Staphylococcus. The exo-enzyme coagulase enables the conversion of
It is used to distinguish between pathogenic and nonpathogenic members of Staphylococcus. The exo-enzyme coagulase enables the conversion of
fibrinogen to fibrin to form an insoluble clot. Staphylococcus aureus is usually coagulase-positive. Coagulase is tightly bound to the surface of the S.
aureus and can coat its surface with fibrin upon contact with blood. The fibrin clot protects the bacterium from phagocytosis and other defenses of the
host. An S. aureus infection of the blood, if left untreated, will result in death.
1. Working with your lab partner(s), record your results for your BAP, MSA, and CAMP plates on your worksheet.
2. Get TWO coagulase test tubes.
3. Aseptically inoculate the test tube with EITHER of the following:
- an extra large loopful of your nose sample (YELLOW COLONIES ONLY!)
- Bacteria A from the plate provided to you
4. Aseptically inoculate your other test tube with
- Bacteria B from the plate provided to you
5. Gently mix and incubate at 37°C.
HARDY StaphTEX BLUE KIT:
5. Label three of the reaction circles from the HARDY StaphTEX Blue Kit as +, -, and ?
6. Invert and mix the latex reagent from the HARDY StaphTEX Blue Kit.
7. Squeeze 1 drop of the re-suspended latex reagent onto 3 of the reaction circles on the slide-card.
8. Add one drop of the positive control onto another circle. Add one drop of the negative control onto another circle WITHOUT THE DROPS TOUCHING.
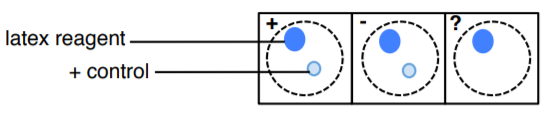
9. Using a wooden applicator stick, apply the same bacteria you used in step 3 into the (?) reaction circle and mix.

10. Using a separate wooden stick, mix the reagents within the (+) and (-) reaction circle GENTLY! Make sure to spread the mixture out to cover most of the circle as it will make the reaction easier to see.
11. Gently hand rock the slide-card for 20 seconds to agitate the mixture (avoid spilling onto other reaction circles). Record your results on your worksheet.
widal test
Salmonella typhi causes typhoid fever while Salmonella paratyphi causes a milder form of the disease. French bacteriologist George Widal (1862-1929) developed the Widal test to differentiate the two. The Widal test is a serological test that utilizes a suspension of killed Salmonella typhi as an antigen to detect the presence of anti-Salmonella typhi antibodies in a patient’s serum. Although the use of the Widal test in developed countries has waned, it still used a diagnostic tool in developing countries.
Antibody titers are low during the 1st week of infection with both bacteria and slowly rise over time. Infections with any other gram-negative bacteria may yield a false positive result due to cross-reactivity. To allow for the confidence of diagnosis, patient tests are submitted in paired serum samples (1st test done early and 2nd test done 2 weeks later).
WIDAL TEST:
12. Label 8 conical tubes 1:20,1:40, 1:80, 1:160, 1:320, 1:640, 1:1280, and negative control.
13. Add 500 μl of sterile saline to each tube using a pipetter.
14. Obtain a 1:10 dilution of serum (patient sample which contains antibodies) from your instructor.
15. Add 500 μl of patient serum to the 1:20 tube, finger vortex.
16. Take 500 μl from the 1:20 tube and pipette into the 1:40 tube, finger vortex.
17. Take 500 μl from the 1:40 tube and pipette into the 1:80 tube, finger vortex.
18. Take 500 μl from the 1:80 tube and pipette into the 1:160 tube, finger vortex.
19. Take 500 μl from the 1:160 tube and pipette into the 1:320 tube, finger vortex.
20. Take 500 μl from the 1:320 tube and pipette into the 1:640 tube, finger vortex.
21. Take 500 μl from the 1:640 tube and pipette into the 1:1280 tube, finger vortex.
22. Take 500 μl from the 1:1280 tube and discard.
23. Add 500 μl of heat-killed HD S. typhi flagella antigen to every tube, INCLUDING the original 1:10 dilution of the patient serum and the negative control.
24. Incubate at 50°C water bath.


