15.7D: Prenatal Screening
- Page ID
- 5499
Many tests are now available to detect genetic diseases such as sickle cell disease, cystic fibrosis and phenylketonuria (PKU). Most of these tests can not only be performed on cells removed from adults but also on cells removed from the fetus and even from a pre-implantation embryo.
Amniocentesis
During its development, the fetus sheds cells into the amniotic fluid. After 14–22 weeks of pregnancy, a small volume of this fluid can be removed (using a needle inserted through the abdominal wall).
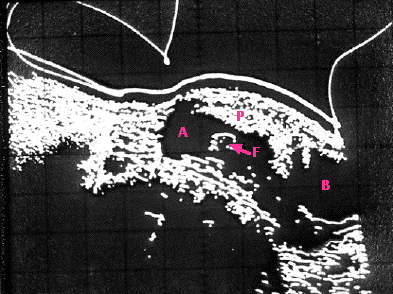
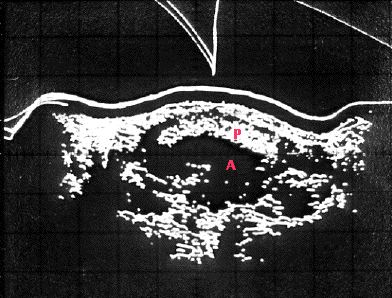
Using ultrasound to locate the position of the placenta prior to amniocentesis. These sonograms are made by recording the echoes received from structures within the abdomen. A, amniotic cavity; B, urinary bladder; F, part of the fetus; P, placenta. Both longitudinal (left) and transverse (right) scans are needed for accurate localization of the placenta. (Courtesy of the Downstate Medical Center of the State University of New York.)
Separating the cells and culturing them enables the clinician to look for
- chromosome abnormalities (e.g., the three number 21 chromosomes of Down syndrome)
- certain enzymatic defects (e.g., an inability to metabolize galactose, hence milk)
- the sex of the fetus
Over 100 genetic abnormalities can be diagnosed by amniocentesis and the pregnancy deliberately ended if the parents wish it.
Chorionic Villus Sampling (CVS)
This is an alternate method of prenatal diagnosis. A small amount of placental tissue is sucked out by a tube inserted through the abdominal wall or through the vagina (the latter avoiding the need for an incision). For some tests the fetal cells can be examined immediately without the need to culture them. Another advantage of CVS is that it can be performed earlier in pregnancy (after only 10–12 weeks) than amniocentesis. If an abortion is to be performed, it is a simpler process early in pregnancy.
Non-Invasive Prenatal Genetic Testing (NIPT)
Although the blood vessels of the placenta are in close contact with the mother's blood vessels in the uterus, intermingling of their blood does not normally occur. However some of cells of the fetus do manage to get into the mother's circulation where they may represent 1 in a million of her white blood cells (so only some 2–6 cells per ml of blood). Fragments of fetal DNA (~ 300 bp long) from apoptotic cells of the placenta are also found in the mother's plasma as early as 5 weeks after implantation. This raises the possibility of using genetic tests (e.g., PCR) to identify mutations or chromosomal abnormalities in the fetus using a small (~10 ml) sample of blood drawn from the mother.
Two home blood test kits for determining the sex of the fetus are already on the market. The collected drops of blood are sent to a laboratory to determine whether any Y-chromosome-specific DNA (e.g., SRY) is present. Tests of fetal DNA for Down syndrome (trisomy 21), as well as for trisomy 13 and 18, have both higher sensitivity (false negatives <0.1%) and specificity (false positives <0.2%) than amniocentesis and CVS.
In several European countries, Rh-negative mothers can now have their blood screened for the presence of an Rh-positive fetus. The time will surely come when such NIPT screening will become available for many genetic disorders. The procedure is also called non-invasive prenatal diagnosis - NIPD.
The level of fetal DNA in the mother's blood rises to a peak at the time of birth and some evidence suggests that this rise may be a trigger to start the birth process.
Preimplantation Genetic Diagnosis (PGD)
Genetic Analysis of Blastomeres
One of the remarkable facts about mammalian development is that all the cells in the early (e.g., 8-cell) embryo are not needed to produce a healthy fetus (which is why a single fertilized egg can on occasions produce identical twins, triplets, etc.). So couples using in vitro fertilization (IVF) also can take advantage of genetic screening. While the embryo is in culture, one or two cells can safely be removed and tested for their genotype. For example:
- The sex of the embryo can be determined with a probe for Y-specific DNA. This permits prospective mothers carrying a severe X-linked trait like hemophilia A to choose a female rather than a male embryo for attempted implantation.
- Fluorescent probes specific for the DNA of particular chromosomes can detect (by FISH) if there is an abnormal number (aneuploidy) such as the three #21 chromosomes of Down syndrome.
- In fact the entire karyotype of the embryo can be determined. Random fragments of DNA prepared by the polymerase chain reaction (PCR) of all the DNA of a cell from the embryo can be
- given a fluorescent label
- applied to the metaphase chromosomes of a standard reference cell that has a normal karyotype along with
- DNA fragments from the reference cell labelled with a different color.
- too much (e.g. 3 copies of #21 — trisomy)
- too little (only a single copy of #14 — monosomy)
Genetic Analysis of Polar Bodies
As meiosis I is completed, one set of duplicated chromosomes (dyads) is extruded into the first polar body. The DNA of the polar body can be amplified by the polymerase chain reaction (PCR) and tested.
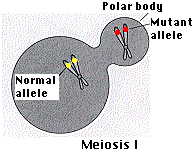
If the mother is heterozygous for a trait, and no crossover has occurred, and the polar body contains the mutant alleles (see figure), the egg can be safely fertilized. (For simplicity, the figure shows only the pair of homologues carrying the locus of concern.)
However, if crossing over has occurred, the first polar body would contain one mutant and one healthy allele. In that case, there is a 50:50 chance that, after fertilization, the other copy of the mutant allele will end up in the egg (instead of in the second polar body). So the second polar body should also be tested to see if it also contains the mutant allele. Only if it does can the egg be safely used.
Contributors and Attributions
John W. Kimball. This content is distributed under a Creative Commons Attribution 3.0 Unported (CC BY 3.0) license and made possible by funding from The Saylor Foundation.


