9.2: Candida
( \newcommand{\kernel}{\mathrm{null}\,}\)
The yeast Candida is normal flora of the gastrointestinal tract and is also frequently found on the skin and on the mucous membranes of the mouth and vagina. Candida is normally held in check in the body by:
1. The body's normal immune defenses; and
2. The body's normal bacterial microbiota.
However, Candida may become an opportunistic pathogen and overgrow an area of colonization if the host becomes immunosuppressed or is given broad-spectrum antibiotics that destroy the normal bacterial microbiota. (Since Candida is eukaryotic, antibiotics used against prokaryotic bacteria do not affect it.)
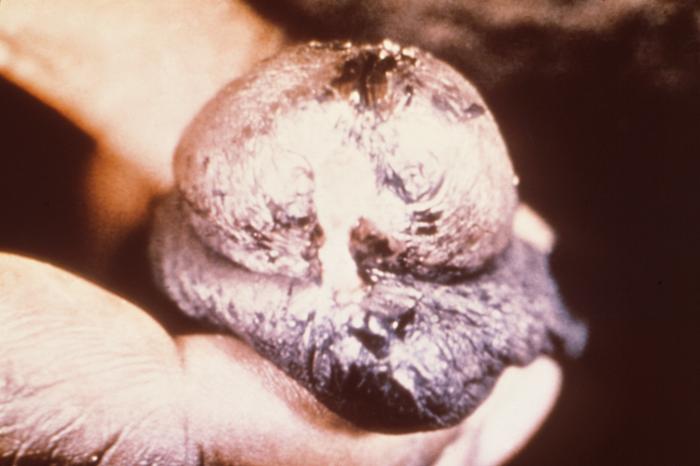
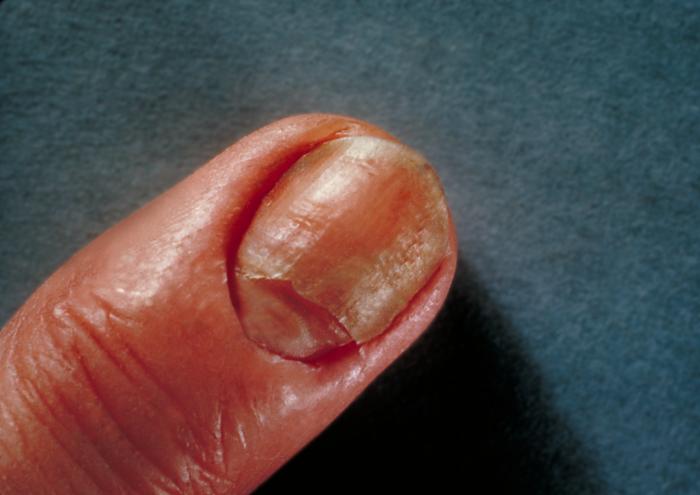
Any infection caused by the yeast Candida is termed candidiasis. The most common forms of candidiases are oral mucocutaneous candidiasis, or thrush (see Fig. \(\PageIndex{1A}\) and Fig. \(\PageIndex{1B}\)), vaginitis (see Fig. \(\PageIndex{1C}\) and \(\PageIndex{1D}\)), balantitis (infection of the penis, Fig. \(\PageIndex{1E}\)), onychomycosis (infection of the nails; Fig. \(\PageIndex{1F}\)), and dermatitis (diaper rash and other infections of moist skin). In addition, Candida can cause urinary tract infections. However, antibiotic therapy, cytotoxic and immunosuppressive drugs, and immunosuppressive diseases such as diabetes, leukemias, and AIDS can enable Candida to cause severe opportunistic systemic infections involving the skin, lungs, heart, and other organs. In fact, Candida now accounts for 10% of the cases of septicemia. Candidiasis of the esophagus, trachea, bronchi, or lungs, in conjunction with a positive HIV antibody test, is one of the indicator diseases for AIDS.
|
Fig 9.2.1A: Candida albicans growing in the Mouth (Thrush) |
Fig. \(\PageIndex{1B}\): Mouth Smear of a Person with Thrush |
Fig 9.2.1C: Candida albicans growing on the Cervix |
Fig 9.2.1D: Vaginal Smear of a Person with Candida Vaginitis |
|---|---|---|---|
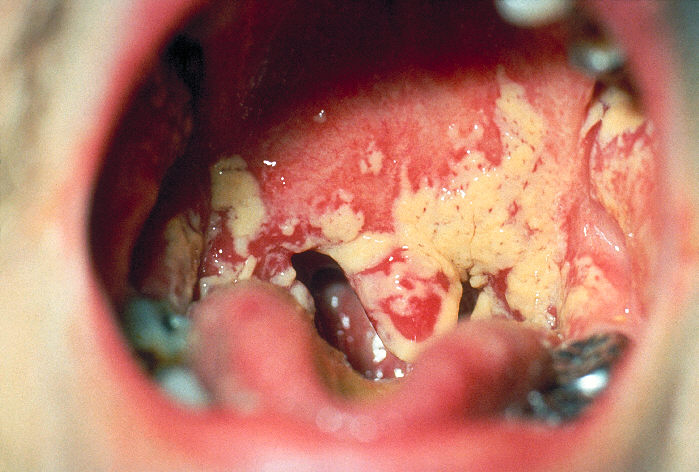 |
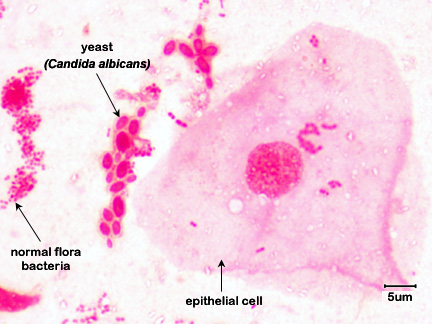 |
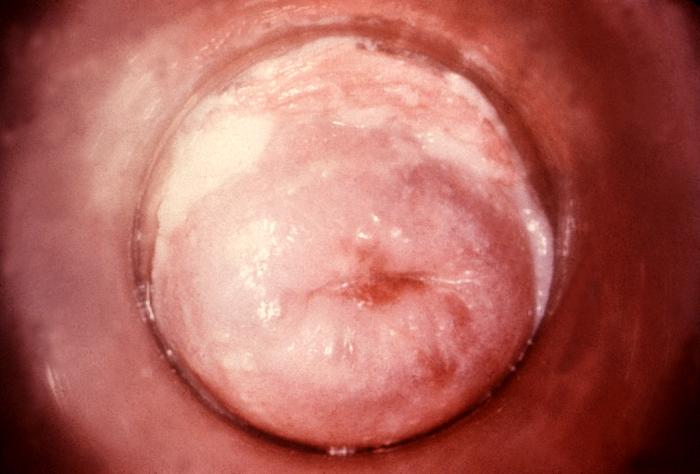 |
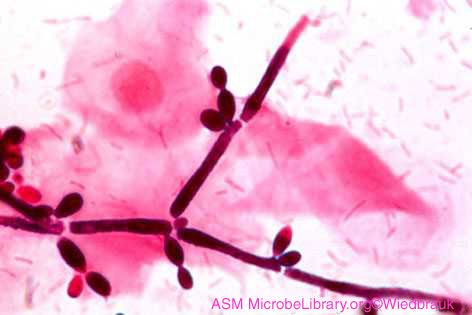 |
| Note budding yeast (arrows). |
Note epithelial cells, rod-shaped bacteria, and Candida albicans in its hyphal form. |
||
| By Content Providers: CDC [Public domain]. Courtesy of the Centers for Disease Control and Prevention |
Copyright; Gary E. Kaiser, Ph.D. The Community College of Baltimore County, Catonsville Campus CC-BY-3.0 | By Content Providers: CDC [Public domain]. Courtesy of the Centers for Disease Control and Prevention |
Copyright; Gary E. Kaiser, Ph.D. The Community College of Baltimore County, Catonsville Campus CC-BY-3.0 |
|
Fig 9.2.1E: Candida albicans Infection of the Penis (Balantitis) |
Fig. \(\PageIndex{1F}\): Candida albicans Infection of the Nails |
|---|---|
 |
 |
| Note budding yeast (arrows). | |
| By Content Providers: CDC [Public domain]. Courtesy of the Centers for Disease Control and Prevention |
Copyright; Gary E. Kaiser, Ph.D. The Community College of Baltimore County, Catonsville Campus CC-BY-3.0 |
The most common Candida species causing human infections is C. albicans, causing 50-60% of all Candida infections. Candida glabrata is second, causing 15-20% of Candida infections; Candida parapsilosis is third, responsible for 10-20%. More recently, Candida auris has been causing relatively rare but severe infections in patients that have been hospitalized for long periods of time, sometimes entering the bloodstream causing invasive infections throughout the body. C. auris is often resistant to common antifungal drugs and kills as many as 1 out of 3 patients with invasive infections.
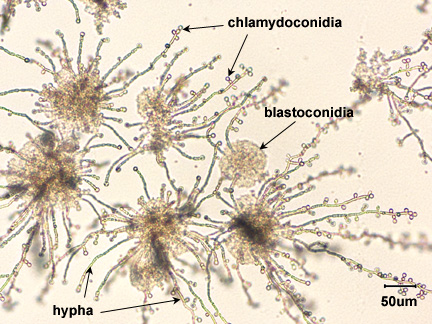
Candida is said to be dimorphic, that is it has two different growth forms. It can grow as an oval, budding yeast, but under certain culture conditions, the budding yeast may elongate and remain attached producing filament-like structures called pseudohyphae. C. albicans may also produce true hyphae similar to molds. In this case long, branching filaments lacking complete septa form. The pseudohyphae and hyphae help the yeast to invade deeper tissues after it colonizes the epithelium. Asexual spores called blastoconidia (blastospores) develop in clusters along the hyphae, often at the points of branching. Under certain growth conditions, thick-walled survival spores called chlamydoconidia (chlamydospores) may also form at the tips or as a part of the hyphae. (See Fig. 9.2.2.)
Contributors and Attributions
Dr. Gary Kaiser (COMMUNITY COLLEGE OF BALTIMORE COUNTY, CATONSVILLE CAMPUS)

