1.41: Human Microbiome
- Page ID
- 79463
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)- Define the terms microbial flora, microbiota, and microbiome.
- List locations in the human body where it is normal and healthy to have microbes growing.
- Explain how microorganisms keep humans healthy and give at least three ways they are beneficial to our health.
- Give at least three ways humans are not cultivating as healthy a microbiome as we could.
- Tell that the microbial communities are distinct in different areas of the human body.
- Tell that the microbial communities are distinct in different individuals.
- Grow microbes from your own skin microbiome.
- Characterize microbes grown from your own skin microbiome and tell the likely species they are.
Introduction to the Human Microbiome
The importance of the normal microbial flora (a.k.a. microbiota or microbiome) of the human body has been an area of increasing interest in both research and the popular media. One frequently cited statistic is that there are 10-100 times more bacterial than human cells in the body. More recent calculations, however, result in a ratio closer to 1:1, with an estimated 1013 human cells and 1013 – 1015 bacterial cells. The cellular contribution of microbes to the human body, however, is small compared to the genetic contribution. The human genome contains approximately 20,000 genes, but there are 3.3 million unique bacterial genes in the gut microbiota alone. That is a 150-fold difference between the human and bacterial genetic contribution. No matter the exact proportion of bacteria in the human body, the impact of the microbiota on our physiology is substantial.
It has been known for decades that animals raised without normal flora display a variety of health effects across many body systems. Not surprisingly, neither the digestive system nor the immune system develops properly. The cecum (part of the large intestine/colon) tends to be enlarged and other gastrointestinal (GI) abnormalities appear. The immune system is underdeveloped. More recently it has been shown that the central nervous system, including the brain, does not develop properly in these animals. Because bacteria produce vitamins necessary for animal nutrition (most notably vitamin K), animals without normal flora suffer from vitamin deficiencies. Lack of normal flora also makes animals more susceptible to infection with a variety of pathogens, particularly those that infect the GI tract. Although lack of normal flora generally has negative effects, it does also result in an absence of dental caries (cavities) and lower body fat.
Normal flora is found in all areas of the human body exposed to the environment (one exception is the lungs), but internal organs and body fluids are considered sterile in a healthy individual. This is generally true, although bacteria are sometimes found in these “sterile” tissues even in healthy people. For instance, a person’s blood will become bacteremic (contain bacteria) for up to three hours after brushing their teeth.
Each area of the human body contains a characteristic population of microbes, although the exact composition of each person’s flora is unique. The diversity of the bacteria populating the human gut alone is enormous, with an estimated 40,000 species. An increasing number of studies associates such shifts in the gut microbiota with outcomes such as susceptibility to infection, immune disorders, metabolic changes, and altered mood and behavior. Each of these physiological effects can be linked directly to chemical communication within the microbiota and between the microbiota and human.
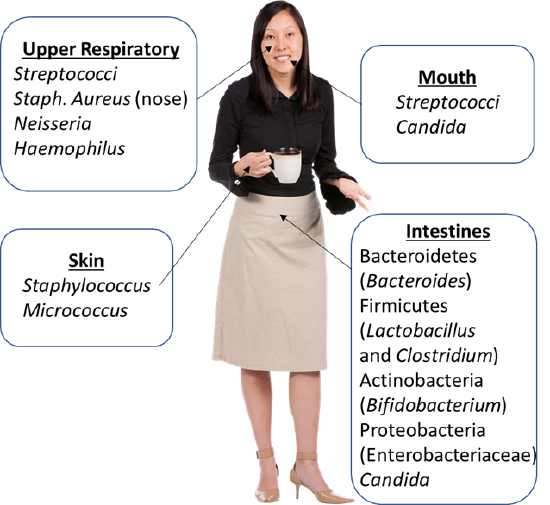
Figure 1: Locations of normal flora and the types of species commonly found in the different human habitats for microorganisms. (2021; Jeanne Kagle)
Flora of the Skin
The exact microbial population on the skin depends on the specific body area. Moist areas, such as axilla (armpits) and groin, tend to have more (and different) bacterial growth compared to drier areas. The most common bacteria of the skin flora are the Gram-positive, catalase positive cocci of the genera Staphylococcus and Micrococcus. Although Staphylococcus aureus can occasionally be found on the skin, it is more commonly found in the nose in those people that carry it in their normal flora.

Figure 2: The microbial community compositions differ based on the human skin locations. The microbial community compositions are shown for each skin location with pie charts representing the types of species present and the quantities of these species.
Flora of the Mouth and Upper Respiratory Tract
The flora of the mouth and upper respiratory tract is typically associated with a more diverse set of microbes. Streptococci, specifically, alpha-hemolytic Streptococci often referred to collectively as the “viridans Streptococci”are very prominent in the mouth. These include S. mutans, S. sanguis, and S. mitis. S. mutans in particular plays a critical role in the formation of plaque and dental caries (cavities). Although both Staphylococci and Streptococci are Gram-positive cocci, unlike the Staphylococci the Streptococci are catalase-negative, consistent with the low-oxygen environment of the mouth.
Other inhabitants of the mouth and upper respiratory tract include bacteria in the genera Neisseria and Haemophilus. As mentioned above, Staphylococcus aureus is most often found in the nose of those individuals who carry it in their normal flora. The fungal genus Candida is also common in the mouth and upper respiratory tract.
Flora of the Intestines
The most studied population of normal flora in the microbes living in the intestines. This population of microbes is commonly referred to as the gut microbiota or gut microbiome. Although the bacterial species most commonly associated with the intestines is Escherichia coli, it is actually not the most numerous in the intestine. Bacteria in the phylum Bacteroidetes form a large proportion of bacteria in the gut. The Gram-positive Firmicutes (such as Lactobacillus and Clostridium) and Actinobacteria (including Bifidobacterium) can be equally numerous. In healthy individuals, Proteobacteria (including E. coli and other Enterobacteriaceae) are the least abundant of the major bacterial groups in the intestines. There are many other groups of microbes found in the intestines, including fungi such as Candida. It is shifts in the proportions of these groups of microbes that are typically studied when investigating the role of normal flora on human health.
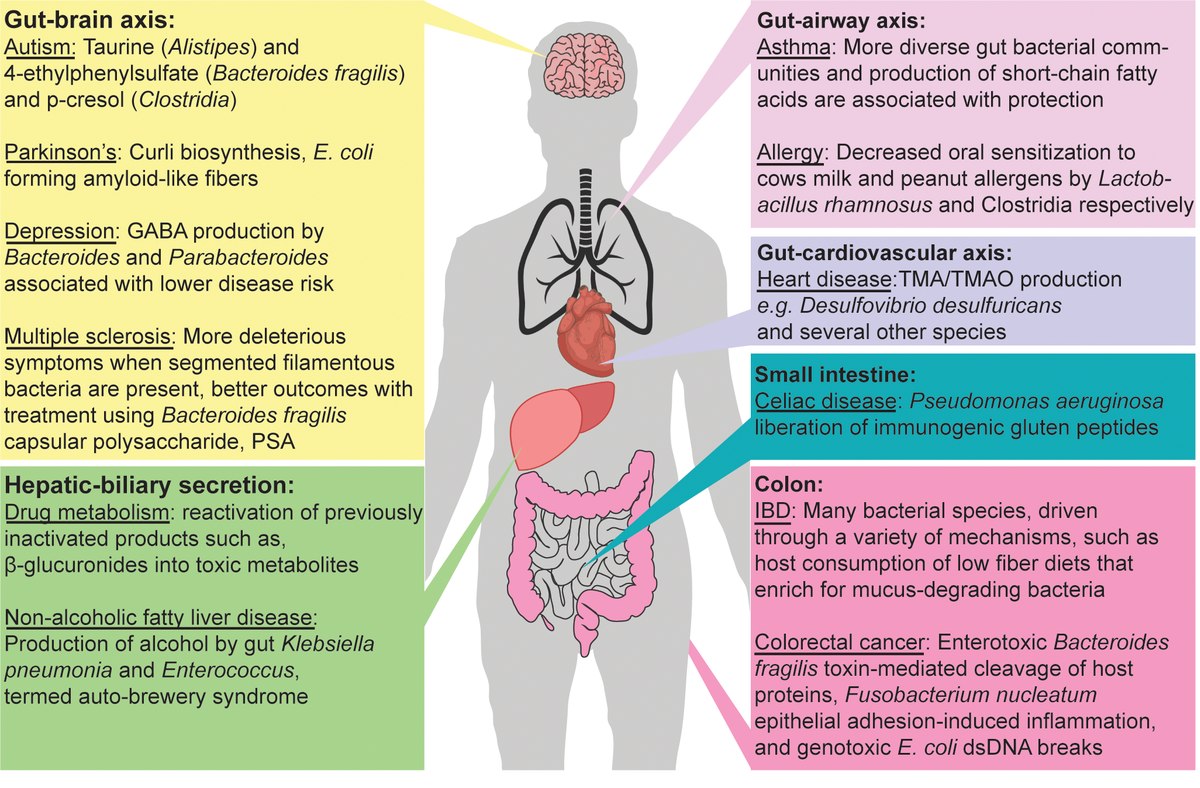
Figure 3: A summary of some of the know effects of the human gut microbiome relating to conditions affective multiple human organ systems.
Laboratory Instructions
In this experiment, a few locations of the skin will be swabbed in order to examine microbes present in different locations.
Prepare Petri Plates and Swab Skin
- Prepare 2 TSA plates per person.
- Label the 2 TSA plates with your name.
- Choose the 2 skin locations you would like to swab and label one petri plate with each location you chose.
- Moisten a sterile cotton swab with DI or distilled water.
- Swab the first skin location you chose and then do a zig-zag streak on the TSA plate you labeled with that skin location.
- Repeat steps 4 and 5 for the other skin location you chose.
- Invert the petri plates and incubate for 24 – 48 hours.
Examine Results
- Examine the TSA plates for colony morphologies. Choose one isolated colony from each petri plate. Choose colonies that have different morphologies. Describe the colony morphologies in the results & questions section below.
- Create two bacterial smears from the two isolated colonies you chose from each plate. You can use a single slide with one smear on each side. Label the slide so you do not get the two smears mixed up.
- Heat fix the two bacterial smears. Fix each individually (heat-fix one smear, let the slide cool off, then heat-fix the other smear).
- Conduct a Gram stain on the two bacterial smears (can be done at the same time.
- Examine the Gram-stained cells with a microscope.
- Record the cell shape, cell arrangement, and Gram for each of the colonies you chose.
- Use the table below to "identify" each species found on your skin. Write the species you found for each skin location.
|
Skin Organism |
Gram |
Microscopic Morphology |
Microscopic Arrangement |
Colony Appearance on TSA |
|---|---|---|---|---|
|
Staphylococcus epidermidis* |
Positive |
Cocci |
Clusters |
Large, round, white, glistening |
|
Staphylococcus aureus |
Positive |
Cocci |
Clusters |
Large, round glistening, typically yellow |
|
Corynebacterium spp.* |
Positive |
Pleomorphic rods |
Club-shaped, bipolar |
Dry and wrinkled |
|
Yeasts |
Positive |
Large budding cells |
Single |
Large, round, moist |
|
Bacillus spp.* |
Positive |
Bacilli |
Single, chains |
Round or irregular, surface dull becoming thick and opaque |
|
Streptococcus viridans* |
Positive |
Cocci |
Chains |
Small, dome-shaped colony surrounded by an area of discoloration. |
|
Micrococcus luteus |
Positive |
Cocci |
Single, tetrads |
Large, round, yellow, glistening colony |
* These are the most commonly isolated microorganisms from healthy skin.
Results & Questions
|
Skin location #1: ______________________ Results from colony on skin location #1 |
Skin location #2: ______________________ Results from colony on skin location #2 |
|
|---|---|---|
| colony color | ||
| colony appearance (shiny, dull, dry, moist, glistening, etc.) | ||
| colony form | ||
| Gram | ||
| cell shape | ||
| cell arrangement | ||
| likely species (based on the table above) |
- Complete the table above to summarize results of the two isolated colonies you chose.
- Examining the results from the skin swabs, answer the following:
- How many distinct types of microbes can you identify on the petri plates (each distinct type would have a different colony morphology)?
- Which of the skin locations you swabbed had the most microbes present?
- True or false. The microbes growing on your skin, under normal circumstances, are dangerous to your health.
- Explain why microbes growing on your skin may actually be beneficial to your health.
- List at least 3 ways microbes in your "gut" are important for keeping you healthy.
- What happens to your microbiome when you take antibiotics?
- What circumstances prevent humans from getting enough exposure to microbes to build up a healthy microbiome? Give at least three.
- True or false. All microbial communities living on the skin have the same composition.
- True or false. All humans have the same species composition in their gut microbiome.
Attributions
- Chapter Image: Holobiont representation.png by Helen Spence-Jones is licensed under CC BY-SA 4.0
- The Human Microbiota from BSC 3271: Microbiology for Health Sciences Sp21 (Kagle) by J. Kagle is licensed under an undeclared license.
- Journal.ppat.1008370.g001.tif by Robert W. P. Glowacki, Eric C. Martens is licensed under CC BY 4.0
- Skin Microbiome20169-300.jpg by Darryl Leja, NHGRI is in the public domain


