14.3: The Beta Streptococci
- Page ID
- 123468
Lancefield serologic groups A, B, C, D, F, and G are all streptococci that may show beta hemolysis on Blood agar. However, some group B streptococci are non-hemolytic and group D streptococci (discussed below) usually show alpha hemolysis or are non-hemolytic.
Streptococcus pyogenes, often referred to as group A beta streptococci or GAS because they belong to Lancefield serologic group A and show beta hemolysis on blood agar, are responsible for most acute human streptococcal infections. S. pyogenes isolates are Gram-positive cocci 0.5-1.0 µm in diameter that typically form short chains in clinical specimens and longer chains in laboratory media. The most common infection is pharyngitis (streptococcal sore throat) with the organism usually being limited to the mucous membranes and lymphatic tissue of the upper respiratory tract. S. pyogenes is responsible for 15-30% of cases of acute pharyngitis in children and 5-10% of cases in adults. Between 5% and 20% of children are asymptomatic carriers. Pharyngitis is pread person to person primarily by respiratory droplets; skin infections are spread by direct contact with an infected person or through fomites.
From the pharynx, however, the streptococci sometimes spread to other areas of the respiratory tract resulting in laryngitis, bronchitis, pneumonia, and otitis media (ear infection). Occasionally, it may enter the lymphatic vessels or the blood and disseminate to other areas of the body, causing septicemia, osteomyelitis, endocarditis, septic arthritis, and meningitis. It may also infect the skin, causing erysipelas, impetigo, or cellulitis.
Group A beta streptococcus infections can result in two autoimmune diseases, rheumatic fever and acute glomerulonephritis, where antibodies made against streptococcal antigens cross react with joint membranes and heart valve tissue in the case of rheumatic fever, or glomerular cells and basement membranes of the kidneys in the case of acute glomerulonephritis.
Streptococcal pyrogenic exotoxin (Spe), produced by rare invasive strains and scarlet fever strains of Streptococcus pyogenes (the group A beta streptococci). S. pyogenes produces a number of SPEs that are cytotoxic, pyrogenic, enhance the lethal effects of endotoxins, and contribute to cytokine-induced inflammatory damage. SPEs are responsible for causing streptococcal toxic shock syndrome (STSS) whereby excessive cytokine production leads to fever, rash, and triggering the shock cascade. The SPEs also appear to be responsible for inducing necrotizing fasciitis, a disease that can destroy the skin, fat, and tissue covering the muscle (the fascia). SPE B is also a precursor for a cysteine protease that can destroy muscles tissue.
CDC reports that approximately 9,000-11,500 cases of invasive GAS disease occur each year in the U.S., with STSS and necrotizing fasciitis each accounted for approximately 6-7% of the cases. STSS has a mortality rate of around 35%. The mortality rate for necrotizing fasciitis is approximately 25%.
For further information on virulence factors for group A beta Streptococci, see the following Learning Objects in your Lecture Guide:
The group B streptococci (GBS or Streptococcus agalactiae) usually show a small zone of beta hemolysis on Blood agar, although some strains are non-hemolytic. S. agalactiae isolates are Gram-positive cocci 0.6-1.2 µm in diameter that typically form short chains in clinical specimens and longer chains in laboratory media. They are found in the gastrointestinal tract and genitourinary tract of 15%-45% healthy woman. This reservoir, along with nosocomial transmission, provides the inoculum by which many infants are colonized at birth. The transmission rate from a mother colonized with GBS to her baby is thought to be around 50%. Most colonized infants (and adults) remain asymptomatic, however, an estimated 1-2% of neonates colonized will develop invasive GBS diseases, including pneumonia, septicemia, and/or meningitis. Pregnant women should be tested to determine if they are GBS carriers and be given IV antibiotics if they are a carrier
Other infections associated with group B streptococci include urinary tract infections, skin and soft tissue infections, osteomyelitis, endometritis, and infected ulcers (decubitus ulcers and ulcers associated with diabetes). In the immunocompromised patient it sometimes causes pneumonia and meningitis.
The group C streptococci (mainly S. equi, S. equisimilis and S. zooepidemicus) are beta hemolytic. They sometimes cause pharyngitis and, occasionally, bacteremia, endocarditis, meningitis, pneumonia, septic arthritis, and cellulitis. Group C streptococci are a common cause of infections in animals.
The group F streptococci (mainly S. anginosus) have been isolated from abscesses of the brain, mouth, and jaw. They also sometimes cause endocarditis.
The group G streptococci also show beta hemolysis. They sometimes cause pharyngitis and can also cause serious infections of the skin and soft tissues (mainly in the compromised host) as well as endocarditis, bacteremia, and peritonitis.
All of these beta hemolytic streptococci can be identified by biochemical testing and/or by serologic testing. Today you will look at the isolation and identification of group A beta streptococci (Streptococcus pyogenes) by biochemical testing. Serological identification will be performed in Lab 17.
ISOLATION AND IDENTIFICATION OF GROUP A BETA STREPTOCOCCI (Streptococcus pyogenes)
Videos reviewing techniques used in this lab:
Group A beta streptococci are usually isolated on Blood agar. Streptococcus pyogenes produces
1. Very small, white to grey colonies approximately 1mm in diameter.
2. A zone of beta hemolysis (see Fig. \(\PageIndex{1}\)) around 2-3mm in diameter surrounding each colony.
There are two streptococcal hemolysins, streptolysin S and streptolysin O. Streptolysin O can be inactivated by oxygen so more distinct hemolysis can be seen by stabbing the agar several times. In this way, some of the organisms form subsurface colonies growing away from oxygen. Since both streptolysin S and streptolysin O are active in the stabbed area, a more clear zone of beta hemolysis can be seen.
3. Sensitivity to the antibiotic bacitracin found in a Taxo A® disc.
Only the group A beta streptococci are sensitive to bacitracin, as shown by a zone of inhibition around a Taxo A® disc (see Fig. \(\PageIndex{1}\)), a paper disc containing low levels of bacitracin. Other serologic groups of streptococci are resistant to bacitracin and show no inhibition around the disc. (The Lancefield group of a group A beta streptococcus can also be determined by direct serologic testing as will be demonstrated in Lab 16.)
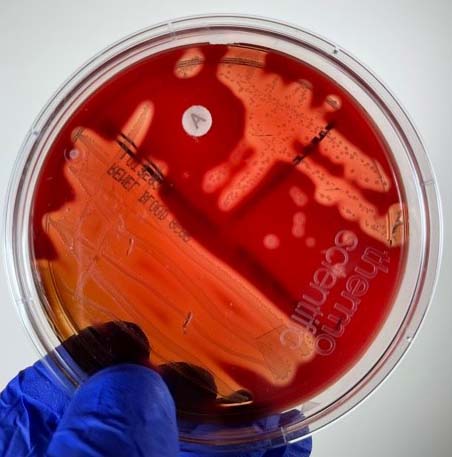
See Fig. \(\PageIndex{9}\) for a blood agar plate of a throat culture showing possible Streptococcus pyogenes.
Contributors and Attributions
Dr. Gary Kaiser (COMMUNITY COLLEGE OF BALTIMORE COUNTY, CATONSVILLE CAMPUS)

