53: Serology - Antigen-Antibody Tests
- Page ID
- 3703
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Learning Objectives
- To make a serological identification using Staphylococcus and Streptococcus
- To identify non-specific antibodies (heterophile antibodies) against Epstein-Barr virus
The surface of microorganisms is covered with physical features that can be recognized by the immune system. Any feature that can elicit an immune response is called an antigen. The immune system makes proteins called immunoglobulins or antibodies which bind to an antigen to either directly neutralize the antigen or cause it to be cleared more efficiently by other components of the immune system. Antibodies linked to large particles such as latex beads can be used to agglutinate microorganisms using specific reactive antibodies. Such agglutination is directly observable to the naked eye as a clumping reaction.
This exercise involves 2 kinds of serological tests---one for the identification of an unknown antigen and the other for the identification of an unknown antibody.
TESTING FOR ANTIBODY USING A KNOWN ANTIGEN
In the Monospot test a known Epstein-Barr viral antigen is used in the test, for the identification of patient antibody to this virus (which causes infectious mononucleosis, Burkitt's lymphoma, and nasopharyngeal cancer). The interesting thing about this test is that you are identifying NONSPECIFIC antibody rather than antibody against the Epstein-Barr virus, the cause of infectious mononucleosis. This odd antibody, called ‘heterophile' antibody reacts against sheep and bovine RBCs. The term heterophile antibody refers to antibodies having the capacity to react with certain antigens, which are very different from the ones inducing the antibody formation. The latex particles in the MONO-LATEX REAGENT LATEX are coated with a suspension of mononucleosis antigen obtained from red blood cells from cattle. If antibodies are present in the serum or plasma and mixed with the latex, a specific reaction will result in a visible agglutination of the latex particles. The patient serum, a NEGATIVE control, and a POSITIVE control are each placed on the glass slide, then adding the reagent LATEX (plastic beads covered with antigen).
TESTING FOR ANTIGEN USING A KNOWN ANTIBODY
Another way to use serological testing is for the identification of the antigen itself, using a known specific antibody for that antigen: You will see 2 methods in lab. The older, more reliable way of identifying Strep and Staph bacteria is by growth on agar media, as well as biochemical or antibiotic testing. This type of identification takes 1-2 days.
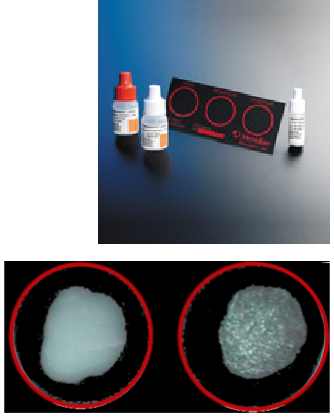
A latex-conjugated antibody (Difco® Staph Latex-kitor Staphyloslide kit) can be used to confirm the presence of Staphylococcus aureus. This is a good confirmation of S. aureus that has been presumptively identified by biochemical and physical testing. It differentiates Staphylococci which possess clumping factor and/or Protein A, Blue latex powder pre-coated with the antibody to Staph aureus is mixed with a Staph culture. If the specific antigen of Staph aureus is present, it will react with the latex-antibody, producing a noticeable agglutination (which is more easily seen with the blue of the latex). That is the only function of the blue latex.
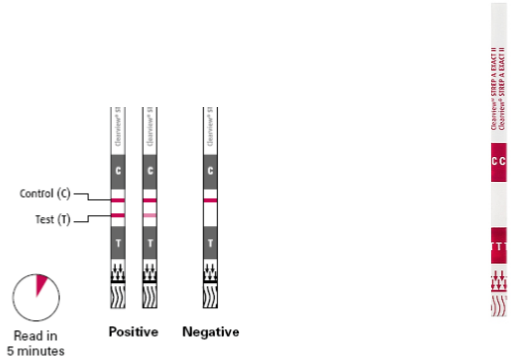
Another test used today will be the Clearview Exact Strep dipstick, a rapid test used to detect Strep (strep throat) antigen directly from throat swabs. It is an immunoassay test, consisting of a strip that has been precoated with anti-Strep antibody plus another Strep antibody that is colored with gold. The Strep from the patient’s mouth is on a cotton swab, and the Strep antigen is then extracted with extraction reagents. The test strip is inserted into this antigen reagent mixture and the mixture moves chromatographically up the teststrip, attaching to the antibody. This antigen-antibody complex then binds with the second Strep antibody (bound to gold), forming a ‘sandwich.’ A colored ‘sandwich’ of antibody-antigen-antibody-gold is formed on the test lines, showing up as a pink line.
MATERIALS NEEDED
- A Staphylococcus culture on an agar medium plate
- A Streptococcus culture on an agar medium plate
- Difco Staph latex-kit or Staphyloslide kit
- Clearview test for Streptoccus
- Monospot test kit for Epstein-Barr virus
THE PROCEDURES: will be performed by instructor as demo for the class
Serological typing of Staphylococcus aureus
- Mix the latex reagent by shaking; expel any latex from the dropper for complete mixing.
- Dispense 1 drop of Test Latex (contains Staph antibody) onto one of the circles on the reaction card and add 1 drop of Control Latex onto another circle.
- Using a loop, pick up and smear 5 suspect colonies (either a suspect Staph from your body OR a known Staph aureus supplied from the lab) onto the Test Latex-containing circle and mix this into the Test Latex reagent. Spread to cover the circle. Be sure you have a homogenous bacterial suspension. Clumps will make the reaction difficult to identify, and possibly give a false + reaction.
- Repeat step 3 for the Control Latex, using the same bacterial culture.
- Pick up and hand rock the card for up to 20 sec and observe for agglutination under normal lighting conditions.
- Rock the slide back and forth for no longer than one minute and look for blue agglutination. Clumping is a positive reaction for the identification of S. aureus.
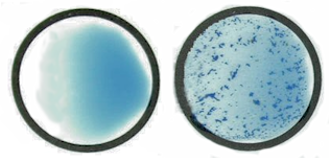
Clearview test for Streptococcal antigen
- Place the Extraction Tube in the tube holder. Add 3 drops of Extraction Reagent 1 to the Extraction Tube. Add 3 drops of Extraction Reagent 2 to the Extraction Tube.
- Place the throat swab specimen in the Extraction Tube. Rotate the swab inside the tube using a circular (you may use the pure culture of Strep provided) motion to roll against the side of the Extraction Tube so that liquid is expressed and reabsorbed from the swab. Let it stand for a minimum of 1 minute.
- Gently squeeze the swab firmly against the tube to expel as much liquid as possible from the swab. Discard the swab.
- Immerse the test strip into the Extraction Tube with the arrows pointing towards the specimen extract. Leave the test strip in the Extraction Tube. Start the timer.
- Read results in 5 minutes. Depending on the number of organisms on the swab, a positive result may be visible as soon as 1 minute. However, to confirm a negative result the complete reaction time of 5 minutes is required. Do not read results after 10 minutes.
Monospot test
 Place a free-falling drop of NEGATIVE control serum on the glass slide.
Place a free-falling drop of NEGATIVE control serum on the glass slide.- Place a free-falling drop of POSITIVE control serum on the glass slide in a different well. Since we don't have patient serum, you will use the positive control serum as the patient's serum.
- Add 1 free-falling drop of the reagent LATEX to each well.
- Mix the contents of each circle with a stirrer (different stirrers for each circle), covering the entire surface of the circle.
- Rock the slide in a circular motion for 2 minutes.
- Observe for agglutination. A light held directly over the slide will improve the readability of the test.
QUESTIONS
- Why feature of antibodies results in a positive test causing clumping?
- Why are the antibodies attached to latex particles for this type of test?
- For each of the above tests run in lab, is the test identifying a specific antigen or a specific antibody?
- What are heterophile antibodies?
Contributors and Attributions
Jackie Reynolds, Professor of Biology (Richland College)

