7.6: Blood Types
- Last updated
- Save as PDF
- Page ID
- 30663
Giving the Gift of Life
Did you ever donate blood as the individual in Figure \(\PageIndex{1}\) is doing? If you did, then you probably know that your blood type is an important factor in blood transfusions. People vary in the type of blood they inherit, and this determines which type(s) of blood they can safely receive in a transfusion. Do you know your blood type?
What Are Blood Types?
Blood type (or blood group) is a genetic characteristic associated with the presence or absence of certain molecules, called antigens, on the surface of red blood cells. These molecules may help maintain the integrity of the cell membrane, act as receptors, or have other biological functions. A blood group system refers to all of the gene(s), alleles, and possible genotypes and phenotypes that exist for a particular set of blood type antigens. Human blood group systems include the well-known ABO and Rhesus (Rh) systems, as well as at least 33 others that are less well known.
Antigens and Antibodies
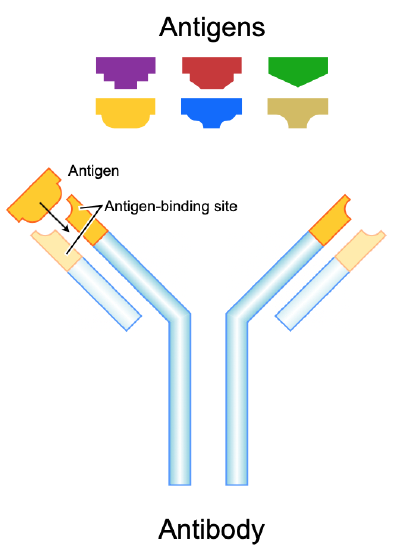
Antigens such as those on the red blood cells are molecules that the immune system identifies as either self (produced by your own body) or non-self (not produced by your own body). Blood group antigens may be proteins, carbohydrates, glycoproteins (proteins attached to chains of sugars), or glycolipids (lipids attached to chains of sugars), depending on the particular blood group system. If antigens are identified as nonself, the immune system responds by forming antibodies that are specific to the non-self antigens. Antibodies are large, Y-shaped proteins produced by the immune system that recognize and bind to non-self antigens. The analogy of a lock and key is often used to represent how an antibody and antigen fit together, as shown in Figure \(\PageIndex{2}\). When antibodies bind to antigens, it marks them for destruction by other immune system cells. Nonself antigens may enter your body on pathogens such as bacteria or viruses, on foods, or on red blood cells in a blood transfusion from someone with a different blood type than your own. The last way is virtually impossible nowadays because of effective blood typing and screening protocols.
Genetics of Blood Type
An individual’s blood type depends on which alleles for a blood group system were inherited from their parents. Generally, blood type is controlled by alleles for a single gene or for two or more very closely linked genes. Closely linked genes are almost always inherited together because there is little or no recombination between them. Like other genetic traits, a person’s blood type is generally fixed for life, but there are rare instances in which blood type can change. This could happen, for example, if an individual receives a bone marrow transplant to treat a disease such as leukemia. If the bone marrow comes from a donor who has a different blood type, the patient’s blood type may eventually convert to the donor’s blood type because red blood cells are produced in the bone marrow.
ABO Blood Group System
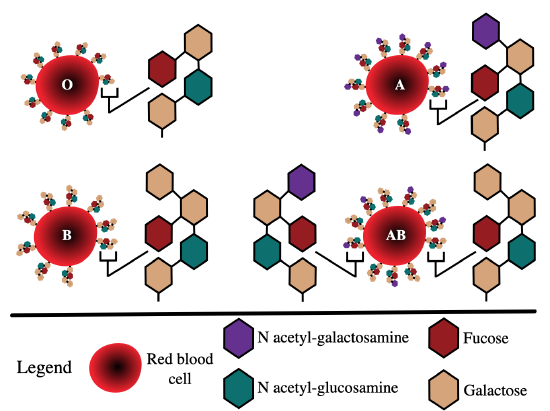
The ABO blood group system is the best known human blood group system. Antigens in this system are glycoproteins. These antigen compounds are shown in Figure \(\PageIndex{3}\). There are four common blood types for the ABO system:
- Type A, in which only the A antigen is present
- Type B, in which only the B antigen is present
- Type AB, in which both the A and B antigens are present
- Type O, in which neither the A nor the B antigen is present
Genetics of the ABO System
The ABO blood group system is controlled by a single gene on chromosome 9. There are three common alleles for the gene, often represented by the letters IA (or A), IB (or B), and i (or O). With three alleles, there are six possible genotypes for the ABO blood group. However, alleles IA and IB are both dominant to allele i and codominant to each other. This results in just four possible phenotypes (blood types) for the ABO system. These genotypes and phenotypes are shown in Table \(\PageIndex{1}\).
Table \(\PageIndex{1}\): ABO Blood Group System
| Genotype | Phenotype (Blood Type, or Group) |
|---|---|
| \(I^Ai\) | A |
| \(I^AI^A\) | A |
| \(I^AI^B\) | AB |
| \(I^Bi\) | B |
| \(I^BI^B\) | B |
| \(ii\) | O |
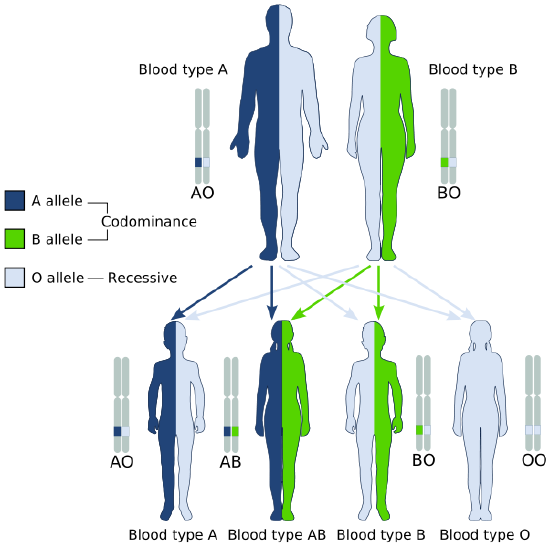
The diagram in Figure \(\PageIndex{4}\) shows an example of how ABO blood type is inherited. In this particular example, the father has blood type A (genotype AO) and the mother has blood type B (genotype BO). This mating type can produce children with each of the four possible ABO phenotypes, although in any given family not all phenotypes may be present in the children.
Medical Significance of ABO Blood Type
The ABO system is the most important blood group system in blood transfusions. If red blood cells containing a particular ABO antigen are transfused into a person who lacks that antigen, the person’s immune system will recognize the antigen on the red blood cells as non-self. Antibodies specific to that antigen will attack the red blood cells, causing them to agglutinate, or clump and break apart. If a unit of incompatible blood were to be accidentally transfused into a patient, a severe reaction (called acute hemolytic transfusion reaction) is likely to occur in which many red blood cells are destroyed. This may result in kidney failure, shock, and even death. Fortunately, such medical accidents virtually never occur today.
ABO antibodies are likely to already be present in a recipient’s blood for antigens that the person lacks. These antibodies are produced in the first years of life by sensitization to similar antigens commonly occurring in the environment. Anti-A antibodies are thought to originate from an immune response to an antigen on the influenza virus, and anti-B antibodies are thought to originate from an immune response to an antigen found on bacteria such as E. coli. Once the antibodies have been produced, they circulate in the plasma. The relationship between ABO red blood cell antigens and plasma antibodies is shown in Table \(\PageIndex{2}\).
| Blood group | A | B | AB | O |
|---|---|---|---|---|
| Antibodies in plasma | Anti-B | Anti-A | None | Anti-A and Anti-B |
| Antigens on the red blood cell | A antigen | B antigen | A and B antigen | None |
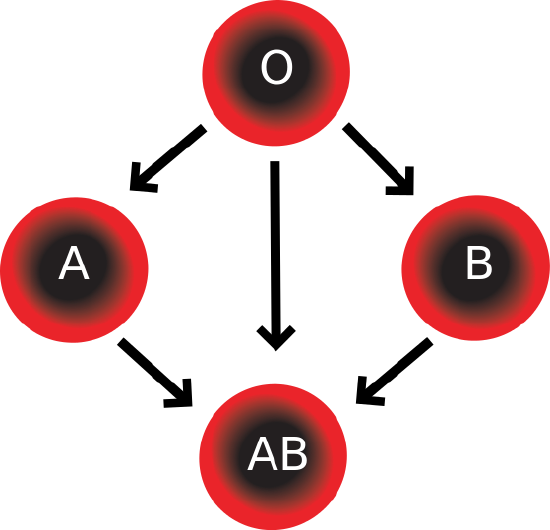
Which blood types are compatible and which are not? Type O blood contains both anti-A and anti-B antibodies, so people with type O blood can only receive type O blood. However, they can donate blood to people of any ABO blood type. That’s why individuals with type O blood are called universal donors. Type AB blood contains neither anti-A nor anti-B antibodies, so people with type AB blood can receive blood from people of any ABO blood type. That’s why individuals with type AB blood are called universal recipients. However, they can donate blood only to people who also have type AB blood. These and other relationships between blood types of donors and recipients are summarized in Figure \(\PageIndex{5}\).
ABO blood type antigens are found not only on red blood cells but also on platelets, in other body fluids such as tears and urine, and on cells of other types of tissues. Blood type compatibility is important to consider for successful organ transplantation. If a transplanted organ has nonself antigens for ABO, it may be attacked by antibodies and rejected by the body.
Rhesus Blood Group System
Another well-known blood group system is the Rhesus (Rh) blood group system. The Rhesus system has dozens of different antigens but only five main antigens (named D, C, c, E, and e). The major Rhesus antigen is the D antigen. People with the D antigen are called Rh-positive (Rh+), and people who lack the D antigen are called Rh-negative (Rh-). Rhesus antigens are thought to play a role in transporting ions across cell membranes by acting as channel proteins.
The Rhesus blood group system is controlled by two linked genes on chromosome 1. One gene, called RHD, produces a single antigen, antigen D. The other gene, called RHCE, produces the other four relatively common Rhesus antigens (C, c, E, and e), depending on which alleles for this gene are inherited.
Rhesus Blood Group and Transfusions
After the ABO system, the Rhesus system is the second most important blood group system in blood transfusions. The D antigen is the one most likely to provoke an immune response in people who lack the antigen. People who have the D antigen (Rh+) can be safely transfused with either Rh+ or Rh- blood, whereas people who lack the D antigen (Rh-) can be safely transfused only with Rh- blood.
Unlike anti-A and anti-B antibodies to ABO antigens, anti-D antibodies for the Rhesus system are not usually produced by sensitization to environmental substances. However, people who lack the D antigen (Rh-) may produce anti-D antibodies if exposed to Rh+ blood. This may happen accidentally in a blood transfusion, although this is extremely unlikely today. It may also happen during pregnancy with an Rh+ fetus if some of the fetal blood cells pass into the mother’s blood circulation.
Hemolytic Disease of the Newborn
If a woman who is Rh- is carrying an Rh+ fetus, the fetus may be at risk. This is especially likely if the mother has formed anti-D antibodies during a prior pregnancy because of a mixing of maternal and fetal blood during childbirth. Unlike antibodies against ABO antigens, antibodies against the Rhesus D antigen can cross the placenta and enter the blood of the fetus. This may cause hemolytic disease of the newborn (HDN), also called erythroblastosis fetalis, an illness in which fetal red blood cells are destroyed by maternal antibodies, causing anemia. This illness may range from mild to severe. If it is severe, it may cause brain damage and is sometimes fatal for the fetus or newborn. Fortunately, HDN can be prevented by preventing the formation of anti-D antibodies in the Rh- mother. This is achieved through an injection into the mother of a medication called Rho(D) immune globulin.
Feature: Myth vs. Reality
Myth: Your nutritional needs can be determined by your ABO blood type. Knowing your blood type allows you to choose the appropriate foods that will help you lose weight, increase your energy, and live a longer, healthier life.
Reality: This idea was proposed in 1996 in a New York Times bestseller Eat Right for Your Type, by Peter D’Adamo, a naturopath. Naturopathy is a method of treating disorders that involve the use of herbs, sunlight, fresh air, and other natural substances. Some medical doctors consider naturopathy a pseudoscience. A major scientific review of the blood type diet could find no evidence to support it. In one study, adults eating the diet designed for blood type A showed improved health, but this occurred in everyone regardless of their blood type. Because the blood type diet is based solely on blood type, it fails to account for other factors that might require dietary adjustments or restrictions. For example, people with diabetes but different blood types would follow different diets, and one or both of the diets might conflict with standard diabetes dietary recommendations and be dangerous.
Myth: ABO blood type is associated with certain personality traits. For example, people with blood type A are patient and responsible but may also be stubborn and tense, whereas people with blood type B are energetic and creative but may also be irresponsible and unforgiving. In selecting a spouse, both your own and your potential mate’s blood type should be taken into account to ensure the compatibility of your personality.
Reality: The belief that blood type is correlated with personality is widely held in Japan and other East Asian countries (the Japanese booth pictured below offers fortunes based on blood type). The idea was originally introduced in the 1920s in a study commissioned by the Japanese government but later shown to have no scientific support. The idea was revived in the 1970s by a Japanese broadcaster who wrote popular books about it. There is no scientific basis for the idea, and it is generally dismissed as pseudoscience by the scientific community. Nonetheless, it remains popular in East Asian countries, like astrology in many other countries.
Review
- Define blood type and blood group system.
- Explain the relationship between antigens and antibodies.
- Identify the alleles, genotypes, and phenotypes in the ABO blood group system.
- Discuss the medical significance of the ABO blood group system.
- Give examples of how different ABO blood types vary in their susceptibility to diseases.
- Describe the Rhesus blood group system.
- Relate Rhesus blood groups to blood transfusions.
- What causes hemolytic disease of the newborn?
- A woman is blood type O and Rh- and her husband is blood type AB and Rh+. Answer the following questions about this couple and their offspring.
a. What are the possible genotypes of their offspring in terms of ABO blood group?
b. What are the possible phenotypes of their offspring in terms of ABO blood group?
c. Can the woman donate blood to her husband? Explain your answer.
d. Can the man donate blood to his wife? Explain your answer.
- True or False. The D antigen is part of the ABO blood group system.
- Explain why hemolytic disease of the newborn may be more likely to occur in a second pregnancy than in a first.
Explore More
Is malaria the reason so many people have type O blood? Listen to this fascinating National Public Radio interview with Dr. Christine Cserti-Gazdewich, a blood specialist (hematologist) at the University of Toronto, who discusses an emerging theory of universal blood. If you click on the icon of the podcast, you will find the transcript on their site.
Attributions
- Offutt blood drive by Charles Haymond; public domain via Wikimedia Commons
- Antibody by Fvasconcellos; public domain via Wikimedia Commons
- ABO blood group diagram by InvictaHOG; public domain via Wikimedia Commons
- ABO system codominance by NIH; public domain via Wikimedia Commons
- Blood compatibility by InvictaHOG; public domain via Wikimedia Commons
- Text adapted from Human Biology by CK-12 licensed CC BY-NC 3.0


