9.3: Cardiovascular Disease
- Page ID
- 191881
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Eating this greasy cheeseburger smothered in bacon may not literally cause a heart attack. However, regularly eating high-fat, low-fiber foods such as this may increase the risk of a heart attack or other type of cardiovascular disease. In fact, unhealthy lifestyle choices such as this may account for as many as 90 percent of cases of cardiovascular disease.

What Is Cardiovascular Disease?
Cardiovascular disease includes
- diseases of the coronary arteries that supply the heart muscle with oxygen and nutrients
- diseases of arteries such as the carotid artery that provide blood flow to the brain, and
- diseases of the peripheral arteries that carry blood throughout the body.
Worldwide, cardiovascular disease is the leading cause of death, causing about 33% of all deaths each year.
Most cases of cardiovascular disease are in those over 60, with onset typically beginning in their 50s. It occurs earlier in men than in women. It also occurs at higher rates among underresourced groups, as healthy food options may be hard to find and regular exercise may be difficult to maintain. They also often receive poorer quality of care due to stigma, lack of healthcare providers’ awareness, and insensitivity to the unique needs of their communities.
While genetics, social, political, and other external factors are extremely challenging to adapt to, other factors that increase the risk of cardiovascular disease can be controlled. Ways to prevent cardiovascular disease or keep it from progressing include:
- Don't smoke.
- Maintain as healthy a weight as possible
- Eat as many healthy foods as possible.
- Take medications as needed to control diagnosed diabetes and cholesterol
- Get exercise (especially cardiovascular) when possible
It should be noted that high blood lipid levels (LDL, cholesterol, and triglycerides) are definitely risk factors for cardiovascular disease. HDL is "good" cholesterol and higher levels lowers risk of cardiovascular disease.
Interestingly, studies of high-cholesterol diets do not support a direct correlation with elevated blood cholesterol levels. Clearly, cardiovascular disease is multifactorial in terms of its causes.
Precursors of Cardiovascular Disease
Two very common conditions are precursors to virtually all cases of cardiovascular disease: hypertension (high blood pressure) and atherosclerosis (hardening of the arteries).
Hypertension
Hypertension is when blood pressure in the arteries is persistently elevated (Table \(\PageIndex{1}\)).
It usually does not cause symptoms. Many people with high blood pressure are unaware of their condition unless their blood pressure is measured during a physical or medical visit for another health problem. More than 50% of all women have hypertension, but it goes undiagnosed and is known as a "silent killer".
| Category | Systolic (mm Hg) | Diastolic (mm Hg) |
|---|---|---|
| Normal blood pressure | 90-119 | 60-79 |
| Prehypertension | 120-139 | 80-89 |
| Hypertension | 140 or higher | 90 or higher |
Hypertension is either primary (90% of cases) or secondary.
Primary hypertension, in addition to the numerous genes that have cumulative, small effects on blood pressure, is impacted by lifestyle factors that increase the risk, including excess dietary salt and alcohol consumption.
Secondary high blood pressure is attributable to chronic kidney disease or an endocrine disorder (e.g., Cushing’s disease).
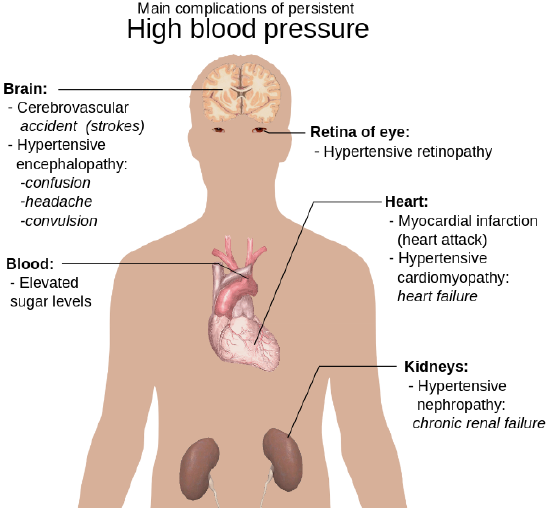
Treating hypertension is important to reduce all cardiovascular disease risk, especially stroke, and other complications (Figure \(\PageIndex{2}\)).
Lifestyle changes, including a reduced-salt, healthier diet, may be all that is needed to lower blood pressure to normal. In many cases, however, medications are also required.
Dr. Elizabeth Grey discusses the new blood pressure guidelines, treatment of hypertension, and risk correlation.
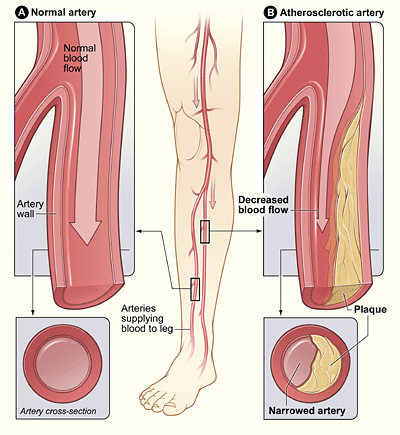
Atherosclerosis
In atherosclerosis, arterial walls thicken and stiffen due to the buildup of plaques within the arteries. Plaques consist of white blood cells, cholesterol, and other fats. The formation of plaques may be due to a buildup of LDL in the vessels, leading to inflammation. Typically, there is also a proliferation of smooth muscle cells, making the plaque both fibrous and fatty. In most people, plaques form in arteries during childhood and progress over time. Individuals may develop just a few plaques or dozens.
Over time, the plaques may harden as calcium crystals accumulate, reducing the elasticity of the artery walls. As plaques enlarge, the arteries dilate to compensate and maintain blood flow.
Eventually, however, the arteries are likely to become so narrowed by plaque (stenosis) that blood flow is reduced or even blocked (Figure \(\PageIndex{3}\)).
Plaques typically remain asymptomatic for decades. Signs and symptoms appear only after stenosis or complete arterial blockage:
- The formation of blood clots is common, which may also plug arteries at the site of the plaque or travel elsewhere in the circulation.
- Sometimes plaques rupture or become detached from an arterial wall and become lodged in a smaller, downstream artery.
- Blockage of arteries by plaques or clots may cause a heart attack, stroke, or other potentially life-threatening cardiovascular events.
- If blood flow to the kidneys is affected, it may lead to chronic kidney disease.
Risk factors for the development of atherosclerosis include hypertension, high cholesterol (especially LDL cholesterol), diabetes, and smoking. The chance of developing atherosclerosis increases with age and a family history of cardiovascular disease. It is more common in men.
Treatment of atherosclerosis often includes both lifestyle changes and medications to lower cholesterol, control blood pressure, and reduce the risk of blood clot formation. In extreme cases or when other treatments are inadequate, surgery may be recommended. Surgery may involve placing stents in arteries to keep them open and improve blood flow, or using grafts to divert blood flow around blocked arteries.
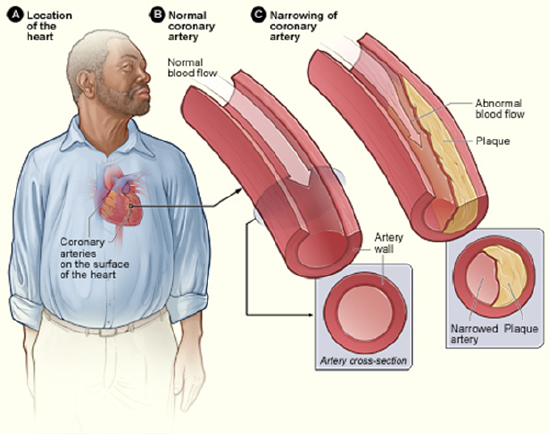
Coronary Artery Disease
Coronary artery disease results from atherosclerosis of the coronary arteries. Treatment of the diseases mainly involves treating underlying atherosclerosis. Two of the most common coronary artery diseases are angina and myocardial infarction.
Angina
Angina (stable or unstable) is chest pain or pressure occurring when heart muscle cells do not receive adequate blood flow (ischemia) (Figure \(\PageIndex{4}\)). It may be accompanied by pain in the back, neck, shoulders, or jaw. In some cases, there may be shortness of breath, sweating, or nausea. Treatment of angina involves relieving the symptoms and slowing the progression of underlying atherosclerosis.
- Stable angina results from exertion (e.g., brisk walking or running) and improves quickly with rest or nitroglycerin, a medication that dilates the coronary arteries and improves blood flow. Stable angina may develop into unstable angina.
- Unstable angina occurs during rest, lasts more than 15 minutes, and is of new onset. This type of angina is more dangerous and may be a sign of an imminent heart attack, requiring urgent medical attention.
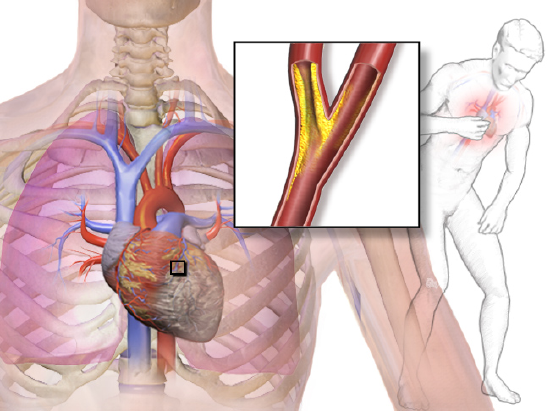
Myocardial Infarction
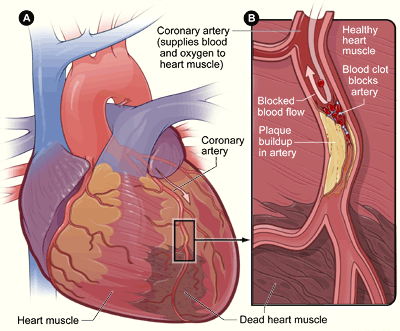
A myocardial infarction (MI), or heart attack, occurs when blood flow stops to a part of the heart. This causes damage to the heart muscle and the death of heart cells. An MI usually occurs because of a complete coronary artery blockage, often due to a blood clot or the rupture of a plaque (Figure \(\PageIndex{5}\)).
An MI typically causes chest pain and pressure, among other possible symptoms, but at least 25% of MIs are asymptomatic.
If the patient survives, an MI often causes permanent damage to the heart. This puts the heart at risk of heart arrhythmias, heart failure, and cardiac arrest.
- Heart arrhythmias are abnormal heart rhythms, which are potentially life-threatening. Heart arrhythmias can often be interrupted with a cardiac defibrillator, which delivers an electrical shock to the heart, effectively “rebooting” it.
- Heart failure occurs when the heart's pumping action is impaired, and tissues do not receive adequate oxygen. This is a chronic condition that tends to get worse over time, although it can be managed with medications.
- Cardiac arrest occurs when the heart no longer pumps blood or pumps blood so poorly that vital organs can no longer function. This is a medical emergency requiring immediate intervention.
In the worst case, an MI may cause sudden death.
Megan Corbin, a 31-year-old dance studio owner and instructor, did not realize her excruciating back pain was a sign of a heart attack.
Other Cardiovascular Diseases
Hypertension and atherosclerosis often cause other cardiovascular diseases. These commonly include stroke and peripheral artery disease.
Stroke
A stroke occurs when blocked or ruptured arteries in the brain cause the death of brain cells, leading to a loss of normal function. It is the leading cause of disability in the United States.
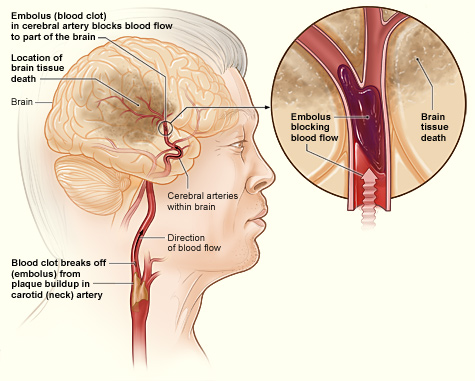
- An ischemic stroke (90% of strokes) occurs when an embolus (blood clot) breaks off from a plaque or forms in the heart due to arrhythmia (Figure \(\PageIndex{6}\)). The embolus travels to the brain, becoming lodged in an artery and blocking blood flow to part of the brain. Treatment with a clot-busting drug within a few hours of the stroke may prevent permanent damage. Almost 90 percent of strokes are ischemic strokes.
- A hemorrhagic stroke occurs when an artery in the brain ruptures and causes bleeding in the brain, depriving tissues downstream of adequate blood flow and putting pressure on brain tissue. Surgery to temporarily open the cranium may be required to relieve the pressure. These are more likely to be fatal than ischemic strokes.
Signs and symptoms of stroke may include:
- an inability to move, feel, or see on one side of the body
- problems understanding speech or difficulty speaking
- memory problems
- confusion
- dizziness.
- hemorrhagic strokes may cause a severe headache.
Symptoms of a stroke usually occur within seconds or minutes of the brain injury and are temporary or permanent, depending on the severity of the stroke. If the symptoms of a stroke go away on their own in less than an hour or two, the stroke is called a transient ischemic attack.
Rehabilitation with physical, occupational, speech, or other types of therapy may significantly improve functioning.
Maintaining a normal blood pressure with lifestyle changes or medications is the best way to reduce the risk of stroke. Another possible cause of stroke is the use of illicit drugs such as amphetamines or cocaine. Having had a stroke in the past greatly increases one’s risk of future strokes. Men are also more likely than women to have strokes.
Peripheral Artery Disease
Peripheral artery disease (PAD) is atherosclerosis in arteries other than the coronary or those supplying the brain (Figure \(\PageIndex{7}\)).
PAD most commonly affects the legs, but other arteries may also be involved.
Symptoms include
- leg pain when walking, usually resolving with rest (most common)
- skin ulcers
- bluish skin
- cold skin
- poor nail and hair growth in the affected leg(s).
Up to 50% all cases of PAD do not have any symptoms.
The main risk factors for PAD are smoking, diabetes, high blood pressure, and high blood cholesterol.
PAD is typically diagnosed when blood pressure readings taken at the ankle are lower than blood pressure readings taken at the upper arm. People with PAD have a 4-5 times greater risk of myocardial infarction or stroke.
Surgery to expand the affected arteries or to graft vessels in order to bypass blockages may be recommended in some cases.