7.5: The Thyroid Gland
- Page ID
- 191395
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Thyroid Structure and Function
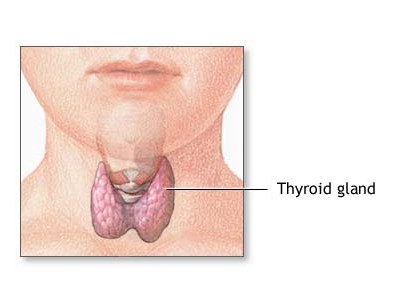
The thyroid gland is one of the largest endocrine glands in the body. It is located in the front of the neck below Adam’s apple, is butterfly-shaped, and composed of two lobes (Figure \(\PageIndex{1}\)). The lobes are connected by a narrow band of thyroid tissue called an isthmus.
Like all endocrine glands, the thyroid gland synthesizes hormones and secretes them into the bloodstream. Once in the blood, they can travel to cells throughout the body and influence their functions.
Internally, the thyroid gland is composed mainly of follicles. A follicle is a small cluster of cells surrounding a central cavity, which stores hormones and other molecules made by the follicular cells.
Thyroid follicular cells are unique in being highly specialized to absorb and utilize iodine (I-) from the blood to produce thyroid hormones. The cells also use some of the iodide they absorb to form a protein called thyroglobulin, which stores iodide for later hormone synthesis.
The outer layer of cells of each follicle secretes thyroid hormones as needed. Scattered among the follicles are another type of thyroid cells, called parafollicular cells (or C cells). These cells synthesize and secrete the hormone calcitonin.
Thyroid Hormones: T4 and T3
There are two main thyroid hormones produced by the follicles: thyroxine (T4) and triiodothyronine (T3). T3 is much more potent than T4, but T4 accounts for about 90% of circulating thyroid hormone. Most of the T4 is converted to T3 by target tissues.
T3 and T4 cross cell membranes everywhere in the body. However, unlike steroid hormones, thyroid hormones can cross cell membranes only with the help of special transporter proteins.
Once inside the cell nucleus, thyroid hormones increase the rate of cellular metabolism, so cells absorb more carbohydrates, use more energy, and produce more heat. They also increase the rate and force of the heartbeat. Finally, they increase cells' sensitivity to fight-or-flight hormones, such as catecholamines, including adrenaline.
- T4 and T3 production is regulated primarily by thyroid-stimulating hormone (TSH) (Figure \(\PageIndex{2}\)).
- TSH production, in turn, is regulated by thyrotropin-releasing hormone (TRH), which is produced by the hypothalamus.
- The thyroid gland, pituitary gland, and hypothalamus form a negative feedback loop to keep thyroid hormone secretion within a normal range.
- TRH and TSH production are suppressed when T4 levels start to become too high.
- The opposite occurs when T4 levels start to become too low.

Calcitonin
Parafollicular cells of the thyroid gland help regulate blood calcium levels by stimulating the movement of calcium into bone via the hormone calcitonin.
Calcitonin is secreted in response to rising blood calcium levels. It decreases blood calcium levels by enhancing calcium absorption and deposition in bone.
Calcitonin works hand in hand with parathyroid hormone, which is secreted by the parathyroid glands and has the opposite effects. Together, these two hormones maintain calcium homeostasis.
Thyroid Disorders
As with other endocrine disorders, thyroid disorders are generally associated with either over- or under-secretion of hormones. Abnormal secretion of thyroid hormones may occur for various reasons.
Hyperthyroidism
Hyperthyroidism occurs when the thyroid gland produces excessive amounts of thyroid hormones.
Signs and symptoms of hyperthyroidism can include a goiter, protruding eyes (Figure \(\PageIndex{3}\)), heart palpitations, excessive sweating, diarrhea, weight loss despite increased appetite, muscle weakness, and unusual sensitivity to heat.
Medications can be prescribed to mitigate the symptoms of the disease. Anti-thyroid drugs can also be given to decrease the production of thyroid hormones. If the drugs are ineffective, the gland can be partially or entirely removed. This can be done surgically or with the administration of radioactive iodine. Removal of the thyroid produces hypothyroidism.

The most common cause of hyperthyroidism is Graves’ disease, an autoimmune disorder in which abnormal antibodies produced by the immune system stimulate the thyroid to secrete excessive quantities of its hormones.
This stimulation overrides the usual negative feedback mechanism that normally controls thyroid hormone output.
Graves’ disease often results in the formation of an enlarged thyroid (goiter) because of the continued stimulation to produce more hormones.
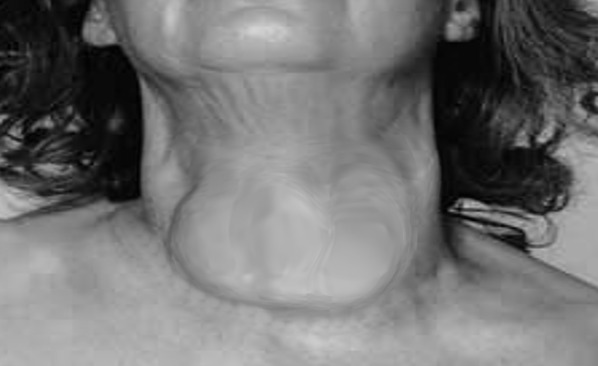
Figure \(\PageIndex{4}\): An example of a goiter caused by Grave's disease. Goiter in a Woman, S Bhimji, MD CC-BY-NC-ND 4.0
Hypothyroidism
Hypothyroidism occurs when the thyroid gland produces insufficient thyroid hormone. The most common cause worldwide is dietary iodine deficiency, but this is uncommon in the Western world because iodine is added to salt. It can also result from Hashimoto’s thyroiditis.
In cases of iodine deficiency, the negative feedback loop controlling thyroid hormone release leads to repeated stimulation of the thyroid. This results in the thyroid gland enlarging and forming a goiter. Although the gland enlarges, it cannot increase hormone output because of iodine deficiency in the diet.
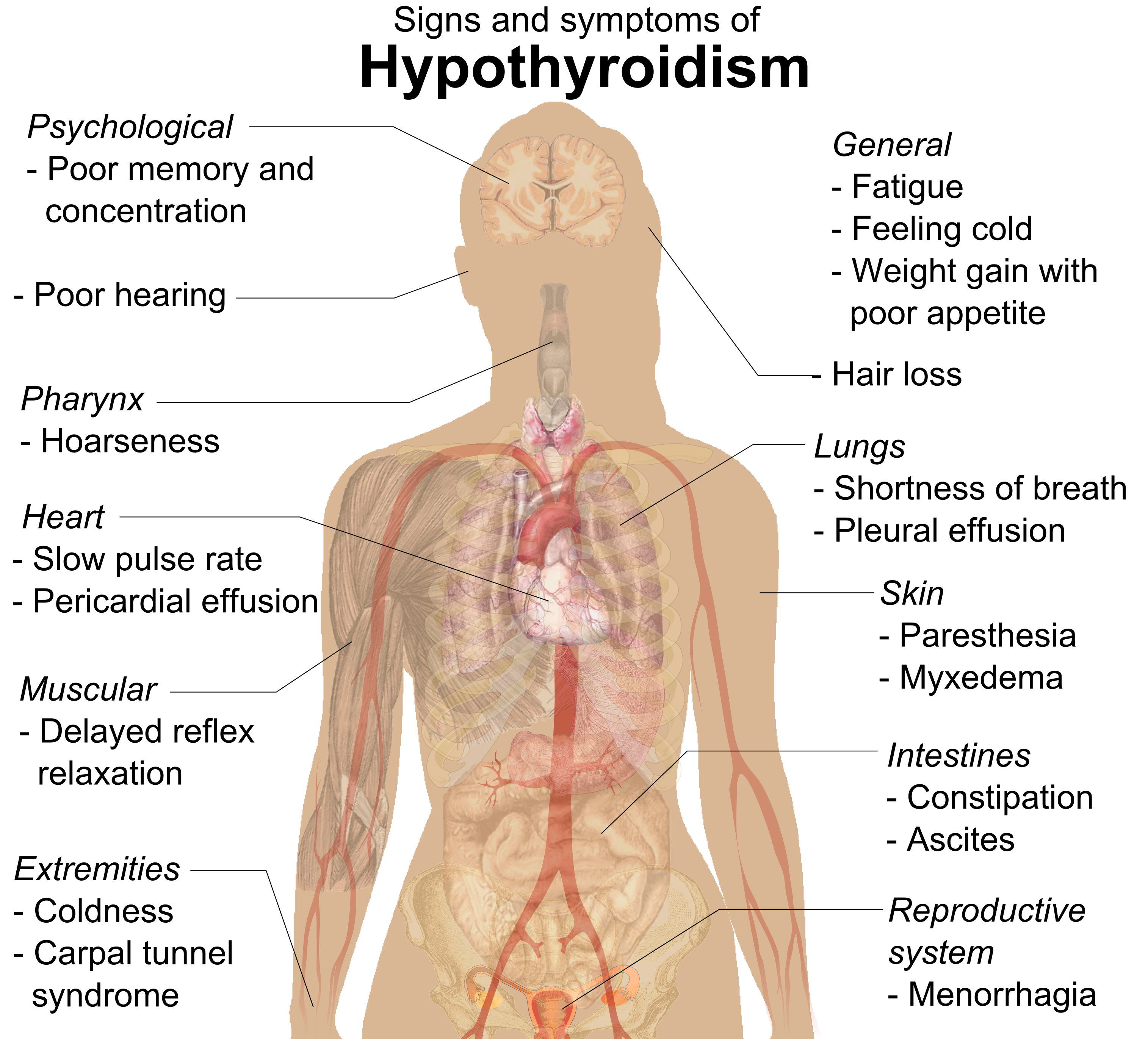
Hypothyroidism produces many signs and symptoms (Figure \(\PageIndex{4}\), including fatigue, cold intolerance, abnormal weight gain, shortness of breath, baldness, constipation, menorrhagia, poor memory and hearing, hoarseness, slow heart rate, delayed reflexes, and carpal tunnel syndrome.
Hypothyroidism is generally treated with thyroid hormone replacement therapy (Synthroid), which may be needed for the rest of a person’s life.
Hypothyroidism in a pregnant woman can have serious adverse consequences for the fetus. During the fetal period, cells of the developing brain are a major target for thyroid hormones, which play a crucial role in brain maturation. When thyroid hormone levels are too low, the fetus may suffer permanent deficits in cognitive abilities. Deafness is also a potential outcome of hypothyroidism in utero.
Where iodine deficiency is not a problem, the most common cause of hypothyroidism is Hashimoto’s thyroiditis.
In this autoimmune disease, the immune system attacks the thyroid gland, leading to hypothyroidism.
Hashimoto’s thyroiditis tends to run in families, suggesting a genetic component. It usually appears after age 30 and is more common in females than in males.
Thyroid disorders are relatively common, affecting as many as 20 million people in the United States. Because the disorders are common, there are also many common myths about them.
Myth: If you have a thyroid problem, you will know something is wrong because you will have obvious symptoms.
Reality: The majority of people with a thyroid disorder are not aware they have it because the symptoms are often mild, nonspecific, and easy to ignore. Generally, thyroid hormone blood tests are needed to make a conclusive diagnosis.
Myth: If you are diagnosed with a thyroid disorder, you will have to take medication for the rest of your life.
Reality: Whether you need to continue thyroid medication for life depends on the cause of the disorder. For example, some women develop hypothyroidism during pregnancy but no longer need medication after the pregnancy is over and hormone levels return to normal.
Myth: As soon as you start taking thyroid medication, your symptoms will resolve.
Reality: It often takes weeks or even months for thyroid hormone levels to return to normal and symptoms to disappear.
Myth: You can take an over-the-counter iodine supplement to correct hypothyroidism.
Reality: In the United States, where dietary iodine is almost always adequate, iodine deficiency is unlikely to be the cause of hypothyroidism. Therefore, taking supplemental iodine is not likely to correct the problem.
Myth: If thyroid symptoms are mild, you don’t need to take medication.
Reality: Because thyroid hormones are responsible for so many vital body functions, failing to treat even a mild thyroid disorder may lead to a range of other problems, such as osteoporosis or infertility.
Myth: Goiter may be caused by eating “goitrogenic” vegetables, such as broccoli, Brussels sprouts, and spinach.
Reality: Although these foods can interfere with the thyroid’s ability to process iodide, you would have to eat huge amounts of them to cause goiter.
Myth: Thyroid disorders occur only after middle age and only in women.
Reality: Thyroid disorders may occur at any age and in any sex. Hypothyroidism occurs more commonly in older adults, but hyperthyroidism occurs more commonly in younger adults. Although women are more likely to develop thyroid disorders, about 20 percent of cases occur in men.


