Case Study: John Snow and the Origin of Epidemiology
- Page ID
- 26899
This page is a draft and is under active development.
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)John Snow and the Origin of Epidemiology; “You Know Nothing, John Snow.”
Part I—Beginnings

John Snow was born in York, England, in 1813, the first of 9 children of a working-class family. Snow’s wealthy and well-connected uncle, arranged an apprenticeship for his nephew with a surgeon-apothecary, one of the two types of health care providers in 19th century London. Physicians were graduates of the medical programs at Oxford or Cambridge while surgeon-apothecaries went through a longer apprenticeship, attending classes part-time at smaller medical schools. John Snow moved to Newcastle at the age of 14 to apprentice with William Hardcastle. It was in Newcastle, near the end of Snow’s apprenticeship, that he first encountered cholera as it arrived in England in 1831.
In his medical studies, Snow learned the prevailing humoral model of disease, which held that health depended on the balance of four humors: blood, phlegm, black bile, and yellow bile. Diseases resulted from an excess or deficit in one of these four humors. To correct the problem, physicians would use leeches to bleed patients or purgatives to cause diarrhea or vomiting. The humoral model eventually was replaced with the miasma model of disease, which suggested that diseases were caused by pollution or “bad air.” At the time, the Germ Theory of Disease had not been established, and physicians didn’t fully understand the nature of disease and its transmission.
After being released from his apprenticeship, John Snow was one of the first physicians to study and calculate dosages for ether and chloroform as surgical anaesthetics. It was his work with anesthesia and gases that made him doubt the miasma model of disease.
1. Compare the two different types of medical professions of the 19th century. What modern professions would compare to these?
2. *Search cholera and list the major symptoms of the disease. Why is it sometimes called “The Blue Death?”
3. Compare the humoral model of disease (part 1) to the miasma model of disease. Which do you think is closest to our modern understanding of disease?
Part II: Sanitation in the 19th Century
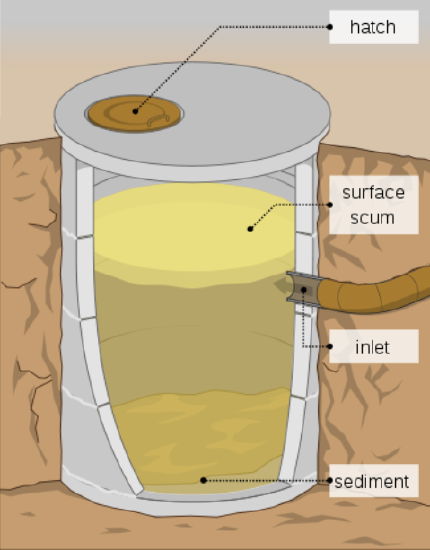
London in the middle of the 19th century contained 2.5 million people, housed in 30 square miles, a population density greater than present-day Manhattan. The Soho district of London had a serious problem with filth due to the large influx of people and a lack of proper sanitary services: the London sewer system had not reached Soho. Many cellars had cesspools underneath their floorboards.
A cesspit (cesspool) was an underground holding tank used for the storage of feces. Some pits were emptied when they became full; cleaned out by tradesmen using shovels and horse-drawn wagons. Some cesspits were designed to allow liquid to leach into the soil. Because of the population density in London, many of these cesspits were overflowing; waste accumulated in basements, courtyards, and even the streets. Since the cesspools were overrunning, the London government decided to dump the waste into the River Thames.
Because of the problems of waste disposal, few Londoners had a source of drinking water uncontaminated by human sewage. At that time, a total of nine different water companies supplied Londoners with water, obtained from either shallow wells or the Thames River. Some companies had their intake pipes farther upstream than others. Water obtained from pipes downstream were more likely to be contaminated with human waste.
4. What was it like to live in London in the early 19th century?
5. Examine the diagram showing a cesspit. Before houses installed cesspits, chamber pots were dumped into the streets. What were some advantages to having a cesspit? What were the disadvantages?
6. How does changing the location of the pipes (either upstream or downstream) improve water quality? Sketch an image of the river and the intake pipes and sewer pipes to show the ideal location.
Part III: Outbreak
 On 31 August 1854, after several other outbreaks had occurred elsewhere in the city, a major outbreak of cholera struck Soho. By September, 500 people had died and the mortality rate was 12.8 percent in some parts of the city. By the end of the outbreak, 616 people had died. John Snow later called it "the most terrible outbreak of cholera which ever occurred in this kingdom."
On 31 August 1854, after several other outbreaks had occurred elsewhere in the city, a major outbreak of cholera struck Soho. By September, 500 people had died and the mortality rate was 12.8 percent in some parts of the city. By the end of the outbreak, 616 people had died. John Snow later called it "the most terrible outbreak of cholera which ever occurred in this kingdom."
The germ theory was not created at this point (as Louis Pasteur would not create it until 1861), so Snow was unaware of the mechanism by which the disease was transmitted, but evidence led him to believe that it was not due to breathing foul air as the miasma model would suggest. He first published his theory in an essay On the Mode of Communication of Cholera in 1849 which proposed that cholera was transmitted in water. The essay received negative reviews in the Lancet and the London Medical Gazette. However, a reviewer made a helpful suggestion in terms of what evidence would be compelling: the crucial natural experiment would be to find people living side by side with lifestyles similar in all respects except for the water source.
Snow sought ways of strengthening his argument by carrying out the crucial experiment sought by the Medical Gazette’s reviewer. He went door to door interviewing families of cholera victims.
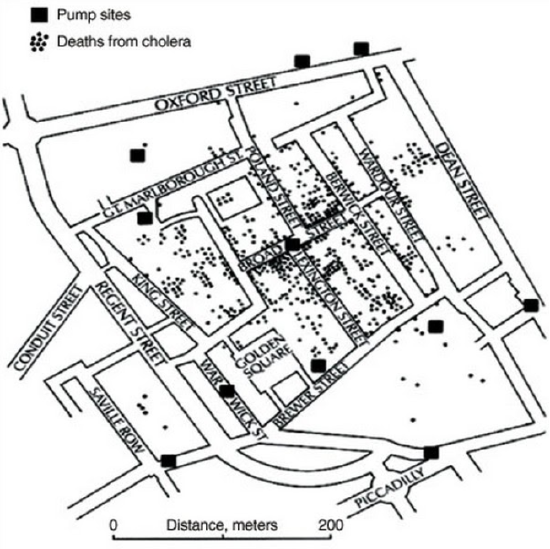
Snow began marking cholera deaths on city maps, and patterns began to emerge. He mapped out the locations of individual water pumps and generated cells which represented all the points on his map which were closest to each pump.
7. Based on the data shown in the map, which pump is the most likely source of the cholera infection? Circle all pumps that might also be suspect in this investigation.
8. The cluster of cases near Saville Row might be considered an outlier as they have their own pump nearby. What questions would Snow want to ask family members in this area?
Part IV: Snow Makes His Case
In Snow's own words:
On proceeding to the spot, I found that nearly all the deaths had taken place within a short distance of the [Broad Street] pump. There were only ten deaths in houses situated decidedly nearer to another street-pump. In five of these cases the families of the deceased persons informed me that they always sent to the pump in Broad Street, as they preferred the water to that of the pumps which were nearer. In three other cases, the deceased were children who went to school near the pump in Broad Street...
The result of the inquiry, then, is, that there has been no particular outbreak or prevalence of cholera in this part of London except among the persons who were in the habit of drinking the water of the above-mentioned pump well.
—John Snow, letter to the editor of the Medical Times and Gazette
Although Snow's chemical and microscopic examination of a sample of the Broad Street pump water was not able to conclusively prove its danger, his studies of the pattern of the disease were convincing enough to persuade the St James parish authorities to disable the well pump by removing its handle. At this point, John Snow had partnered with Reverend Henry Whitehead who assisted with interviewing families and tracking the disease. Whitehead succeeded in identifying an earlier case, an infant living in a house a few feet from the Broad Street pump who died from diarrhea two days before the cholera outbreak was officially recognized.
After excavation of the Broad Street well, it was found that it had been dug only three feet from an old cesspit that had begun to leak fecal bacteria. A mother of the baby who had contracted cholera had its diapers washed into this cesspit and was likely the source of the original infection.
12. What was John Snow’s original hypothesis and how did it conflict with prevailing models of health and disease?
13. Why would evidence of cholera in people living side by side, differing only in water supply, provide critical evidence ?
14. Snow found that none of the monks in the adjacent monastery contracted cholera. They drank only beer, which they brewed themselves. Does this mean that beer made with contaminated water is safe to drink? How could you test this?
Part V: The Aftermath

 Unfortunately, after the cholera epidemic had subsided, government officials replaced the Broad Street Pump Handle. They had responded only to the urgent threat posed to the population, and afterward they rejected Snow's theory. To accept his proposal would have meant indirectly accepting the oral-fecal method transmission of disease, which was too unpleasant for most of the public to contemplate.
Unfortunately, after the cholera epidemic had subsided, government officials replaced the Broad Street Pump Handle. They had responded only to the urgent threat posed to the population, and afterward they rejected Snow's theory. To accept his proposal would have meant indirectly accepting the oral-fecal method transmission of disease, which was too unpleasant for most of the public to contemplate.
Although many continued to reject Snow’s explanation, some began to give it grudging acceptance, often without acknowledging his contribution. Snow’s vindication came at a meeting of the Medical Society where a member stood up after such a presentation insisting that Snow be given credit. The pump is now a historic site in London and is located in front of the John Snow Pub.
15. The basic questions of epidemiology focus on time and place: “why here” and “why now”. What are the answers to these questions for the Broad Street outbreak?
16. Why was the death of the baby a significant observation for this study?
17. Epidemiology relies on non-experimental tests of hypotheses. What was Snow’s hypothesis and how did he test it without performing experiments.
18. Consider the term “non-experimental.” Given you had no ethical concerns with testing on humans, how would you test the hypothesis in an “experimental” way?
Notes
London Map: str.llnl.gov/str/September02/Hall.html
Science Stories: Using Case Studies to Teach Critical Thinking
By Clyde Freeman Herreid, Nancy A. Schiller, Ky F. Herreid books.google.com
"Septic tank EN" by Olek Remesz (wiki-pl: Orem, commons: Orem) - Own work, based on this picture by Zielu20. Licensed under CC BY-SA 3.0 via Wikimedia Commons - http://commons.wikimedia.org/wiki/File:Septic_tank_EN.svg#mediaviewer/File:Septic_tank_EN.svg
http://www.ph.ucla.edu/epi/snow/snowbook.html - “On the Mode of Communcation of Cholera”:

