15.1.2.2.2: Streptococcus pyogenes
- Page ID
- 42659
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)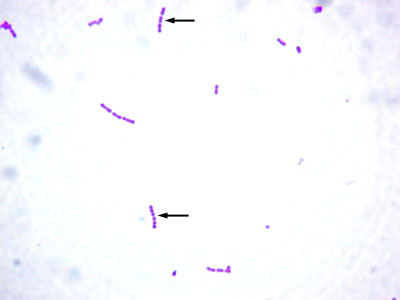
Organism
-
Streptococcus pyogenes, a group A streptococcus, is a Gram-positive coccus typically arranged in chains.
- Facultative anaerobe
- Catalase negative
- Beta-hemolytic

Habitat
- Asymptomatic colonization of the upper respiratory tract in humans.
Source
- Pharyngitis is pread person to person primarily by respiratory droplets; skin infections are spread by direct contact with an infected person or through fomites (contaminated inanimate objects).
Epidemiology
- The group A beta hemolytic streptococci are responsible for most acute human streptococcal infections. Between 5% and 20% of children are asymptomatic carriers. The most common infection is pharyngitis with the organism usually being limited to the mucous membranes and lymphatic tissue of the upper respiratory tract. Children are at greatest risk for infection.
Clinical Disease
- The most common infection is pharyngitis (strep throat) with the organism usually being limited to the mucous membranes and lymphatic tissue of the upper respiratory tract. Characteristic pockets of pus typically form on the tonsils (pyogenes means "pus-making")
- From the pharynx, however, the streptococci sometimes spread to other areas of the respiratory tract resulting in laryngitis, bronchitis, pneumonia, and otitis media.
- Scarlet fever:
- accompanies streptococcal pharyngitis
- diffuse red rash beginning on chest and spreading to the rest of the body; after rash disappears, skin sloughs off
- tongue becomes bright red
- caused by pyrogenic toxins of some strains
- Occasionally, it may enter the lymphatic vessels or the blood and disseminate to other areas of the body, causing septicemia, osteomyelitis, endocarditis, septic arthritis, and meningitis.
- If it enters injured skin, it may cause pyogenic (pus-creating) cutaneous infections such as impetigo (skin infection), erysipelas (localized, pus-filled lesions involving lymph nodes, pain, and inflammation), or cellulitis .
- Necrotizing fasciitis:
- Certain strains of S. pyogenes cause invasive group A beta streptococcal infections. Each year in the U.S. there are between 750 and 1500 cases of necrotizing fasciitis where a streptococcal-coded protease called Exotoxin B destroys the muscle (myositis) or the muscle covering (necrotizing fasciitis).
- S. pyogenes are introduced into compromised skin (cut, scrape, or other wound)
- Commonly called "flesh-eating disease"
- Initial symptoms include redness, swelling, and intense pain at the site of infection
- Later symptoms include distended and discolored skin, fever, nausea, vomiting, low blood pressure, and mental confusion
- Can progress extremely rapidly
- Affected tissue must be removed completely and the patient treated with broad-spectrum antibiotics
-
- Sequelae:
- Subsequent to the initial infection
- Thought to be autoimmune diseases caused by antibodies made against streptococcal antigens cross react with human tissues
- Rheumatic fever
- Antibodies react with joint membranes and heart valves
- Common symptoms are fever, joint pain, heart murmur, fatigue, and small, painless bumps under the skin
- Most common in 5-15 year olds
- Results in life-long heart valve damage
- Acute glomerulonephritis:
- Anitbodies react against glomerular cells and basement membranes of the kidneys
- Symptoms include high blood pressure, low urine output, and blood and proteins in urine
- Children usually completely recover; adults may have permanent damage
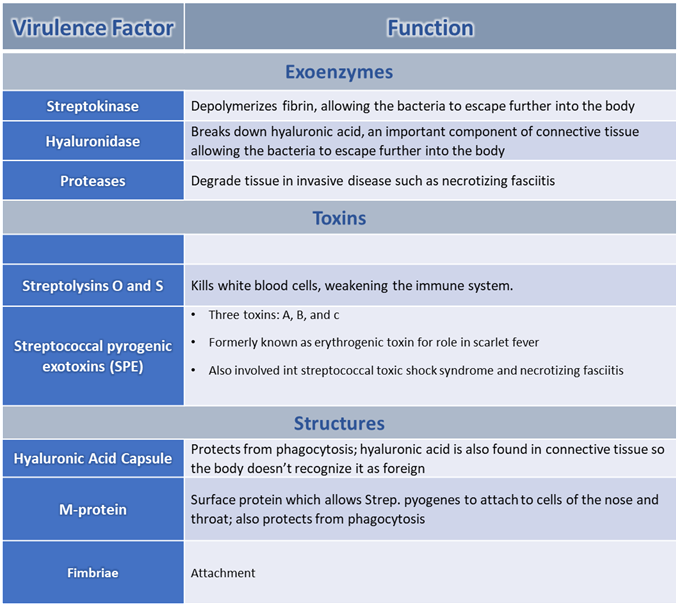
Primary Virulence Factors
- Similar to Staph. aureus, Strep. pyogenes has a variety of virulence factors, some of which (such as the pyrogenic (meaning "fever generating) exotoxins) are only found in certain strains (Figure \(\PageIndex{2}\))
Additional Information: http://textbookofbacteriology.net/streptococcus.html
From Streptococcus Group A Infections, by Sat Sharma, MD, FRCPC, FACP, FCCP, DABSM, Program Director, Associate Professor, Department of Internal Medicine, Divisions of Pulmonary and Critical Care Medicine, University of Manitoba; Site Coordinator of Respiratory Medicine, St Boniface General Hospital; and Godfrey Harding, MD, FRCPC, Program Director of Medical Microbiology, Professor, Department of Medicine, Section of Infectious Diseases and Microbiology, St Boniface Hospital, University of Manitoba, Canada.