21.2C: Animal Viruses
- Page ID
- 13548
Animal viruses have their genetic material copied by a host cell after which they are released into the environment to cause disease.
- Describe various animal viruses and the diseases they cause
Key Points
- Animal viruses may enter a host cell by either receptor -mediated endocytosis or by changing shape and entering the cell through the cell membrane.
- Viruses cause diseases in humans and other animals; they often have to run their course before symptoms disappear.
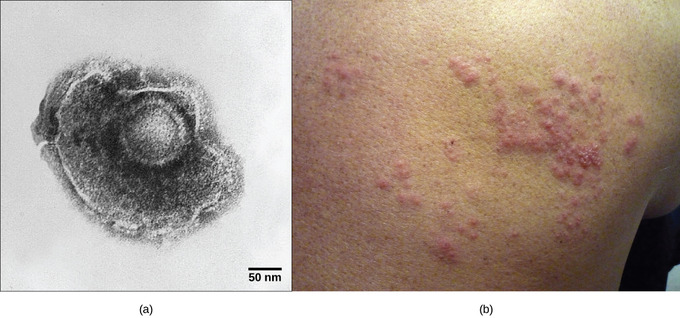
- Examples of viral animal diseases include hepatitis C, chicken pox, and shingles.
Key Terms
- receptor-mediated endocytosis: a process by which cells internalize molecules (endocytosis) by the inward budding of plasma membrane vesicles containing proteins with receptor sites specific to the molecules being internalized
Animal Viruses
Animal viruses, unlike the viruses of plants and bacteria, do not have to penetrate a cell wall to gain access to the host cell. Non-enveloped or “naked” animal viruses may enter cells in two different ways. When a protein in the viral capsid binds to its receptor on the host cell, the virus may be taken inside the cell via a vesicle during the normal cell process of receptor-mediated endocytosis. An alternative method of cell penetration used by non-enveloped viruses is for capsid proteins to undergo shape changes after binding to the receptor, creating channels in the host cell membrane. The viral genome is then “injected” into the host cell through these channels in a manner analogous to that used by many bacteriophages. Enveloped viruses also have two ways of entering cells after binding to their receptors: receptor-mediated endocytosis and fusion. Many enveloped viruses enter the cell by receptor-mediated endocytosis in a fashion similar to some non-enveloped viruses. On the other hand, fusion only occurs with enveloped virions. These viruses, which include HIV among others, use special fusion proteins in their envelopes to cause the envelope to fuse with the plasma membrane of the cell, thus releasing the genome and capsid of the virus into the cell cytoplasm.
After making their proteins and copying their genomes, animal viruses complete the assembly of new virions and exit the cell. Using the example of HIV, enveloped animal viruses may bud from the cell membrane as they assemble themselves, taking a piece of the cell’s plasma membrane in the process. On the other hand, non-enveloped viral progeny, such as rhinoviruses, accumulate in infected cells until there is a signal for lysis or apoptosis, and all virions are released together.
Animal viruses are associated with a variety of human diseases. Some of them follow the classic pattern of acute disease, where symptoms worsen for a short period followed by the elimination of the virus from the body by the immune system with eventual recovery from the infection. Examples of acute viral diseases are the common cold and influenza. Other viruses cause long-term chronic infections, such as the virus causing hepatitis C, whereas others, like herpes simplex virus, cause only intermittent symptoms. Still other viruses, such as human herpes viruses 6 and 7, which in some cases can cause the minor childhood disease roseola, often successfully cause productive infections without causing any symptoms at all in the host; these patients have an asymptomatic infection.
In hepatitis C infections, the virus grows and reproduces in liver cells, causing low levels of liver damage. The damage is so low that infected individuals are often unaware that they are infected, with many infections only detected by routine blood work on patients with risk factors such as intravenous drug use. Since many of the symptoms of viral diseases are caused by immune responses, a lack of symptoms is an indication of a weak immune response to the virus. This allows the virus to escape elimination by the immune system and persist in individuals for years, while continuing to produce low levels of progeny virions in what is known as a chronic viral disease. Chronic infection of the liver by this virus leads to a much greater chance of developing liver cancer, sometimes as much as 30 years after the initial infection.
As mentioned, herpes simplex virus can remain in a state of latency in nervous tissue for months, even years. As the virus “hides” in the tissue and makes few if any viral proteins, there is nothing for the immune response to act against; immunity to the virus slowly declines. Under certain conditions, including various types of physical and psychological stress, the latent herpes simplex virus may be reactivated and undergo a lytic replication cycle in the skin, causing the lesions associated with the disease. Once virions are produced in the skin and viral proteins are synthesized, the immune response is again stimulated and resolves the skin lesions in a few days by destroying viruses in the skin. As a result of this type of replicative cycle, appearances of cold sores and genital herpes outbreaks only occur intermittently, even though the viruses remain in the nervous tissue for life. Latent infections are common with other herpes viruses as well, including the varicella-zoster virus that causes chickenpox. After having a chickenpox infection in childhood, the varicella-zoster virus can remain latent for many years and reactivate in adults to cause the painful condition known as “shingles”.