15.8E: Cholera
- Page ID
- 12301
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)- Describe the mode of transmission for Vibrio cholerae and the steps that can be taken to prevent this
Vibrio Cholerae
Cholera is an infection in the small intestine caused by the bacterium Vibrio cholerae. The primary symptoms of cholera are profuse, painless diarrhea and vomiting of clear fluid. These symptoms usually start suddenly, one to five days after ingestion of the bacteria. The diarrhea is frequently described as “rice water” in nature and may have a fishy odor. If the severe diarrhea is not treated with intravenous rehydration, it can result in life-threatening dehydration and electrolyte imbalances.
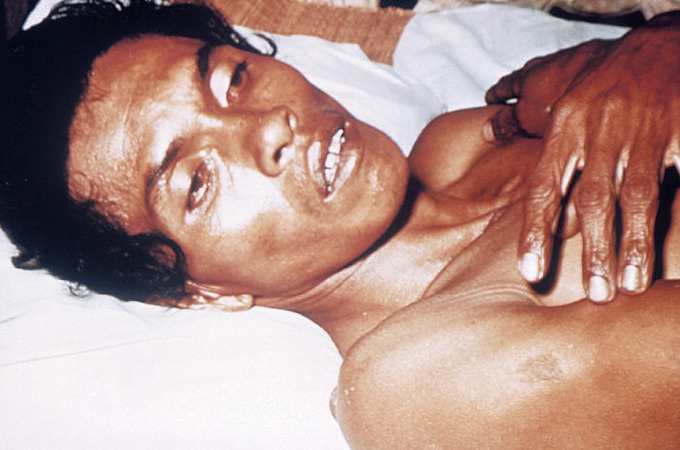
Transmission
Cholera is typically transmitted by either contaminated food or water. In the developed world, seafood is the usual cause, while in the developing world it is more often water. Cholera is rarely spread directly from person to person. Both toxic and nontoxic strains exist.
Most V. cholerae bacteria, when consumed, do not survive the acidic conditions of the human stomach. The few surviving bacteria conserve their energy and stored nutrients during the passage through the stomach by shutting down much protein production. When the surviving bacteria exit the stomach and reach the small intestine, they need to propel themselves through the thick mucus that lines the small intestine to get to the intestinal walls, where they can thrive. V. cholerae bacteria begin production of the hollow cylindrical protein flagellin to make flagella. These flagella are cork-screw helical fibers that rotate to propel the bacteria through the mucus of the small intestine.
Once the cholera bacteria reach the intestinal wall, they no longer need the flagella to move. The bacteria stop producing the protein flagellin, again conserving energy and nutrients by changing the mix of proteins they manufacture in response to the changed chemical surroundings. The V. cholerae start producing the toxic proteins that give the infected person a watery diarrhea.
The diarrhea carries new generations of V. cholerae bacteria out into the drinking water of the next host if proper sanitation measures are not in place. A rapid dip-stick test is available to determine the presence of V. cholerae in a water supply. Samples that test positive should be further tested to determine antibiotic resistance. In epidemic situations, a clinical diagnosis may be made by taking a patient history and doing a brief examination. Treatment is usually started without or before confirmation by laboratory analysis. Although cholera may be life-threatening, prevention of the disease is normally straightforward if proper sanitation practices are followed. In developed countries, due to nearly universal advanced water treatment and sanitation practices, cholera is no longer a major health threat.
Breaking the Transmission Path
Effective sanitation practices, if instituted and adhered to in time, are usually sufficient to stop an epidemic. There are several points along the cholera transmission path at which its spread may be halted.
- Sterilization or proper disposal and treatment of infected fecal waste water produced by cholera victims and all contaminated materials (e.g. clothing, bedding, etc.) is essential. All materials that come in contact with cholera patients should be sanitized by washing in hot water, using chlorine bleach if possible. Hands that touch cholera patients or their clothing, bedding, etc., should be thoroughly cleaned and disinfected with chlorinated water or other effective antimicrobial agents.
- Antibacterial treatment of general sewage by chlorine, ozone, ultraviolet light or other effective treatment before it enters the waterways or underground water supplies helps prevent undiagnosed patients from inadvertently spreading the disease.
- Warnings about possible cholera contamination should be posted around contaminated water sources with directions on how to decontaminate the water (boiling, chlorination etc.) for possible use.
- All water used for drinking, washing, or cooking should be sterilized by either boiling, chlorination, ozone water treatment, ultraviolet light sterilization (e.g. by solar water disinfection), or antimicrobial filtration in any area where cholera may be present.
- Public health education and adherence to appropriate sanitation practices are of primary importance to help prevent and control transmission of cholera and other diseases.
Prevention and Treatment
A number of safe and effective oral vaccines for cholera are available. In most cases, cholera can be successfully treated with oral rehydration therapy (ORT), which is effective, safe, and simple to administer. Rice-based solutions are more efficient than glucose-based ones. In cases of severe dehydration, intravenous rehydration may be necessary. Antibiotic treatments for one to three days shorten the course of the disease and reduce the symptoms. People will recover without them, however, if sufficient hydration is maintained. Doxycycline is typically used first line, although some strains of V. cholerae have shown resistance. Testing for resistance during an outbreak can help determine appropriate future choices. Other antibiotics proven to be effective include cotrimoxazole, erythromycin, tetracycline, chloramphenicol, and furazolidone. Fluoroquinolones, such as norfloxacin, also may be used, but resistance has been reported.
Key Points
- The primary symptoms of cholera are profuse, painless diarrhea and vomiting of clear fluid.
- V. cholerae bacteria that survive the gastric juices produce the hollow cylindrical protein flagellin to make flagella, the cork-screw helical fibers they rotate to propel themselves through the mucus of the small intestine.
- A number of safe and effective oral vaccines for cholera are available.
Key Terms
- flagella: A flagellum is a lash-like appendage that protrudes from the cell body of certain prokaryotic and eukaryotic cells.
- electrolyte: any of the various ions (such as sodium or chloride) that regulate the electric charge on cells and the flow of water across their membranes

