4.4: The Menstrual Cycle
- Page ID
- 187720
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Established in 2014, Menstrual Hygiene Day is observed on May 28th each year. Established by a small non-profit (WASH United), and sponsored by over 1,000 partner organizations from around the world, the mission of WASH's movement is to actively work "in menstrual hygiene education, developing and disseminating low-cost, scalable solutions to improve knowledge and reduce stigma".
May 28 was chosen as Menstrual Hygiene Day for its symbolic significance. May is the fifth month of the year, symbolizing the five days of bleeding during menstruation. The 28th day was chosen because the menstrual cycle averages about 28 days.
Maintaining good menstrual hygiene is difficult in developing countries because of taboos on discussing menstruation and the lack of availability of menstrual hygiene products. Poor menstrual hygiene, in turn, can lead to embarrassment, degradation, and reproductive health problems.
Progress on outreach and education is measurable: In 2014, 22 million people were reached through social media about the importance of menstrual hygiene. By 2025, it was 971 million.


Figure \(\PageIndex{1}\): Representations of global events in 2025. WASH CC-BY 4.0
(Top) Kenya: IRC hosted MHH education sessions for adolescent boys in Kakuma Refugee Camp.
(Bottom) India: The Swachh Bharat Mission in Siddipet coordinated a district-wide activation involving schools, communities, and local institutions.
Women, usually between the ages of 12 and 50, undergo a monthly cycle in which their uterus prepares for pregnancy; it prepares for a fertilized egg to implant and grow into a baby. If pregnancy does not occur, the lining breaks down and is expelled from the uterus. This is known as menstruation.
What Is the Menstrual Cycle?
The menstrual cycle refers to natural changes that occur in a female's reproductive system each month during the reproductive years. The cycle is necessary for egg production and for preparing the uterus for pregnancy. It involves changes in both the ovaries and the uterus and is controlled by pituitary and ovarian hormones.
Day 1 of the cycle is the first day of the menstrual period, when bleeding from the uterus begins as the built-up endometrium lining the uterus is shed. The endometrium builds up again during the remainder of the cycle, only to be shed again during the beginning of the next cycle if pregnancy does not occur. In the ovaries, the menstrual cycle includes the development of a follicle, ovulation of a secondary oocyte, and the degeneration of the follicle if pregnancy does not occur.
Both uterine and ovarian changes during the menstrual cycle are generally divided into three phases, although the phases are not the same in the two organs.
Menarche to Menopause
The reproductive years of females are delineated by the start and stop of the menstrual cycle. The first menstrual period usually occurs around 12 or 13 years of age, an event known as menarche. There is considerable variation among individuals in the age of menarche. It may occasionally occur as early as eight years of age or as late as 16 years of age and still be considered normal. The average age is generally later in the developing world and earlier in the developed world. This variation is thought to be largely attributable to nutritional differences and possibly exposure to endocrine-disrupting substances.
The cessation of menstrual cycles at the end of the reproductive years is termed menopause. The average age of menopause is 52 years, but it may occur normally at any age between about 45 and 55 years of age. The age of menopause varies due to a variety of biological and environmental factors. It may occur earlier due to certain illnesses or medical treatments.
Variation in the Menstrual Cycle
The length of the menstrual cycle — as well as its phases — may vary considerably, not only among different individuals but also from month to month for a given person.
- The average time between the first day of one menstrual period and the first day of the next is 28 days, but it may range from 21 to 45 days.
- Cycles are considered regular when the longest and shortest cycles differ by less than eight days.
- The menstrual period itself is usually about 5 days long, but it may range from 2 to 7 days.
The Production of Eggs in Ovaries
At birth, ovaries contain all the eggs that will ever be produced by an individual, which may include a million or more eggs.
However, the eggs do not begin to mature until puberty begins and sexual maturity is attained. After this stage of an individual's development, one egg typically matures each month and is released from an ovary. This continues until menopause (cessation of monthly periods), typically by age 52. By then, viable eggs may be almost depleted, and hormone levels can no longer support the monthly cycle.
During the reproductive years, either the left or the right ovary will release an egg each month. Which one of the two releases an egg each month seems to be a matter of chance. Occasionally, both ovaries will release an egg at the same time. If both eggs are fertilized, the offspring are fraternal twins (dizygotic, or "two-zygote," twins), and they are no more alike genetically than non-twin siblings.
Oogenesis
The process of producing eggs in the ovaries of a fetus carrying XX chromosomes is called oogenesis.
Eggs are haploid gametes, and their production occurs in several steps that involve different types of cells, as summarized in Figure \(\PageIndex{2}\).
Oogenesis is completed long before birth. It occurs when diploid germ cells called oogonia (plural, oogonia; singular, oogonium) undergo mitosis. Each such cell division produces two diploid cells.
One is called the primary oocyte, and the other is retained to help maintain a reserve of oogonia. The primary oocyte, in turn, begins the first meiotic division (meiosis I). However, it does not complete meiosis I until puberty.
Gametes, or sex cells, are produced by different processes in humans. Egg cells are produced through oogenesis.
Ovarian Cycle
The events of the menstrual cycle that take place in the ovaries make up the ovarian cycle. It consists of changes that occur in the follicles of one of the ovaries. The ovarian cycle is divided into the following three phases: the follicular phase, ovulation, and the luteal phase. These phases are illustrated in Figure \(\PageIndex{2}\).
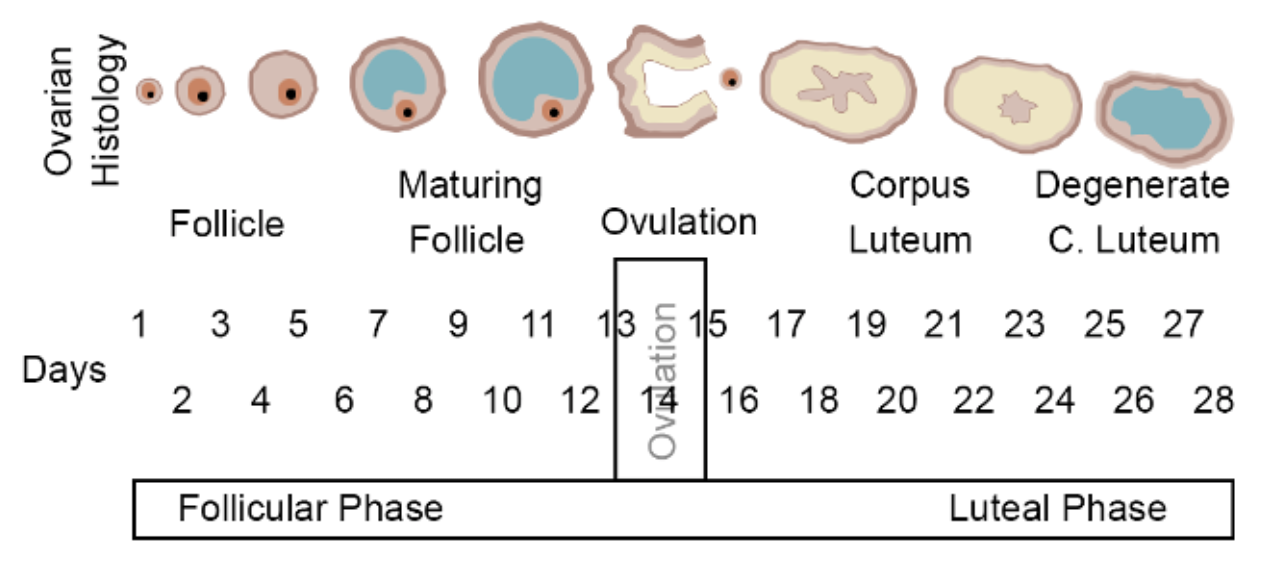
Follicular Phase
Beginning in puberty, about once a month, one of the follicles in an ovary undergoes maturation, and an egg is released. This is known as the follicular phase of the ovarian cycle. It generally lasts about 12 to 14 days for the overall 28-day menstrual cycle.
During this phase, several ovarian follicles are stimulated to begin maturing, but usually only one — the Graafian follicle — matures completely, making it ready to release an egg. The other maturing follicles stop growing and disintegrate. The primary oocyte within the follicle resumes meiosis, as noted in the Oogenesis section above. The secondary oocyte initiates meiosis II, but completes it only if the egg is fertilized.
Follicular development occurs because of a rise in the blood level of follicle-stimulating hormone (FSH), which is secreted by the pituitary gland. The maturing follicle releases estrogen, the level of which rises throughout the follicular phase. You can see these and other changes in hormone levels that occur during the menstrual cycle in the chart in Figure \(\PageIndex{3}\).
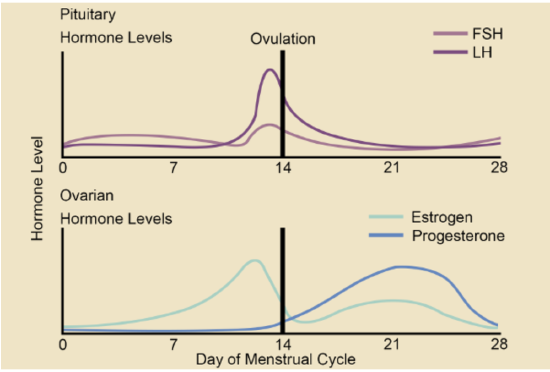
Ovulation
Ovulation is the second phase of the ovarian cycle. It usually occurs around day 14 of a 28-day menstrual cycle. During this phase, the Graafian follicle ruptures and releases its egg. Ovulation is stimulated by a sudden rise in the blood level of luteinizing hormone (LH) from the pituitary gland (Figure \(\PageIndex{3}\) top graph), triggered by a continued rise in estrogen from the maturing follicle in the ovary. The secondary oocyte begins to form, the follicle bursts open, and the ovary ruptures, releasing the secondary oocyte from the ovary.
The now-empty follicle starts to change into a structure called a corpus luteum. The expelled secondary oocyte is usually swept into the nearby Fallopian tube by its waving, fingerlike fimbriae.
Luteal Phase
The luteal phase is the third and final phase of the ovarian cycle. It typically lasts about 14 days in a 28-day menstrual cycle.
At the beginning of the luteal phase, FSH and LH cause the Graafian follicle that ovulated the egg to transform into a structure called a corpus luteum. The corpus luteum secretes progesterone, which in turn suppresses FSH and LH production by the pituitary and stimulates the continued buildup of the endometrium in the uterus.
How this phase ends depends on whether or not the egg has been fertilized.
- If fertilization has occurred,
- a zygote forms and divides to become a blastocyst
- a hormone called human chorionic gonadotropin is produced by the outer layer of the blastocyst
- human chorionic gonadotropin is very similar to LH and preserves the corpus luteum
- the corpus luteum continues to secrete progesterone to maintain the pregnancy
- If fertilization has not occurred,
- the falling levels of FSH and LH during the luteal phase cause the corpus luteum to atrophy
- production of progesterone declines
- the endometrium starts to break down without a high enough level of progesterone to maintain it
- by the end of the luteal phase, the next menstrual cycle begins with the shedding of the endometrium (menses).
While the follicle is maturing in the ovary, the uterus undergoes changes to prepare for an embryo if fertilization occurs. For example, the endometrium gets thicker and becomes more vascular.
Around the time of ovulation, the cervix undergoes changes that help sperm reach the oocyte to fertilize it. The cervical canal widens, and the cervical mucus becomes thinner and more alkaline. These changes help promote the passage of sperm from the vagina into the uterus and make the environment more hospitable to sperm.
Uterine Cycle
The events of the menstrual cycle that take place in the uterus make up the uterine cycle.
This cycle involves changes that mainly occur in the endometrium, the layer of tissue that lines the uterus. The uterine cycle is divided into three phases: menstruation, the proliferative phase, and the secretory phase.
These phases are illustrated in Figure \(\PageIndex{4}\).
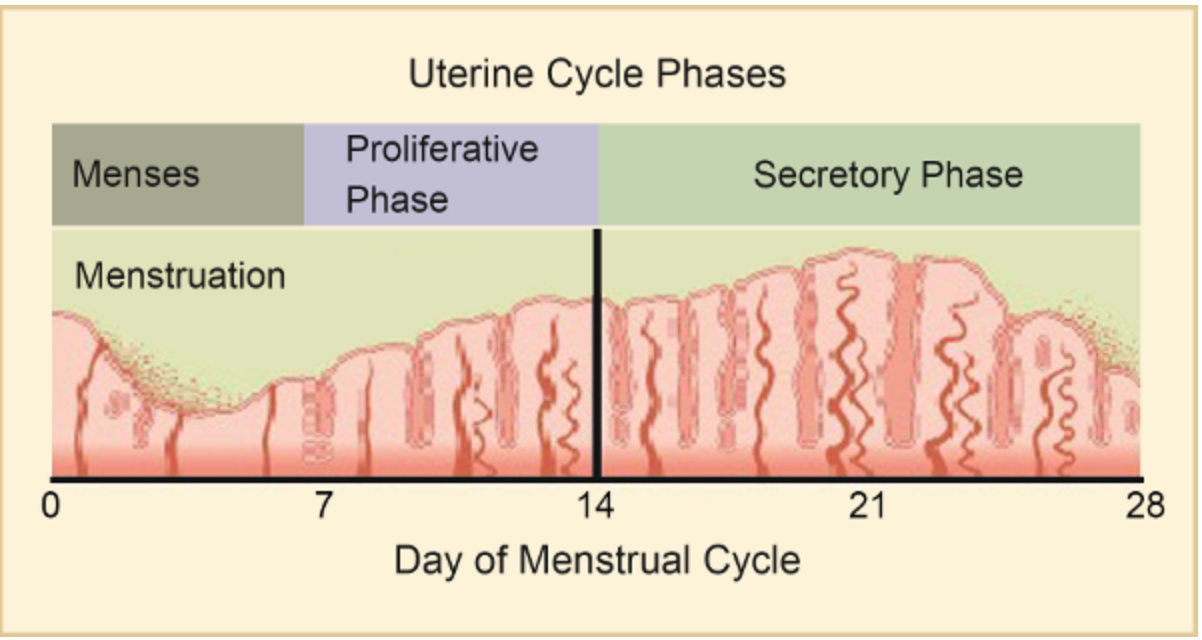
Menstruation
Menstruation (also called the menstrual period or menses) is the first phase of the uterine cycle. It occurs if fertilization has not taken place during the preceding menstrual cycle. During menstruation, the endometrium of the uterus, which has built up during the preceding cycle, degenerates and is shed from the uterus. The average blood loss during menstruation is about 35 mL. The flow of blood is often accompanied by uterine cramps, which may be severe in some people.
Proliferative Phase
The proliferative phase is the second phase of the uterine cycle. During this phase, estrogen secreted by cells of the maturing ovarian follicle causes the lining of the uterus to grow, or proliferate. Estrogen also stimulates the cervix of the uterus to secrete larger amounts of thinner mucus, which can help sperm swim through the cervix and into the uterus, increasing the likelihood of fertilization.
Secretory Phase
The secretory phase is the third and final phase of the uterine cycle. During this phase, progesterone produced by the corpus luteum in the ovary stimulates further changes in the endometrium, making it more receptive to implantation of a blastocyst (more in Section 4.9). For example, progesterone increases blood flow to the uterus and promotes uterine secretions. It also decreases the contractility of smooth muscle tissue in the uterine wall.
Within the field of menstruation studies, our depictions of menstruation and menstruators must be holistic, and the knowledge produced de-stigmatize menstruation.
- First, not all women menstruate. For example, trans women, pregnant women, and those experiencing amenorrhea.
- Second, not all who menstruate are women. For example, those who are AFAB.
- Finally, experiences of menstruating later in life vary among menstruators (e.g., postmenopausal women).
Some do not experience emotional and psychological suffering from their periods in direct relation to their gender identity. Others do, as they disidentify with the body as a whole and/or with certain body parts such as the genitalia or the uterus, or with the bodily function of menstruation. This suffering is sometimes related to gender dysphoria.
Testosterone treatments are a method adopted by some trans menstruators to get rid of unwanted bleeding. Preventing the menstrual period is not necessarily the main reason for using testosterone, but it can be one among several desired outcomes. Menstruators are of a variety of gender identities (far beyond those who identify as trans) and, hence, menstruation cannot be equated singularly with cis/womanhood.
Adapted from Rydström K. (2020). Degendering Menstruation: Making Trans Menstruators Matter. In: Bobel C., Winkler I.T., Fahs B., Hasson K.A., Kissling E.A., Roberts TA. (eds) The Palgrave Handbook of Critical Menstruation Studies. Palgrave Macmillan, Singapore. https://doi.org/10.1007/978-981-15-0614-7_68; CC BY 4.0
Ovarian and Uterine Phases Summarized
Figure \(\PageIndex{5}\): High estrogen and LH stimulate ovulation at the end of the follicular phase of the ovarian cycle. At the same time, endometrial thickness increases during the proliferative phase of the uterine cycle. Following the decline of estrogen and progesterone at the end of the luteal phase from a lack of ovum implantation, the endometrium is shed, and menstruation occurs. Ovarian and Uterine Cycles. Boundless CC-BY-SA 4.0
Fertilization — or Not
Fertilization of an egg by a sperm normally occurs in a Fallopian tube, most often in the part of the tube that passes above the ovary (Figure \(\PageIndex{6}\)).
In order for fertilization to occur, sperm must “swim” from the vagina where they are deposited, through the cervical canal to the uterus, and then through the body of the uterus to one of the Fallopian tubes. Once sperm enter a Fallopian tube, tubular fluid helps carry them toward the secondary oocyte at the distal end of the tube.
The secondary oocyte also promotes fertilization. It releases molecules that guide the sperm and allow the egg's surface to attach to the sperm's surface. The egg can then absorb the sperm, enabling fertilization.
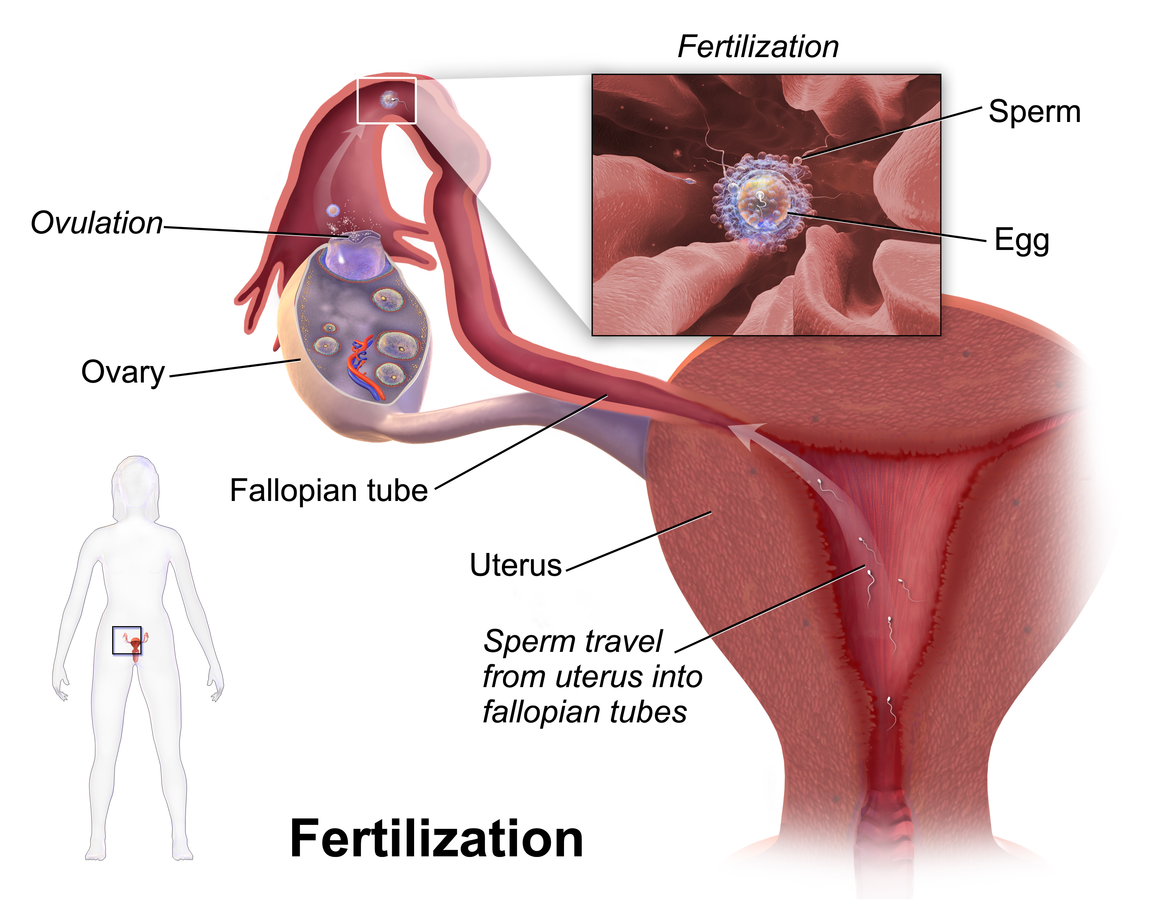
Figure \(\PageIndex{6}\): The Fimbriae of the fallopian tube sweep the egg into the fallopian tube. sperm travels through the cervix and uterus and enters the fallopian tube, where it fertilizes the egg. The embryo, then, travels towards the uterus.
Fertilization. Medical gallery of Blausen Medical CC-BY 3.0.
If Fertilization Occurs
If the secondary oocyte is fertilized by a sperm as it passes through the Fallopian tube, the secondary oocyte quickly completes meiosis II, forming a diploid zygote and another polar body. (This second polar body, like the first, normally breaks down and disappears.)
The zygote then continues the journey through the fallopian tube to the uterus, during which it undergoes several mitotic cell divisions. By the time it reaches the uterus, up to five days after fertilization, it consists of a ball of cells called a blastocyst.
Within another day or two, the blastocyst implants itself in the endometrium lining the uterus, and gestation begins. The processes of pregnancy and childbirth are discussed further in Section 4.9.
If Fertilization Does Not Occur
What happens if the secondary oocyte is not fertilized by a sperm as it passes through the Fallopian tube? It continues toward the uterus without ever completing meiosis II.
It is likely to disintegrate within a few days while still in the Fallopian tube. Any remaining material will be shed from the body during the next menstrual period.


