4.2: Anatomy of the Female Reproductive System
- Page ID
- 187719
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)The geometric design on this ancient stone carving represents a powerful symbol of fertility: the vagina. The symbol is called yoni in Hindu culture and reflects the value it places on the ability to give birth. The vagina is one of several organs in the female reproductive system.

Female Reproductive Organs
The female reproductive system consists of internal and external organs that produce haploid gametes (eggs, or oocytes), secrete sex hormones (such as estrogen), contribute to sexual pleasure, and support and deliver a fetus.
As noted in Section 4.1, the internal reproductive organs include the vagina, uterus, Fallopian (uterine) tubes, and ovaries. The external organs — collectively called the vulva — include the clitoris and labia (Figure \(\PageIndex{2}\)).
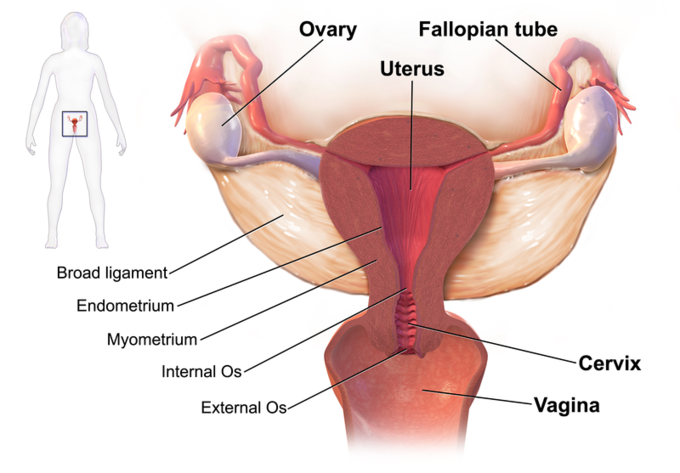
Figure \(\PageIndex{2}\): Structures of the internal female reproductive organs. Boundless CC-BY-SA 4.0
Ovaries
The ovaries are the female gonads, or primary reproductive organs that produce oocytes, or eggs. Ovaries are located on both sides of the pelvic cavity and are supported by many ligaments (Figure \(\PageIndex{2}\)). They are each about the size of an almond and 2-3 cm long.
Ovaries are also endocrine glands and secrete both estrogen and progesterone.
Oogenesis
The developing egg cell (or oocyte) grows within the environment provided by ovarian follicles. Follicles are composed of different types and numbers of cells at different maturation stages, which can be determined by their size. When oocyte maturation is completed, a luteinizing hormone ( LH ) surge secreted by the pituitary gland stimulates follicle rupture and oocyte release.
This process of oocyte development and release is referred to as ovulation. The follicle remains functional and transforms into a corpus luteum, which secretes progesterone to prepare the uterus for possible embryo implantation. Usually, each ovary takes turns releasing eggs each month. However, this alternating egg release is random. When one ovary is absent or dysfunctional, the other ovary will continue to release eggs each month. More is discussed on this topic in the section on the menstrual cycle.
Endocrine Function
Ovaries secrete estrogen, progesterone, and testosterone.
- Estrogen is responsible for the secondary sex characteristics of females at puberty. It is also crucial for the maturation and maintenance of the reproductive organs in their mature functional state.
- Progesterone prepares the uterus for pregnancy and the mammary glands for lactation. The coactions of progesterone and estrogen drive endometrial changes during the menstrual cycle.
- In women, testosterone is essential for the development of muscle mass and bone strength, and for optimal energy levels. It also has a role in libido in women.
Fallopian Tubes
The Fallopian tubes (Figure \(\PageIndex{2}\)) are two thin tubes that lie between the ovaries and the uterus. The Fallopian tubes are not attached to the ovaries, but their broad upper ends — called infundibula — overlap the ovaries. The infundibula also have fringe-like extensions called fimbriae that wave to help guide eggs from the ovaries into the Fallopian tubes.
The lower ends of the Fallopian tubes are attached to the superior body of the uterus on the left and right, opening into the uterus. Eggs are fertilized in the fallopian tubes.
When an ovum is developing in an ovary, it is encapsulated in a sac known as an ovarian follicle. On maturation, the follicle and the ovary’s wall rupture, allowing the ovum to escape. The egg is caught by the fimbriated end of the Fallopian tube and travels into the main tube, where, typically, sperm meet the egg, and fertilization may occur. The fertilized ovum, now a zygote, travels toward the uterus, aided by tubular motions. About 5 days after fertilization, the embryo enters the uterine cavity and may implant about a day later.
Occasionally, an embryo implants into the Fallopian tube instead of the uterus, creating an ectopic pregnancy, which is life-threatening. Ectopic pregnancies are not viable.
Uterus
The uterus (sometimes called the womb) is a pear-shaped, muscular organ that is about 7.6 cm (3 in.) long. It is hormone-responsive and located above the vagina and behind the bladder in the center of the pelvis. The position of the uterus in the pelvis is stabilized by several ligaments and bands of supportive tissue.
The uterus is where a fetus develops during gestation, providing mechanical protection and support for the developing offspring as well as a point of attachment for the placenta. Contraction of the muscular wall of the uterus is responsible for pushing the fetus out of the uterus during vaginal childbirth.
The uterus is also essential in sexual response by directing blood flow to the pelvis and to the external genitalia, including the ovaries, vagina, labia, and clitoris.

Parts of the Uterus
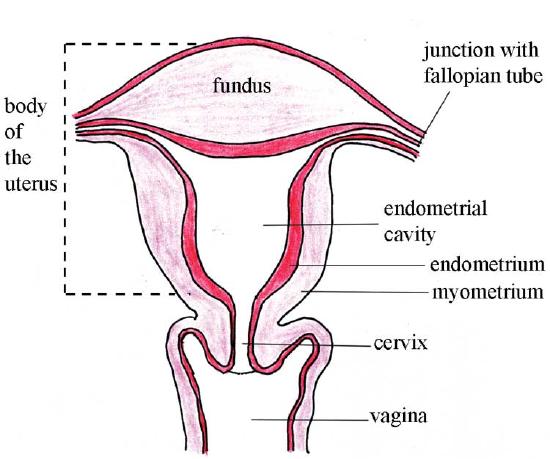
As shown in Figure \(\PageIndex{3}\), the inferior end of the uterus forms the cervix. The cervix is about 2.5 cm (1 in.) long and protrudes downward into the vagina. A small canal runs the length of the cervix, connecting the uterine cavity with the lumen of the vagina. This allows semen deposited in the vagina to enter the uterus, and a baby to pass from the uterus into the vagina during birth. Glands in the cervix secrete mucus that varies in water content and thickness, so it can function either as a barrier to keep microorganisms out of the uterus during pregnancy or as a transport medium to help sperm enter the uterus around the time of ovulation.
The rest of the uterus above the cervix is called the fundus (or body) of the uterus.
The right and left sides of the superior end of the uterus are connected with the two Fallopian tubes.
Tissues of the Uterus
As indicated in Figure \(\PageIndex{4}\), the uterus consists of three tissue layers, called the endometrium, myometrium, and perimetrium.
- The endometrium is the innermost tissue layer of the uterus. It consists of epithelial tissue, including mucous membranes. This layer thickens during each menstrual cycle and, unless an egg is fertilized, sloughs off during the following menstrual period. If an egg is fertilized, the thickened endometrium is maintained by hormones and provides nourishment to the embryo. As gestation progresses, the endometrium develops into the maternal portion of the placenta. The placenta is a temporary organ that consists of a mass of maternal and fetal blood vessels through which the mother’s and fetus’s blood exchange substances.
- The myometrium is the middle layer of the uterus. It consists mainly of a thick layer of smooth muscle tissue. Powerful contractions of the smooth muscle allow the uterus to contract and expel an infant during childbirth.
- The perimetrium is the outermost layer of the uterus. It covers the outer surface of the uterus. This layer consists of two epithelial layers that secrete fluid into the space between them. The fluid allows the uterus to move within the pelvis without rubbing against other organs.
Vagina
The vagina is an elastic, muscular canal leading from its opening in the vulva to the neck of the uterus, called the cervix. It is about 7.5 cm (3.0 in.) long on the anterior surface, and about 9 cm (3.5 in.) long on the posterior surface (Figure \(\PageIndex{5}\)). The vagina accommodates the penis and is the site where sperm are usually ejaculated during sexual intercourse. The vagina also serves to drain blood from the uterus during menstruation and as the birth canal during vaginal childbirth.
The outer walls of the anterior and posterior vagina are formed into longitudinal columns or ridges. The superior portion of the vagina—called the fornix—meets the protruding uterine cervix. The walls of the vagina are lined with an outer, fibrous adventitia, a middle layer of smooth muscle, and an inner mucous membrane with transverse folds called rugae. Together, the middle and inner layers allow the expansion of the vagina to accommodate both intercourse and childbirth. The Bartholin’s glands and the lesser vestibular glands (located near the clitoris) secrete mucus, which keeps the vestibular area moist during intercourse and childbirth.
A thin, perforated hymen can partially surround the opening to the vaginal orifice. Some individuals are born without a hymen. For those who have a hymen, it can be ruptured during physical exercise, a fall, penile-vaginal intercourse, or childbirth.
The vagina is home to a normal population of microorganisms that help to protect against infection by pathogenic bacteria, yeast, or other organisms that can enter the vagina. In a healthy individual, the predominant vaginal bacteria are Lactobacillus. This family of beneficial bacterial flora secretes lactic acid, thereby protecting the vagina by maintaining an acidic pH (below 4.5). Potential pathogens, or organisms that can cause disease, are less likely to survive in these acidic conditions.
The vagina is known as a self-cleaning organ due to the secretion of lactic acid and other fluids that regularly flush the canal. While cleaning the vulva with a gentle soap is safe, douching or other forms of internal vaginal 'cleaning' can disrupt the normal balance of healthy microorganisms and actually increase the risk for infections and irritation.
The American College of Obstetricians and Gynecologists recommends that people not douche and allow the vagina to maintain its normal, healthy population of protective microbial flora.
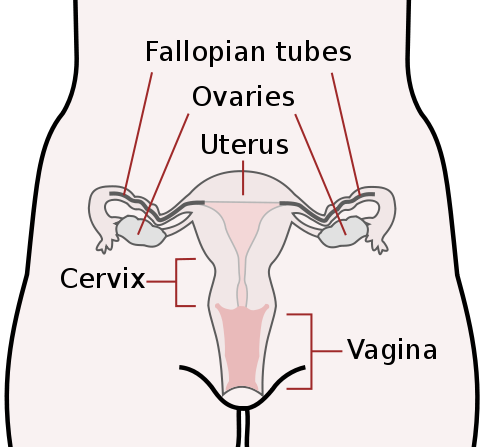
Figure \(\PageIndex{5}\): The vagina is the most immediate internal female reproductive organ. This diagram also indicates the ovaries, uterus, and cervix. Boundless CC-BY-SA 4.0
Sexual Arousal and Intercourse
The concentration of the nerve endings close to the entrance of a woman’s vagina (the lower third) can provide pleasurable sensations during sexual activity when stimulated. Ninety percent of the vagina’s nerve endings are in this area. However, the vagina as a whole has insufficient nerve endings for sexual stimulation and orgasm; this lack of nerve endings makes childbirth significantly less painful.
Research indicates that clitoral tissue extends considerably into the vulva and vagina. During sexual arousal, and particularly clitoral stimulation, the vaginal walls lubricate to reduce friction caused by sexual activity. With arousal, the vagina lengthens rapidly to an average of about 4 in. (10 cm), and can continue to extend in response to pressure. As the woman becomes fully aroused, the vagina tents (expands in length and width), while the cervix retracts. The walls of the vagina are composed of soft elastic folds of mucous membrane, which stretch or contract (with support from pelvic muscles) to the size of the inserted penis or other object, stimulating the penis and helping the male to experience orgasm and ejaculation, thus enabling fertilization.
An erogenous zone commonly referred to as the G-Spot (also known as the Gräfenberg Spot) is located at the anterior wall of the vagina, about five centimeters in from the entrance. Some women experience intense pleasure if the G-Spot is stimulated appropriately during sexual activity. The G-Spot’s existence as a distinct structure separate from the internal clitoral body is still under dispute, and its location can vary from woman to woman and is sometimes nonexistent.
The Vagina and Childbirth
The vagina provides the channel to deliver the baby from the uterus to its independent life outside the mother’s body. During birth, the elasticity of the vagina allows it to stretch many times its normal diameter. The vagina is often referred to as the birth canal in the context of pregnancy and childbirth.
Our bodies are constantly producing, purging, and recycling secretions to fulfill all sorts of functions. Our reproductive organs are no exception. Vaginas undergo ongoing cycles of fluid discharge. But it can be hard to know what is "normal" when there’s a taboo in talking about it. So, what’s healthy discharge? And when is there cause for concern? Elizabeth Micks investigates.
Vulva
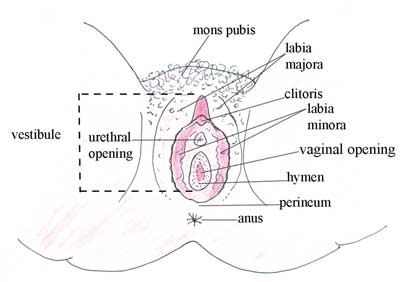
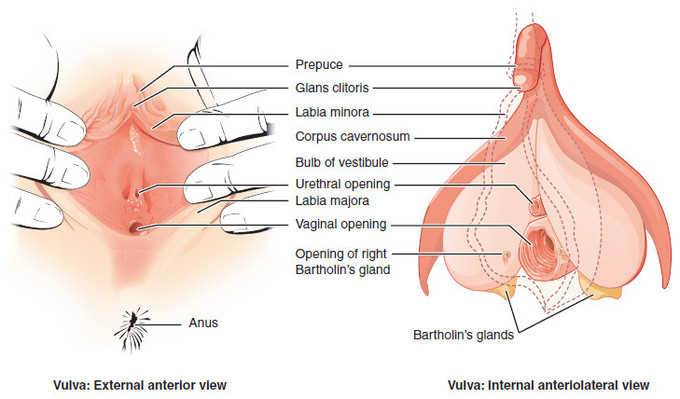
The external reproductive structures are referred to collectively as the vulva (Figure \(\PageIndex{6}\) and Figure \(\PageIndex{7}\)).
Mons pubis
The mons pubis is a pad of fat that is located at the anterior, over the pubic bone. After puberty, it becomes covered in pubic hair, which protects the external and internal reproductive organs and the urinary system by keeping out pathogens, dust, and dirt from the vagina and urethra. Other functions include keeping the vulva warm and moisturized, protecting the skin from friction, and promoting sexual attraction, pheromones, and pleasure.
Labia majora and labia minora
The labia majora (labia = “lips”; majora = “larger”) are folds of hair-covered skin that begin just posterior to the mons pubis. The thinner and more pigmented labia minora (labia = “lips”; minora = “smaller”) extend medially to the labia majora. Although they naturally vary in shape and size, the labia minora, along with pubic hair, serve to protect the urethra and the vagina.
Clitoris
The superior, anterior portions of the labia minora come together to encircle the clitoris (or glans clitoris), an organ that originates from the same cells as the glans penis and has abundant nerves that make it essential in sexual sensation and female orgasm.
The clitoris is located at the front of the vulva where the labia minora meet. The visible portion of the clitoris is the clitoral glans, roughly the size and shape of a pea. The clitoral glans is highly sensitive, containing as many nerve endings as the analogous organ in males, the glans penis. The point where the labia minora attach to the clitoris is called the frenulum clitoridis. A prepuce, the clitoral hood, typically covers and protects the clitoris; however, in women with particularly large clitorises or small prepuces, the clitoris may be partially or wholly exposed. The clitoral hood is the female equivalent of the male foreskin and may be partially hidden inside the pudendal cleft.
Bartholin’s glands
The vaginal opening is located between the opening of the urethra and the anus. It is flanked by outlets to the Bartholin’s glands (or greater vestibular glands), which produce a waxy, pheromone-containing substance involved in lubricating the vaginal opening for intercourse and childbirth.
Hymen
The hymen is a thin membrane that sometimes partially covers the entrance to the vagina. An intact hymen cannot be used as an indication of “virginity”; even at birth, this is only a partial membrane, as menstrual fluid and other secretions must be able to exit the body, regardless of penile-vaginal intercourse.
Perineum
In female anatomy, the perineum is the region between the pubic bone and the anus. The term perineum may refer to only the superficial structures in this region or be used to include both superficial and deep structures. The boundaries vary in classification but may include the genitals and anus.
The perineum is found in both males and females and is an erogenous zone for both. Perineal tears and episiotomy often occur in childbirth with first-time deliveries, but the risk of these injuries can be reduced by preparing the perineum through massage.
Breasts
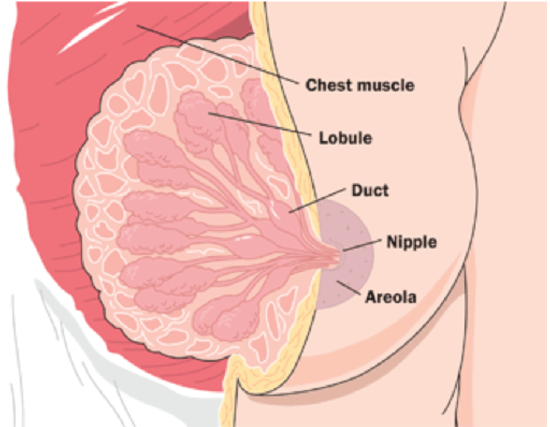
The breasts are not directly involved in reproduction, but because they contain mammary glands, they can provide nourishment to an infant after birth. They also play a role in sexual arousal and attraction.
The breasts overlay major chest muscles, which project outward in a conical shape. The two main types of breast tissue are adipose (fat) tissue and glandular tissue that produces milk. As shown in Figure \(\PageIndex{8}\), each mature breast contains many lobules, where milk is may be produced and stored during pregnancy.
During nursing (or lactation), milk drains into ducts and sacs, which converge at the nipple. Milk exits the breast through the nipple in response to the suckling action of an infant. The nipple is surrounded by a more darkly pigmented area called the areola. The areola contains glands that secrete an oily fluid, which lubricates and protects the nipple during breastfeeding.
Attributions
Some text is adapted from: Anatomy and Physiology (Boundless). Chapter 26.5: The Female Reproductive System. CC-BY-SA 4.0


