19.7: Pancreas
- Page ID
- 92670
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\dsum}{\displaystyle\sum\limits} \)
\( \newcommand{\dint}{\displaystyle\int\limits} \)
\( \newcommand{\dlim}{\displaystyle\lim\limits} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\(\newcommand{\longvect}{\overrightarrow}\)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
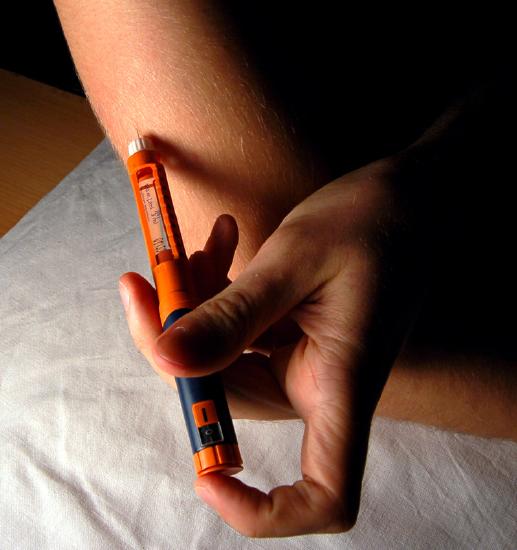
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Giving yourself an injection can be difficult, but for someone with diabetes, it may be a matter of life or death. The person in the photo has diabetes and is injecting himself with insulin, the hormone that helps control the level of glucose in the blood. Insulin is produced by the pancreas.
Introduction to the Pancreas
The pancreas is a large gland located in the upper left abdomen behind the stomach (Figure \(\PageIndex{2}\)), as shown in the figure below. The pancreas is about 15 centimeters (6 in.) long, and it has a flat, oblong shape. Structurally, the pancreas is divided into a head, body, and tail. Functionally, the pancreas serves as both an endocrine gland and an exocrine gland.

- As an endocrine gland, the pancreas is part of the endocrine system. As such, it releases hormones, such as insulin, directly into the bloodstream for transport to cells throughout the body.
- As an exocrine gland, the pancreas is part of the digestive system. As such, it releases digestive enzymes into ducts that carry the enzymes to the gastrointestinal tract, where they assist with digestion. In this concept, the focus is on the pancreas as an endocrine gland.
Beneath your ribs, you’ll find, among other things, the pancreas -- an organ that works a lot like a personal health coach. Emma Bryce explains how this organ controls your sugar levels and produces a special juice that releases the nutrients from your food to help keep you in the best possible shape.
The Pancreas as an Endocrine Gland
The endocrine tissues of the pancreas are organized into clusters of cells called pancreatic islets (Figure \(\PageIndex{3}\)). They are also called the islets of Langerhans.
There are approximately 3 million pancreatic islets, and they are crisscrossed by a dense network of capillaries. The capillaries are lined by layers of islet cells that have direct contact with the blood vessels, into which they secrete their endocrine hormones.
The pancreatic islets consist of four main cell types, each secreting a distinct endocrine hormone. However, all the hormones produced by pancreatic islets play crucial roles in glucose metabolism and blood glucose regulation, among other functions.
- Islet cells called alpha (α) cells secrete the hormone glucagon. The function of glucagon is to increase blood glucose levels. It does this by stimulating the liver to convert stored glycogen into glucose, which is released into the bloodstream.
- Islet cells called beta (β) cells secrete the hormone insulin. The function of insulin is to lower blood glucose levels. It does this by promoting the absorption of glucose from the blood into fat, liver, and skeletal muscle cells. In these tissues, the absorbed glucose is converted into glycogen, fats (triglycerides), or both.
- Islet cells called delta (δ) cells secrete the hormone somatostatin. This hormone is also called the growth hormone-inhibiting hormone because it inhibits the anterior lobe of the pituitary gland from producing growth hormone. Somatostatin also inhibits the secretion of pancreatic endocrine hormones and pancreatic exocrine enzymes.
- Islet cells called gamma (γ) cells secrete the hormone pancreatic polypeptide. The function of pancreatic polypeptide is to help regulate the secretion of both endocrine and exocrine substances by the pancreas.

Disorders of the Pancreas
There are various disorders that affect the pancreas. They include pancreatitis, pancreatic cancer, and diabetes mellitus.
Pancreatitis
Pancreatitis is inflammation of the pancreas. It has a variety of possible causes, including gallstones, chronic alcohol use, infections such as measles or mumps, genetic causes, and certain medications.
Pancreatitis occurs when digestive enzymes produced by the pancreas damage the gland’s tissues, which causes problems with fat digestion.
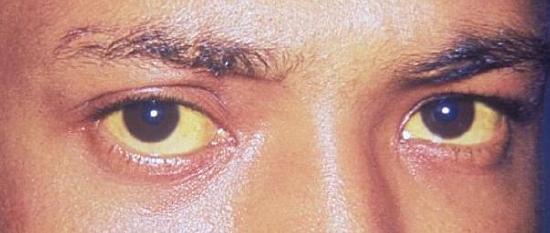
The disorder is usually associated with intense central abdominal pain, which may radiate to the back. Yellowing of the skin and whites of the eyes (Figure \(\PageIndex{4}\)), which is called jaundice, is a common sign of pancreatitis. People with pancreatitis may also have pale stools and dark urine.
Treatment of pancreatitis includes administering drugs to manage pain and addressing the underlying cause of the disease, for example, by removing gallstones.
Pancreatic Cancer
There are several different types of pancreatic cancer that may affect either the endocrine or the exocrine tissues of the gland.
Cancers affecting the endocrine tissues are all relatively rare. However, their incidence has been rising sharply. It is unclear to what extent this reflects increased detection, especially through medical imaging techniques. Unfortunately, pancreatic cancer is usually diagnosed at a relatively late stage, when it is too late for surgery, the only way to cure the disorder.
Pancreatic cancer is rare before the age of 40 and occurs most often after the age of 60. In the United States, pancreatic cancer is the fourth most common cause of death due to cancer.
Factors that increase the risk of developing pancreatic cancer include smoking, chronic pancreatitis, and diabetes. About one in four cases of pancreatic cancer are attributable to smoking. Certain rare genetic conditions are also risk factors for pancreatic cancer.
Diabetes Mellitus
The most common type of pancreatic disorder is diabetes mellitus, more commonly called simply 'diabetes'.
There are many different types of diabetes, but diabetes mellitus is the most common.
It occurs in two major types, type 1 diabetes and type 2 diabetes.
The two types have different causes and may also have different treatments, but they generally produce the same initial symptoms, which include excessive urination and thirst, among others (Figure \(\PageIndex{5}\)).
These symptoms occur because the kidneys excrete more urine to rid the blood of excess glucose, and the loss of water in the urine stimulates greater thirst.
When diabetes is not well controlled, it is likely to have several serious long-term consequences. Most of these consequences are due to damage to small blood vessels caused by high glucose levels.
- Damage to blood vessels, in turn, may lead to an increased risk of coronary artery disease and stroke.
- Damage to retinal blood vessels can lead to gradual vision loss and blindness.
- Damage to blood vessels in the kidneys can lead to chronic kidney disease, sometimes requiring dialysis or a kidney transplant.
- Long-term consequences of diabetes may also include damage to the nerves of the body, known as diabetic neuropathy. In fact, this is the most common complication of diabetes. Symptoms of diabetic neuropathy may include numbness, tingling, and pain in the extremities.
Type 1 Diabetes
Type 1 diabetes is a chronic autoimmune disorder in which the immune system attacks the insulin-secreting beta cells of the pancreas. As a result, people with type 1 diabetes lack the insulin needed to keep blood glucose levels within the normal range.
Type 1 diabetes may develop in people of any age, but is most often diagnosed before adulthood. For type 1 diabetics, insulin injections are critical for survival.
Type 2 Diabetes
Type 2 diabetes is the most common form of diabetes. The cause of high blood glucose in this form of diabetes usually includes a combination of insulin resistance and impaired insulin secretion.
Both genetic and environmental factors play roles in the development of type 2 diabetes.
Management of type 2 diabetes includes changes in diet and physical activity, which may increase insulin sensitivity and help reduce blood glucose levels to normal ranges. Medications may also be used as part of the treatment, as may insulin injections.
Some patients with type 1 diabetes have been given pancreatic islet cell transplants from other human donors. If the transplanted cells are not rejected by the recipient’s immune system, they can cure the patient of diabetes. However, only about 1,000 such surgeries have been performed over the past 10 years due to a shortage of suitable human donors.
In June of 2016, a research team led by Dr. David K.C. Cooper at the Thomas E. Starzl Transplantation Institute in Pittsburgh, Pennsylvania, reported on their work developing pig islet cells for transplantation into patients with human diabetes. The researchers genetically engineered the pig islet cells to be protected from the human immune response. As a result, patients receiving transplanted cells would require only minimal immune suppression after surgery. Pig islet cells would also be less likely to transmit pathogenic agents, as animals could be raised in a controlled environment.
The researchers have successfully transplanted the pig islet cells into monkey models of type 1 diabetes. As of June 2016, the scientists were seeking funding to conduct clinical trials in humans with type 1 diabetes.
Dr. Cooper predicted that if the human trials go as well as expected, the pig islet cells could be available to cure patients in as little as 2 years.
Diabetes has a history dating back to Ancient Greece. Our treatment of it, however, is more recent and was originally made possible by man's best friend. Due to physiological traits shared with humans, dogs have saved countless lives through the discovery of insulin. Duncan C. Ferguson shares the story of the canine's great contribution to man -- and how we can all reap the medical benefits.


