19.3: Lower Respiratory Tract
- Page ID
- 53809
Lower Respiratory Tract
Once air makes its way into the larynx it then continues down the trachea (commonly known as the windpipe) which ultimately splits into two main stems towards the right and left lungs, respectively: the right primary bronchus and the left primary bronchus. The right primary bronchus is wider than the left primary bronchus and it is also has a more vertical angle than the left primary bronchus. Due to these structural differences, if a foreign object is accidently inhaled, it is more likely to become lodged in the right primary bronchus than the left primary bronchus.
The large airways are lined mostly by pseudostratified ciliated columnar epithelium with mucus-secreting goblet cells, respiratory mucosa. Mucus helps trap particles and then the ciliated columnar cells beat rhythmically to move the mucus and any trapped particles from the air towards the pharynx where they can either be spit out or swallowed. This mechanism is known as the mucociliary escalator.
Above: (Left) The larynx, trachea, large bronchi, and lungs (only part shown). (Top right) Cross section of the trachea, located anterior to the esophagus. (Bottom right) The respiratory mucosa lining the inside of most of the large airways and creates the mucociliary escalator.
Above: Pseudostratified ciliated columnar epithelia that line the inside of large airways and are responsible for creating the mucociliary escalator.
Above: (Left) The trachea, magnified by 10x. The trachea, continuing inferiorly from the larynx, lies anterior to the esophagus. The patency of the trachea and primary bronchi respiratory organs is maintained by C-shaped cartilage rings, whose openings face the esophagus. The two main lobes of the thyroid gland are located at the lateral boundaries of the trachea. (Right) The walls of the trachea and primary bronchi are identical, resembling the pattern typical for most respiratory passageways. Longitudinally oriented elastic fibers are numerous in the lamina propria, sometimes forming an obvious elastic lamina. Bundles of interlacing smooth muscle lie external to the elastic fibers. The trachea and primary bronchi are extrapulmonary and are part of the conducting portion of the respiratory system. Magnified by 100x.
The bronchi are the largest airways of the lungs and they branch again and again becoming smaller and smaller. At each branch point, they get a different name. The primary bronchi branch into secondary bronchi which branch into tertiary bronchi. The first three generations of bronchi are all pretty wide and have cartilage rings for support. After the first three generations of bronchi though the airwaves get more narrow called bronchioles meaning "little bronchi" and these can stay open without the need for cartilage air is conducted through smaller and smaller bronchioles for about 15 to 20 generations and collectively these are known as conducting bronchioles. These conducting bronchioles are also lined by ciliated columnar cells. Mucus-secreting goblet cells are present as well as a new type of cell called a club cell. These club cells secrete glycosaminoglycans which protect a bronchial or epithelium, that can also transform into ciliated columnar cells so they help regenerate and replace damaged cells, if needed.
|
Lower Respiratory Tract Structure |
Location |
Function |
|---|---|---|
|
alveolar duct |
thin-walled passages at the end of respiratory bronchioles leading to alveolar sacs containing alveoli |
conducting air to/from the alveolar sacs and alveoli |
|
alveolar macrophages |
mobile cells in the alveoli |
big eater cells that patrol alveoli for debris and engulf it to remove it (dust, bacteria, etc.) |
|
alveolar sac |
a structure resembling a bunch of grapes off of an alveolar duct; contains alveoli |
conducting air to/from alveoli; assemblage of alveoli that allow gas transfer with the pulmonary capillaries wrapped around the outside of alveoli |
|
alveoli |
spherical thin-tissue structures assembled into bunches (alveolar sacs) |
assemblage of alveoli that allow gas transfer with the pulmonary capillaries wrapped around the outside of alveoli |
|
bronchial tree |
successive branches of airways wrapped in cartilage; primary bronchi (first branches), secondary bronchi (second branches), and tertiary bronchi |
conducting air to/from bronchioles |
|
bronchioles |
airway branches off of tertiary bronchi in the lungs; smaller passages than bronchi; have a layer of smooth muscle; have cilia; lead to terminal bronchioles which lead to respiratory bronchioles; divide into 2-10 alveolar ducts |
conducting air to/from alveolar ducts |
|
lungs |
paired organs within pleural cavities |
conduct air and enable gas exchange to occur between the air in the lungs and blood in the pulmonary capillaries |
|
parietal pleura |
serous membranes forming the outer layers of the pleural cavities |
forms outer aspects of the pleura cavities; produces pleura fluid to lubricate the pleural cavities |
|
trachea |
tube between the larynx and the primary bronchi; wrapped in tracheal cartilage to keep airways open |
conducting air to/from the lungs |
|
type I alveolar cell |
form about 95% of alveoli surfaces; simple squamous epithelial cells |
gas exchange with capillaries |
|
type II alveolar cell |
very small cuboidal cells in the alveoli |
produce and secrete pulmonary surfactant to maximize gas exchange |
|
visceral pleura |
serous membranes on the external surface of the lung |
forms inner aspects of the pleura cavities; produces pleura fluid to lubricate the pleural cavities |
Above: Secondary bronchi, bronchioles, and alveoli in the lungs. Pulmonary blood vessels are also present. Tissue is magnified by 40x.
Above: A respiratory bronchiole is formed from a terminal bronchiole by the addition of alveoli and by a decrease in its diameter and in the thickness of its wall. The accumulation of additional alveoli to a respiratory bronchiole reduces the wall area of this bronchiole and forms an alveolar duct. Tissue is magnified by 100x.
Now all these cells of the bronchioles receive oxygenated blood from the bronchial arteries of the systemic circulation. The last conducting bronchioles are the terminal bronchioles and then after that air moves into the respiratory bronchioles. Eventually the respiratory bronchioles end at alveolar ducts leading to alveolar sacs containing bunches of alveoli.
Above: (Left) Alveoli arranged in alveolar sacs at the end of alveolar ducts. (Right) Diagram showing how gas exchange occurs between an alveolus and the passing blood in a capillary.
There are hundreds of millions of alveoli in the lungs. The alveoli are where gas exchange occurs between the lungs and the blood. There are no cilia or smooth muscle and instead the walls lined by thin epithelial cells called alveolar cells. Most of the alveolar surface is covered by type I alveolar cells where gas exchange occurs. The type I alveolar cells form a respiratory membrane where O2 (necessary to make ATP) passes from the lungs into the blood and CO2 (a waste product from ATP production) passes from the blood and into the lungs for exhalation. Other alveolar cells called type II alveolar cells have the ability to secrete a substance called surfactant helps decrease the surface tension within the alveoli and therefore helps gases to pass across the respiratory membrane more efficiently. Finally if foreign particles make it deep into the lungs there are alveolar macrophages that can "eat" (phagocytize) the particles up to remove them.
On the other side of the type I alveolar cells are endothelial cells that line the pulmonary capillary walls. Carbon dioxide diffuses out from the deoxygenated blood in the pulmonary capillaries and into the air of the alveoli which will be breathed out upon exhalation. With each breath in, oxygen enters the alveoli and freely diffuses into the blood in the pulmonary capillaries. This blood is now oxygenated and will return to the heart to complete the pulmonary circuit of blood circulation. This newly oxygenated blood is then pumped through the systemic circuit to provide oxygen to the body tissues. This oxygen is used in a metabolic process called cellular respiration, a process conducted by cells throughout the body to produce the energy-rich molecule ATP. It is because of ATP, and the process of making it (cellular respiration), that oxygen is vital for human life.
Above: (Left) Diagram of the structure of the alveolar-pulmonary capillary junction. (Right) Most of the same structures present in the diagram to the left are shown in the microscopic image of alveoli.
Above: (Left) Left lung from an (top) anterior view and (bottom) medial view. (Right) Right lung from an (top) anterior view and (bottom) medial view.
Above: Cadaver images of (left) the bronchial tree and (right) the branches of pulmonary arteries and pulmonary veins within the lungs.
The right lung has three lobes, the superior lobe, middle lobe and inferior lobe, separated by two fissures, a horizontal fissure and an oblique fissure. The left lung just has two lobes the superior lobe and the inferior lobe, separated by an oblique fissure.
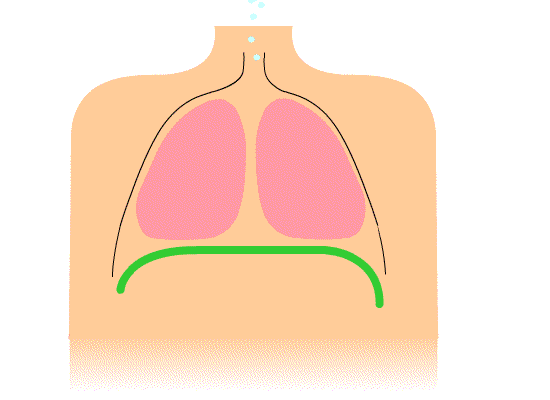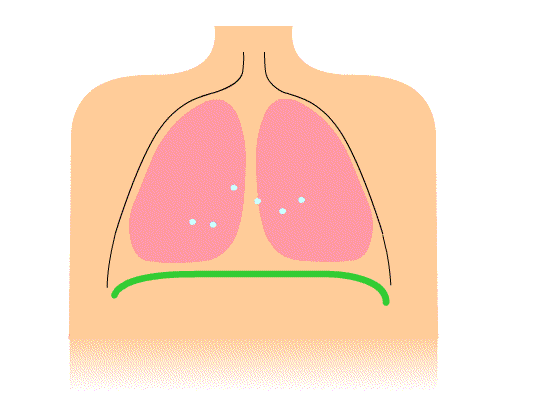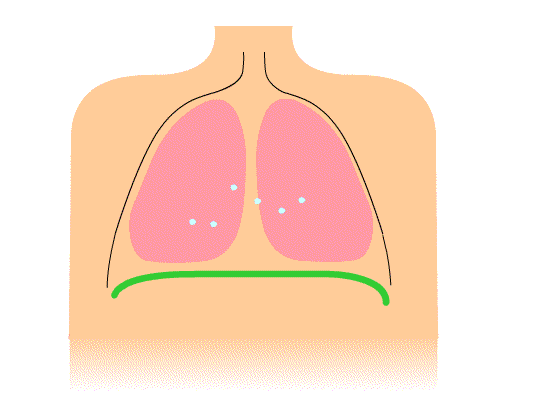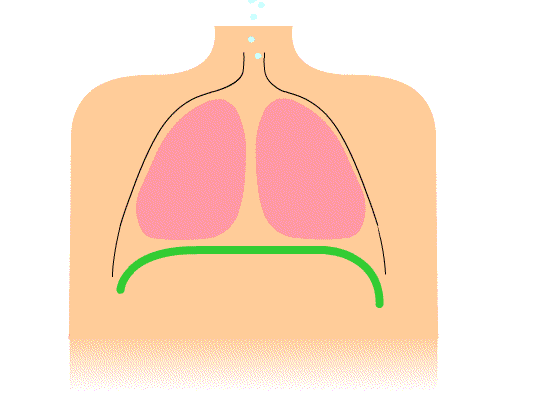
Above: Animation of diaphragm contraction and relaxation resulting in inhalation and exhalation, respectively.
During inhalation, the diaphragm contracts to pull downward while the thorax muscles contract to pull open the chest which both help reduce the pressure inside of the lungs causing gases from the higher pressure air outside of the body to rush into the lungs (gases move from high pressure to low pressure). During an exhalation, the muscles of the diaphragm and thorax relax allowing the lungs to spring back to their normal size which increases internal pressure in the lungs such that the pressure becomes higher inside the lungs than outside the body. The result is that air moves out of the lungs (gases move from high pressure to low pressure).
Above: The lungs are located in the pleural cavities surrounded by parietal pleura and visceral pleura (serosa).
Clinical Application: Pneumonia
Pneumonia is an infection of the lungs that can be acquired by breathing in bacteria or viruses. The infection causes the alveoli to fill with fluid/pus, which can make breathing difficult or labor-some because the body may not be able to get the oxygen it needs from the alveoli walls as easily. Other typical symptoms of pneumonia can include fever, coughing up sputum, chills, nausea, vomiting, and diarrhea, among others. Sometimes symptoms can be mild, causing people to refer to their illness as “walking pneumonia”. Because types of pneumonia are caused by bacteria, antibiotics are commonly used to treat many forms of pneumonia within a reasonable time period. However, viral pneumonias will not improve with the use of antibiotics since antibiotics only kill bacteria. Pneumonia should be taken seriously; it can be severe and deadly for infants, the elderly, and others with an already compromised immune system.
Attributions
- "1.1 Anatomy and Physiology of Respiratory System" by Paul Hudson is licensed under CC BY-NC 4.0
- "Anatomy 204L: Laboratory Manual (Second Edition)" by Ethan Snow, University of North Dakota is licensed under CC BY-NC 4.0
- "Anatomy and Physiology Lab Reference" by Laird C Sheldahl, OpenOregonEducational Resources, Mt. Hood Community College is licensed under CC BY-SA 4.0
- "Anatomy of the Respiratory System" by Dongho Kim is licensed under CC BY-NC-SA 4.0
- "Bronchial anatomy.jpg" by Patrick J. Lynch, medical illustrator is licensed under CC BY 2.5
- Diaphragmatic breathing.gif by John Pierce is in the Public Domain
- "Digital Histology" by Department of Anatomy and Neurobiology and the Office of Faculty Affairs, Virginia Commonwealth University School of Medicine and the ALT Lab at Virginia Commonwealth University is licensed under CC BY 4.0
- "Gas exchange in the aveolus simple (en).svg" by domdomegg is licensed under CC BY 4.0
- "Medical gallery of Blausen Medical 2014" by Blausen.com staff is licensed under CC BY 3.0


