5.2.2: Yeasts
- Page ID
- 28924
- Briefly describe yeasts and state how they reproduce asexually.
- Briefly describe pseodohypae, hyphae, blastoconidia (blastospores), and chlamydoconidia (chlamydospores) and name a yeast producing these structures.
- Name three potentially pathogenic yeasts and state an infection each causes.
Yeast Morphology
- Yeast (see Figure 1) are unicellular fungi which usually appear as oval cells 1-5 µm wide by 5-30 µm long.
- They have typical eukaryotic structures (see Figure 2 and Figure 3).
- They have a thick polysaccharide cell wall.
- They are facultative anaerobes.
- The yeast Candida is said to be dimorphicin that it can grow as an oval, budding yeast, but under certain culture conditions, the budding yeast may elongate and remain attached producing filament-like structures called pseudohyphae. C. albicans may also produce true hyphae similar to molds (see Figure 4). In this case long, branching filaments lacking complete septa form. The pseudohyphae and hyphae help the yeast to invade deeper tissues after it colonizes the epithelium. Asexual spores called blastoconidia (blastospores) develop in clusters along the hyphae, often at the points of branching. Under certain growth conditions, thick-walled survival spores called chlamydoconidia (chlamydospores) may also form at the tips or as a part of the hyphae (see Figure 5.)
| For More Information: A Comparison of Prokaryotic and Eukaryotic Cells from Unit 1 |
The Role of Fungal Cell Wall Components in Initiating Body Defense
To protect against infection, one of the things the body must initially do is detect the presence of microorganisms. The body does this by recognizing molecules unique to microorganisms that are not associated with human cells. These unique molecules are called pathogen-associated molecular patterns or PAMPs. (Because all microbes, not just pathogenic microbes, possess PAMPs, pathogen-associated molecular patterns are sometimes referred to as microbe-associated molecular patterns or MAMPs.)
Components of the yeast cell wall that function as PAMPs include lipoteichoic acids, and zymosan. In addition, bacteria and other microorganisms also possess mannose-rich glycans (short carbohydrate chains with the sugar mannose or fructose as the terminal sugar) that function as PAMPs. These mannose-rich glycans are common in microbial glycoproteins and glycolipids but rare in those of humans. These PAMPs bind to pattern-recognition receptors on a variety of defense cells of the body and triggers innate immune defenses such as inflammation, fever, and phagocytosis.
| Flash animation showing the release of fungal mannans from the cell walls of yeast and their subsequent binding to pattern-recognition receptors on a macrophage. |
| For More Information: Review of Pathogen-Associated Molecular Patterns (PAMPs) from Unit 5 |
| For More Information: Review of Pattern-Recognition Receptors from Unit 5 |
| For More Information: Review of Inflammation from Unit 5 |
Yeast cell wall components also activate the alternative complement pathway and the lectin pathway, defense pathways that play a variety of roles in body defense. Cell wall molecules can also trigger adaptive immunity such as the production of antibody molecules against bacterial cell wall antigens. An antigen is defined as a substance that reacts with antibody molecules and antigen receptors on lymphocytes. An immunogen is an antigen that is recognized by the body as non-self and stimulates an adaptive immune response.
The body recognizes an antigen as foreign when epitopes of that antigen bind to B-lymphocytes and T-lymphocytes by means of epitope-specific receptor molecules having a shape complementary to that of the epitope. The epitope receptor on the surface of a B-lymphocyte is called a B-cell receptor and is actually an antibody molecule. The receptor on a T-lymphocyte is called a T-cell receptor (TCR).
Reproduction of yeasts
1. Yeasts reproduce asexually by a process called budding (see Figure 1 and Figure 6). A bud is formed on the outer surface of the parent cell as the nucleus divides. One nucleus migrates into the elongating bud. Cell wall material forms between the bud and the parent cell and the bud breaks away.
- Scanning electron micrograph of Saccharomyces; courtesy of Dennis Kunkel's Microscopy.
- Movie of Saccharomyces cerevisiae reproducing by budding. Movie of Growth and Division of Budding Yeast (Saccharomyces cerevisiae) . © Phillip Meaden, author. Licensed for use, ASM MicrobeLibrary.
2. A few yeasts, such as Candida albicans, also produce clusters of asexual reproductive spores called blastoconidia (blastospores) and thick-walled survival spores called chlamydoconidia (chlamydospores) ; see Figure 5.
3. Yeasts can also reproduce sexually by means of sexual spores called ascospores which result from the fusion of the nuclei from two cells followed by meiosis. Sexual reproduction is much less common than asexual reproduction but does allow for genetic recombination.
Yeast Infections
Candida albicans
Candida albicans is found as normal flora on the mucous membranes and in the gastrointestinal tract, but is usually held in check by normal flora bacteria and normal body defenses.
Candida can cause a variety of opportunistic infections in people who are debilitated, immunosuppressed, or have received prolonged antibacterial therapy. Women who are diabetic, pregnant, taking oral contraceptives, or having menopause are also more prone to vaginitis. These conditions alter the sugar concentration and pH of the vagina making it more favorable for the growth of Candida. People who are immunosuppressed frequently develop thrush, vaginitis, and sometimes disseminated infections.
Any Candida infection is called candidiasis. Candida most commonly causes vaginitis , thrush (an infection of the mouth), balantitis (an infection of the foreskin and head of the penis), onychomycosis (an infection of the nails), and dermatitis (diaper rash and other infections of moist skin). Less commonly, Candida can infect the lungs, blood, heart, and meninges, especially in the compromised or immunosuppressed host. Candida now causes about 10% of all cases of septicemia. Candidiasis of the esophagus, trachea, bronchi, or lungs, in conjunction with a positive HIV antibody test, is one of the indicator diseases for AIDS.
Candida is said to be dimorphic, that is it has two different growth forms. It can grow as an oval, budding yeast, but under certain culture conditions, the budding yeast may elongate and remain attached producing filament-like structures called pseudohyphae. C. albicans may also produce true hyphae similar to molds. In this case long, branching filaments lacking complete septa form. The pseudohyphae and hyphae help the yeast to invade deeper tissues after it colonizes the epithelium. Asexual spores called blastoconidia are reproductive units produced by budding in yeasts. Under certain growth conditions, thick-walled survival spores called chlamydoconidia may also form at the tips or as a part of the hyphae (see Figure 5)
The most common Candida species causing human infections is C. albicans, causing 50-60% of all Candida infections. Candida glabrata is second, causing 15-20% of Candida infections; Candida parapsilosis is third, responsible for 10-20%.
Cryptococcus neoformans
A lesser known but often more serious pathogenic yeast is Cryptococcusneoformans. Like many fungi, this yeast can also reproduce sexually and the name given to the sexual form of the yeast is Filobasidiella neoformans. It appears as an oval yeast 5-6 µm in diameter, forms buds with a thin neck, and is surrounded by a thick capsule (Figure 8.2.6). It does not produce pseudohyphae and chlamydospores. The capsule enables the yeast to resist phagocytic engulfment. The yeast is dimorphic. In its sexual form, as well as in its asexual form under certain conditions, it can produce a hyphal form.
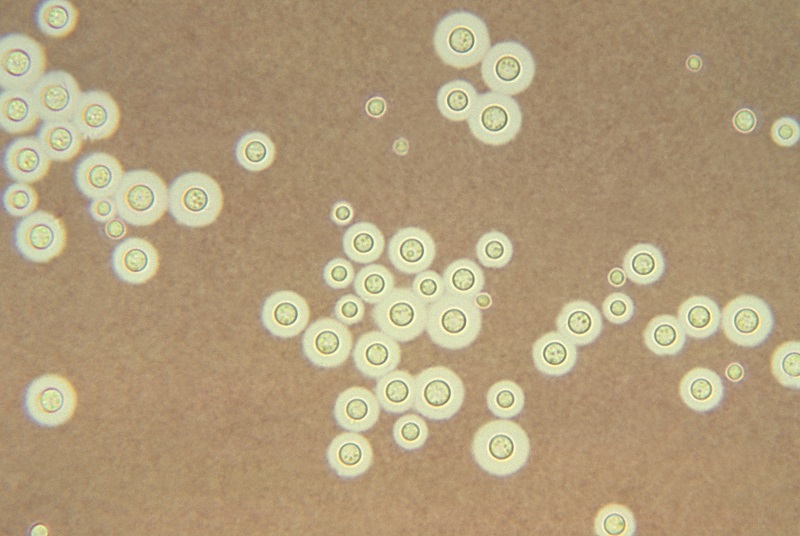
Figure 8.2.6: India ink stain of encapsulated Cryptococcus neoformans. Note encapsulated yeast.Image provided by Dr. Leanor Haley. Courtesy of the Centers for Disease Control and Prevention.
Cryptococcus infections are usually mild or subclinical but, when symptomatic, usually begin in the lungs after inhalation of the yeast in dried bird feces. It is typically associated with with pigeon and chicken droppings and soil contaminated with these droppings. Cryptococcus, found in soil, actively grows in the bird feces but does not grow in the bird itself. Usually the infection does not proceed beyond this pulmonary stage. In the immunosuppressed host, however, it may spread through the blood to the meninges and other body areas, often causing cryptococcal meningoencephalitis. Any disease by this yeast is usually called cryptococcosis.
Dissemination of the pulmonary infection can result in a very severe and often fatal cryptococcal meningoencephalitis. Cutaneous and visceral infections are also found. Although exposure to the organism is probably common, large outbreaks are rare, indicating that an immunosuppressed host is usually required for the development of severe disease. Extrapulmonary cryptococcosis, in conjunction with a positive HIV antibody test, is another indicator disease for AIDS.
Pneumocystis jiroveci
Pneumocystis jiroveci (formerly called Pneumocystis carinii) (see Figure 7 and Figure 8) is thought to be transmitted from person to person by the respiratory route and is almost always asymptomatic. However, in persons with highly depressed immune responses, such as people with leukemias or infected with the Human Immunodeficiency Virus (HIV), P. jiroveci can cause a severe pneumonia called PCP (Pneumocystis pneumonia).
P. jiroveci can be found in three distinct morphologic stages:
- The trophozoite (trophic form), a haploid amoeboid form 1-4 µm in diameter that replicates by mitosis and binary fission. The trophic forms are irregular shaped and often appears in clusters.
- A precystic form or early cyst. Haploid trophic forms conjugate and produce a zygote or sporocyte (early cyst).
- The cyst form, which contains several intracystic bodies or spores are 5-8 µm in diameter. It has been postulated that in formation of the cyst form (late phase cyst), the zygote undergoes meiosis and subsequent mitosis to typically produce eight haploid ascospores (sporozoites) See Figure 7. As the haploid ascospores are released the cysts often collapse forming crescent-shaped bodies (see Figure 8). P. jiroveci is usually transmitted by inhalation of the cyst form. Released ascospores then develop into replicating trophic forms that attach to the wall of the alveoli and replicate to fill the alveoli.
In biopsies from lung tissue or in tracheobronchial aspirates, both a trophic form about 1-4 µm in diameter with a distinct nucleus and a cyst form between 5-8 µm in diameter with 6-8 intracystic bodies (ascospores) can be seen.
Malassezia globosa
Malassezia globosa is a dimorphic yeast that is the most frequent cause of a superficial skin infection called tinea versicolor that commonly appears as a hypopigmentation of the infected skin. M. globosa is also the most common cause of dandruff and seborrheic dermatitis. The yeast is naturally found on the skin. To view additional photomicrographs of Candida, Cryptococcus, and Pneumocystis, see the AIDS Pathology Tutorial at the University of Utah.
- A woman has taken broad spectrum antibiotics for two weeks to treat a bacterial infection. She subsequently develops vaginitis.
- Explain what might account for this.
- Why didn’t the antibiotics prevent the vaginitis?
- A young child with an immunosuppressive disorder and living in an urban area routinely played in a park with a large pigeon population. The child subsequently developed a respiratory infection followed by symptoms of meningitis.
- What infection might be expected and why?
- What might the lab look for in the spinal fluid to help confirm this?
Summary
- Yeasts are eukaryotic unicellular fungi
- Some yeast are dimorphic in that they can grow as an oval, budding yeast, but under certain culture conditions, they may produce filament-like structures called hyphae similar to molds.
- Components of the yeast cell wall that function as pathogen-associated molecular patterns or PAMPs include lipoteichoic acids, zymosan, and mannose-rich glycans.
- These PAMPs bind to pattern-recognition receptors or PRRs on a variety of body defense cells and triggers innate immune defenses.
- Cell wall molecules can also trigger adaptive immunity such as the production of antibody molecules against bacterial cell wall antigens.
- Yeasts reproduce asexually by a process called budding.
- Candida albicans is found as normal flora on the mucous membranes and in the gastrointestinal tract but is usually held in check by the body’s normal microbiota and normal body defenses.
- Candida can cause a variety of opportunistic infections in people who are debilitated, immunosuppressed, or have received prolonged antibacterial therapy, and infect the lungs, blood, heart, and meninges, especially in the compromised or immunosuppressed host.
- Cryptococcus neoformans infections are usually mild or subclinical but, when symptomatic, usually begin in the lungs after inhalation of the yeast in dried bird feces.
- Pneumocystis jiroveci can cause a severe pneumonia called PCP (Pneumocystis pneumonia).
- Malassezia globosa is the most frequent cause of a superficial skin infection called tinea versicolor and also the most common cause of dandruff.
Contributors
Dr. Gary Kaiser (COMMUNITY COLLEGE OF BALTIMORE COUNTY, CATONSVILLE CAMPUS)


