15.1.4: Mycoplasma pneumoniae
- Page ID
- 42668
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \) \( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)\(\newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\) \( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\) \( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\) \( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\) \( \newcommand{\Span}{\mathrm{span}}\) \(\newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\) \( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\) \( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\) \( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\) \( \newcommand{\Span}{\mathrm{span}}\)\(\newcommand{\AA}{\unicode[.8,0]{x212B}}\)

Organism
- Mycoplasma pneumoniae is one of the smallest, free-living organisms (1 to 2 μm long and 0.1 to 0.2 μm wide)
- cells cannot be seen with light microscopy
- M. pneumoniae cells are pleomorphic (taking on many shapes), but often described as spindle-shaped
- one end of the cell contains the "attachment organelle" where adhesins specific for respiratory tract epithelial cells are concentrated (Figure \(\PageIndex{1}\))
- Although they lack a cell wall, mycoplasmas are evolutionarily most closely related to the Gram-positives and are in the Firmicutes phylum
- require an osmotically stable environment (such as within host organism) to prevent lysis
- In addition to small cell size, also have extremely small genome size (0.8 Mbp and 687 genes as opposed to the more typical 4-6 Mbp and 4000-5000 genes of bacteria)
- Can be grown in culture, but colonies are so small a microscope is needed to see them clearly
- Known to ferment glucose, but little else is know about metabolism
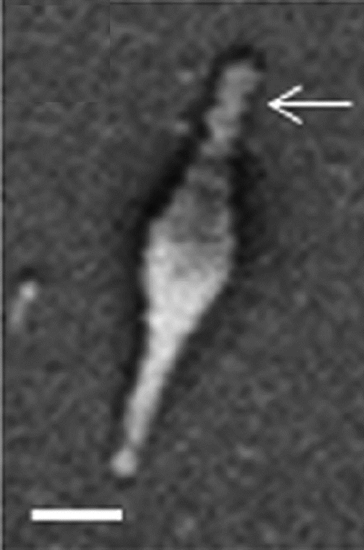
Figure \(\PageIndex{1}\): Scanning electron micrograph of M. pneumoniae cell. Terminal attachment structures indicated by arrowheads. Bar = 200 nm (10.1128/JB.01865-14)
Habitat
- Exclusively found in human respiratory tract
Source
- Inhaled in aersols from infected individual
Epidemiology
- Transmission/outbreaks more common within groups often in close proximity (military bases, households, hospitals, and other congregate living situations)
- Incubation period of 1-3 weeks
- M. pneumoniae causes up to 40% or more of cases of community-acquired pneumonias and as many as 18% of cases requiring hospitalization in children (https://cmr.asm.org/content/17/4/697)
- estimated 18,700 to 108,000 cases of pneumonia in hospitalized adults annually in US
- Risk of hospitalization increases greatly after age 50
- Mortality rate very low (~0.1%), but severe and fatal complications can occur
Clinical Disease
- M. pneumoniae infection is ordinarily mild, and as many as half of adult cases may be asymptomatic
- Most common disease is pneumonia
- Disease referred to by a couple different names
- "walking pneumonia" because usually treated on outpatient basis
- "primary atypical pneumonia" because of its unresponsiveness to antibiotics typically used to treat pneumonia
- Symptoms: persistent dry cough, sore throat, hoarseness, fever, chills, body aches, earache, and general malaise
- Can rarely cause fulminant (sudden with rapid progression) disease involving multiple body systems and organ failure or other extrapulminary infections such as septimcemia and encephalitis
- Usually easily treated with tetracyclines, macrolides (both target ribosomes), or fluoroquinolones (target DNA replication)
- antibiotics which target the bacterial cell wall are ineffective
Primary Virulence Factors
- Adhesins specific for ciliated cells of the respiratory epithelium contained within the attachment organelle allow tight association between M. pneumoniae and epithelial cells (Figure \(\PageIndex{2}\))
- cilia movement is impaired and mucus removal from the respiratory tract is decreased
- M. pneumoniae does not produce toxins, but prolonged colonization kills the epithelial cells

Figure \(\PageIndex{2}\): Transmission electron micrograph of M. pneumoniae-infected hamster tracheal ring, demonstrating the close association of the attachment structure to the epithelium (arrow). (Copyright J. L. Jordan and D. C. Krause.)
Additional Information:

