13.1: Normal Flora of the Human Body
- Page ID
- 51151
The importance of the normal bacterial flora (a.k.a. microbiota) of the human body has been an area of increasing interest in both research and the popular media. One frequently cited statistic is that there are 10-100 times more bacterial than human cells in the body. More recent calculations, however, result in a ratio closer to 1:1, with an estimated 1013 human cells and 1013 – 1015 bacterial cells. The cellular contribution of microbes to the human body, however, is small compared to the genetic contribution. The human genome contains approximately 20,000 genes, but there are 3.3 million unique bacterial genes in the gut microbiota alone. That is a 150-fold difference between the human and bacterial genetic contribution. No matter the exact proportion of bacteria in the human body, the impact of the microbiota on our physiology is substantial.
It has been known for decades that animals raised without normal flora display a variety of health effects across many body systems. Not surprisingly, neither the digestive system nor the immune system develops properly. The cecum tends to be enlarged and other GI abnormalities appear. The immune system is underdeveloped. More recently it has been shown that the central nervous system, including the brain, does not develop properly in these animals. Because bacteria produce vitamins necessary for animal nutrition (most notably vitamin K), animals without normal flora suffer from vitamin deficiencies. Lack of normal flora also makes animals more susceptible to infection with a variety of pathogens, particularly those that infect the GI tract. Although lack of normal flora generally has negative effects, it does also result in an absence of dental caries and lower body fat.
Normal flora is found in all areas of the human body exposed to the environment (one exception is the lungs), but internal organs and body fluids are considered sterile in a healthy individual. This is generally true, although bacteria are sometimes found in these “sterile” tissues even in healthy people. For instance, a person’s blood will become bacteremic (contain bacteria) for up to three hours after brushing their teeth.
Each area of the human body contains a characteristic population of microbes (Figure \(\PageIndex{1}\)), although the exact composition of each person’s flora is unique. The diversity of the bacteria populating the human gut alone is enormous, with an estimated 40,000 species. An increasing number of studies associates such shifts in the gut microbiota with outcomes such as susceptibility to infection, immune disorders, metabolic changes, and altered mood and behavior. Each of these physiological effects can be linked directly to chemical communication within the microbiota and between the microbiota and human.
Flora of the Skin
The exact microbial population on the skin depends on the specific body area. Moist areas, such as axilla (armpits) and groin, tend to have more (and different) bacterial growth compared to drier areas. The most common bacteria of the skin flora are the Gram-positive, catalase positive cocci of the genera Staphylococcus and Micrococcus. Although S. aureus can occasionally be found on the skin, it is more commonly found in the nose in those people that carry it in their normal flora.
Flora of the Mouth and Upper Respiratory Tract
The flora of the mouth and upper respiratory tract is typically associated with a more diverse set of microbes. Streptococci, specifically, alpha-hemolytic Streptococci often referred to collectively as the “viridans Streptococci”are very prominent in the mouth. These include S. mutans, S. sanguis, and S. mitis. S. mutans in particular plays a critical role in the formation of plaque and dental caries (cavities). Although both Staphylococci and Streptococci are Gram-positive cocci, unlike the Staphylococci the Streptococci are catalase-negative, consistent with the low-oxygen environment of the mouth.
Other inhabitants of the mouth and upper respiratory tract include bacteria in the genera Neisseria and Haemophilus. As mentioned above, Staph. aureus is most often found in the nose of those individuals who carry it in their normal flora. The fungal genus Candida is also common in the mouth and upper respiratory tract.
Flora of the Intestines
The most studied population of normal flora in the microbes living in the intestines, often referred to as the gut microbiota. Although the bacterium most commonly associated with the intestines is E. coli, it is actually not the most numerous in the intestine. Bacteria in the phylum Bacteroidetes form a large proportion of bacteria in the gut. The Gram-positive Firmicutes (such as Lactobacillus and Clostridium) and Actinobacteria (including Bifidobacterium) can be equally numerous. In healthy individuals, proteobacteria (including E. coli and other Enterobacteriaceae) are the least abundant of the major bacterial groups in the intestines. There are many other groups of microbes found in the intestines, including fungi such as Candida. It is shifts in the proportions of these groups of microbes that are typically studied when investigating the role of normal flora on human health.

Acquiring Normal Flora
The first introduction of microbiota to a human occurs at birth (a fetus in utero should be microbe-free). Typically, this introduction of flora is from the mother’s vaginal flora. Infants born by caesarean section have significantly different microbiota than those born vaginally. In contrast to the “normal” composition of the gut microbial community, the microbiota of infants born by caesarean section tend to have a high proportion of bacteria normally found on the skin. Although the effects are minor, this difference in the composition of their microbial community have been linked to a variety of health effects including development of the GI tract and immune system.
An infant’s diet also has a substantial effect on the establishment of a healthy microbiota. Human breast milk contains specific oligosaccharides that cannot be digested by the infant but are readily utilized by beneficial gut bacteria such as Bifidobacterium.
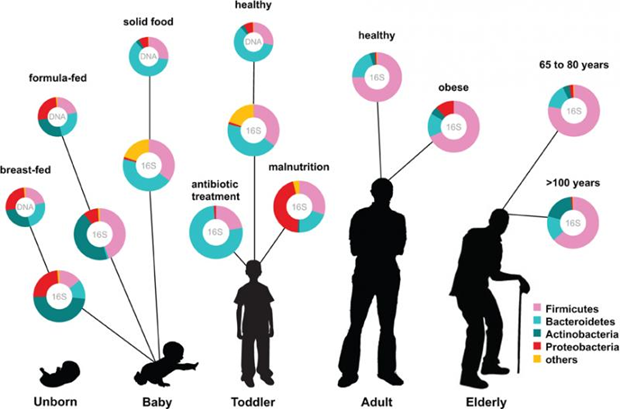
Throughout early childhood a person’s microbiota develops as they encounter new microbes, change their diet, and are exposed to a variety of environmental factors. The immune system plays an important role in promoting the establishment of beneficial bacteria and removing those that could be harmful. There is some evidence that children who are not exposed to a variety of microbes early in life or frequently take antibiotics display the effects of an altered microbiome later on such as allergies, metabolic disorders and obesity, and possibly even certain mental disorders. A person’s microbiota is fully established by about 3 years of age. It remains relatively stable through adulthood but begins to decline at about 65 years old (Figure \(\PageIndex{2}\)). Throughout a person’s lifetime a variety of factors can influence the composition of their microbiota including diet, environmental factors, and genetics.