15.11: Age Related Dysfunctions of the Endocrine System
- Page ID
- 40658
Diabetes Mellitus
An important example of negative feedback is the control of blood sugar.
- After a meal, the small intestine absorbs glucose from digested food. Blood glucose levels rise.
- Increased blood glucose levels stimulate beta cells in the pancreas to produce insulin.
- Insulin triggers liver, muscle, and fat tissue cells to absorb glucose, where it is stored. As glucose is absorbed, blood glucose levels fall.
- Once glucose levels drop below a threshold, there is no longer a sufficient stimulus for insulin release, and the beta cells stop releasing insulin.
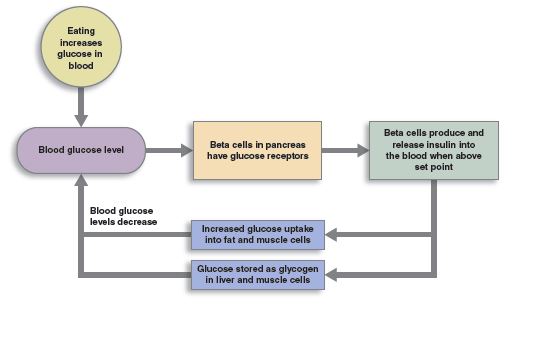
Due to synchronization of insulin release among the beta cells, basal insulin concentration oscillates in the blood following a meal. The oscillations are clinically important, since they are believed to help maintain sensitivity of insulin receptors in target cells. This loss of sensitivity is the basis for insulin resistance. Thus, failure of the negative feedback mechanism can result in high blood glucose levels, which have a variety of negative health effects.
Let’s take a closer look at diabetes. In particular, we will discuss diabetes type 1 and type 2. Diabetes can be caused by too little insulin, resistance to insulin, or both.
Type 1 Diabetes occurs when the pancreatic beta cells are destroyed by an immune-mediated process. Because the pancreatic beta cells sense plasma glucose levels and respond by releasing insulin, individuals with type 1 diabetes have a complete lack of insulin. In this disease, daily injections of insulin are needed.
Also affected are those who lose their pancreas. Once the pancreas has been removed (because of cancer, for example), diabetes type 1 is always present.
Type 2 Diabetes is far more common than type 1. It makes up most of diabetes cases. It usually occurs in adulthood, but young people are increasingly being diagnosed with this disease. In type 2 diabetes, the pancreas still makes insulin, but the tissues do not respond effectively to normal levels of insulin, a condition termed insulin resistance. Over many years the pancreas will decrease the levels of insulin it secretes, but that is not the main problem when the disease initiates. Many people with type 2 diabetes do not know they have it, although it is a serious condition. Type 2 diabetes is becoming more common due to increasing obesity and failure to exercise, both of which contribute to insulin resistance.
Hypothyroidism
Inflammation of the thyroid gland is the more common cause of low blood levels of thyroid hormones. Called hypothyroidism, the condition is characterized by a low metabolic rate, weight gain, cold extremities, constipation, reduced libido, menstrual irregularities, and reduced mental activity. In contrast, hyperthyroidism—an abnormally elevated blood level of thyroid hormones—is often caused by a pituitary or thyroid tumor. In Graves’ disease, the hyperthyroid state results from an autoimmune reaction in which antibodies overstimulate the follicle cells of the thyroid gland. Hyperthyroidism can lead to an increased metabolic rate, excessive body heat and sweating, diarrhea, weight loss, tremors, and increased heart rate. The person’s eyes may bulge (called exophthalmos) as antibodies produce inflammation in the soft tissues of the orbits. The person may also develop a goiter.
Stress Responses
Stress responses are not unique to older persons. People of all ages must respond to stress. However, the physiological changes that contribute to aging can be quite stressful, and how people respond to stress can change with age.
What goes on inside our bodies when we experience stress? The physiological mechanisms of stress are extremely complex, but they generally involve the work of two systems—the sympathetic nervous system and the hypothalamic-pituitary-adrenal (HPA) axis. When a person first perceives something as stressful (Selye’s alarm reaction), the sympathetic nervous system triggers arousal via the release of adrenaline from the adrenal glands. Release of these hormones activates the fight-or-flight responses to stress, such as accelerated heart rate and respiration. At the same time, the HPA axis, which is primarily endocrine in nature, becomes especially active, although it works much more slowly than the sympathetic nervous system. In response to stress, the hypothalamus (one of the limbic structures in the brain) releases corticotrophin-releasing factor, a hormone that causes the pituitary gland to release adrenocorticotropic hormone (ACTH). The ACTH then activates the adrenal glands to secrete a number of hormones into the bloodstream; an important one is cortisol, which can affect virtually every organ within the body. Cortisol is commonly known as a stress hormone and helps provide that boost of energy when we first encounter a stressor, preparing us to run away or fight. However, sustained elevated levels of cortisol weaken the immune system.
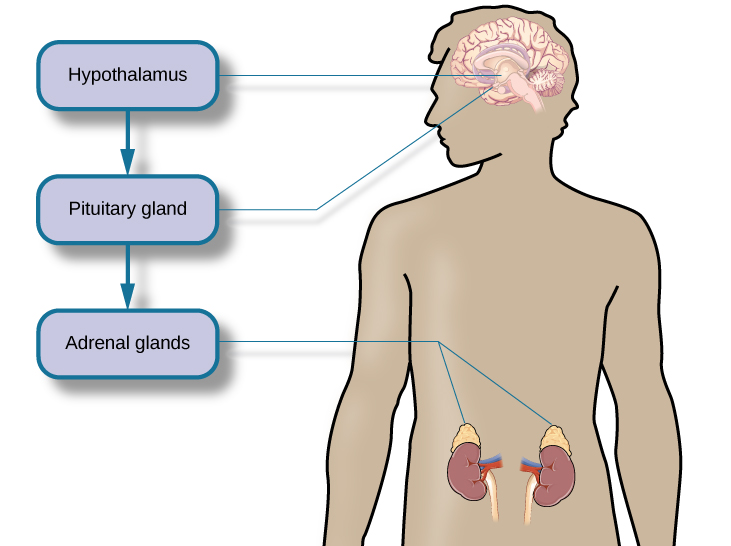
Evidence suggests that due to the cumulative stresses that accompany aging the hypothalamic-pituitary-adrenal axis tends to be hyperactive in older people.
Contributors and Attributions
- Homeostasis. Authored by: Open Learning Initiative. Provided by: Carnegie Mellon University. Located at: https://oli.cmu.edu/jcourse/webui/syllabus/module.do?context=43488d9280020ca6007d5b948d182701. Project: Anatomy & Physiology. License: CC BY-NC-SA: Attribution-NonCommercial-ShareAlike

