17.7: Cardiovascular Disease
- Last updated
- Save as PDF
- Page ID
- 22575
Heart Attack on a Plate
Eating this greasy cheeseburger smothered in bacon may not literally cause a heart attack. However, regularly eating high-fat, low-fiber foods such as this may increase the risk of a heart attack or other type of cardiovascular disease. In fact, unhealthy lifestyle choices such as this may account for as many as 90 percent of cases of cardiovascular disease.

What Is Cardiovascular Disease?
Cardiovascular disease is a class of diseases that involve the cardiovascular system. They include diseases of the coronary arteries that supply the heart muscle with oxygen and nutrients; diseases of arteries such as the carotid artery that provide blood flow to the brain; and diseases of the peripheral arteries that carry blood throughout the body. Worldwide, cardiovascular disease is the leading cause of death, causing about a third of all deaths each year.
Most cases of the cardiovascular disease occur in people over the age of 60, with disease onset typically being about a decade earlier in males than females. The LGBT (lesbian, gay, bisexual, and transgender) community belongs to almost every race, ethnicity, religion, age, and socioeconomic group. The LGBT youth are at a higher risk for cardiovascular diseases, obesity, anxiety, and depression as compared to the general population. LGBT youth receive poor quality of care due to stigma, lack of healthcare providers’ awareness, and insensitivity to the unique needs of this community. Young LGBT individuals find it difficult to report their sexual identity to their clinicians. Some clinicians are not well trained in addressing the concerns of members of this community.
You can’t control your age or sex, but you can control other factors that increase the risk of cardiovascular disease. Not smoking, maintaining a healthy weight, eating a healthy diet, taking medications as needed to control diabetes and cholesterol, and getting regular exercise are all ways to prevent cardiovascular disease or keep it from progressing. It should be noted that high blood lipid levels are definitely risk factors for cardiovascular disease. High levels of cholesterol in the diet do not appear to lead directly to high levels of cholesterol in the blood. Clearly, cardiovascular disease is multifactorial in terms of its causes.
Precursors of Cardiovascular Disease
There are two very common conditions that are precursors to virtually all cases of cardiovascular disease: hypertension (hypertension) and atherosclerosis (hardening of blood wall). Both conditions affect the arteries and their ability to maintain normal blood flow.
Hypertension
Hypertension is a chronic medical condition in which the blood pressure in the arteries is persistently elevated, as defined in Table \(\PageIndex{1}\). Hypertension usually does not cause symptoms, so more than half of the people with high blood pressure are unaware of their condition. Hypertension is typically diagnosed when blood pressure is routinely measured during a medical visit for some other health problem.
| Category | Systolic (mm Hg) | Diastolic (mm Hg) |
|---|---|---|
| Normal blood pressure | 90-119 | 60-79 |
| Prehypertension | 120-139 | 80-89 |
| Hypertension | 140 or higher | 90 or higher |
High blood pressure is classified as either primary or secondary high blood pressure. At least 90% of cases are primary high blood pressure, which is caused by some combination of genetic and lifestyle factors. Numerous genes have been identified as having small effects on blood pressure. Lifestyle factors that increase the risk of high blood pressure include excess dietary salt and alcohol consumption in addition to the risk factors for cardiovascular disease stated above. Secondary high blood pressure, which makes up the remaining 10% of cases of hypertension, is attributable to chronic kidney disease or an endocrine disorder such as Cushing’s disease.
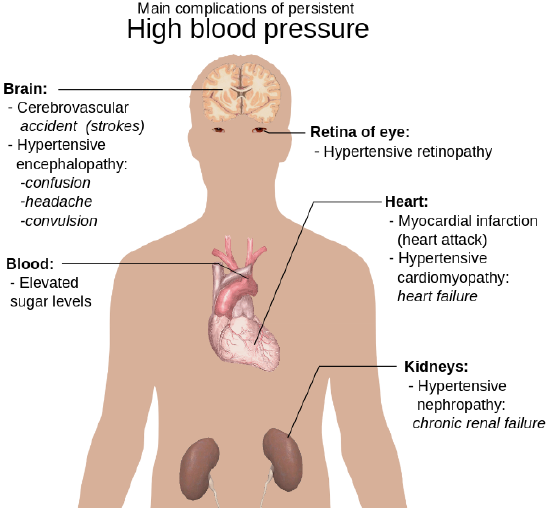
Treating hypertension is important for reducing the risk of all types of cardiovascular disease, especially stroke. These and other complications of persistent high blood pressure are shown in Figure \(\PageIndex{2}\). Lifestyle changes, such as reducing salt intake and adopting a healthier diet may be all that is needed to lower blood pressure to the normal range. In many cases, however, medications are also required.
Atherosclerosis
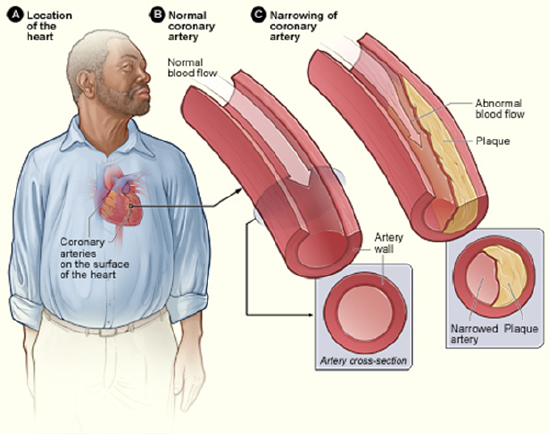
Atherosclerosis is a condition in which artery walls thicken and stiffen as a result of the buildup of plaques inside the arteries. Plaques consist of white blood cells, cholesterol, and other fats. Typically, there is also a proliferation of smooth muscle cells that make the plaque fibrous as well as fatty. Over time, the plaques may harden with the addition of calcium crystals. This reduces the elasticity of the artery walls. As plaques increase in size, the artery walls dilate to compensate so blood flow is not affected. Eventually, however, the lumen of the arteries is likely to become so narrowed by plaque buildup that blood flow is reduced or even blocked entirely. Figure \(\PageIndex{3}\) illustrates the formation of a plaque in a coronary artery.
In most people, plaques start to form in arteries during childhood and progress throughout life. Individuals may develop just a few plaques or dozens of them. Plaques typically remain asymptomatic for decades. Signs and symptoms appear only after there is severe narrowing (stenosis) or complete blockage of arteries. As plaques increase in size and interfere with blood flow, they commonly lead to the formation of blood clots. These may plug arteries at the site of the plaque or travel elsewhere in the circulation. Sometimes plaques rupture or become detached from an arterial wall and become lodged in a smaller, downstream artery. Blockage of arteries by plaques or clots may cause a heart attack, stroke, or other potentially life-threatening cardiovascular events. If blood flow to the kidneys is affected, it may lead to chronic kidney disease.
The process in which plaques form is not yet fully understood, but it is thought that it begins when low-density lipoproteins (LDLs) accumulate inside endothelial cells in artery walls, causing inflammation. The inflammation attracts white blood cells that start to form a plaque. Continued inflammation and a cascade of other immune responses cause the plaque to keep growing. Risk factors for the development of atherosclerosis include hypertension, high cholesterol (especially LDL cholesterol), diabetes, and smoking. The chance of developing atherosclerosis also increases with age, male sex, and a family history of cardiovascular disease.
Treatment of atherosclerosis often includes both lifestyle changes and medications to lower cholesterol, control blood pressure, and reduce the risk of blood clot formation. In extreme cases or when other treatments are inadequate, surgery may be recommended. Surgery may involve the placement of stents in arteries to keep them open and improve blood flow or the use of grafts to divert blood flow around blocked arteries.
Coronary Artery Disease
Coronary artery diseases are a group of diseases that result from atherosclerosis of coronary arteries. Treatment of the diseases mainly involves treating underlying atherosclerosis. Two of the most common coronary artery diseases are angina and myocardial infarction.
Angina
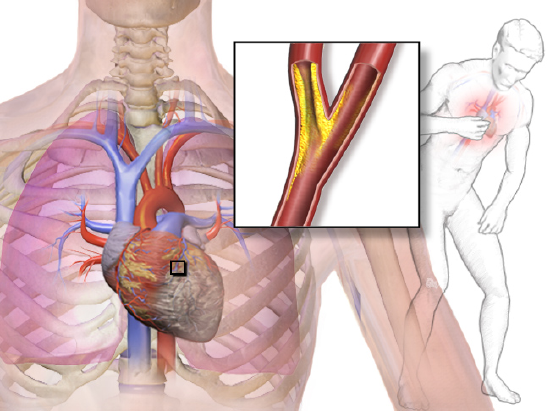
Angina is chest pain or pressure that occurs when heart muscle cells do not receive adequate blood flow and become starved of oxygen (a condition called ischemia). It is illustrated in Figure \(\PageIndex{4}\). There may also be a pain in the back, neck, shoulders, or jaw; and in some cases, the pain may be accompanied by shortness of breath, sweating, or nausea. The main goals of the treatment of angina are relieving the symptoms and slowing the progression of underlying atherosclerosis.
Angina may be classified as either stable angina or unstable angina:
- Stable angina is angina in which pain is precipitated by exertion (say, from brisk walking or running) and improves quickly with rest or the administration of nitroglycerin, which dilates coronary arteries and improves blood flow. Stable angina may develop into unstable angina.
- Unstable angina is angina in which pain occurs during rest, lasts more than 15 minutes, and is of new onset. This type of angina is more dangerous and may be a sign of an imminent heart attack. It requires urgent medical attention.
Myocardial Infarction
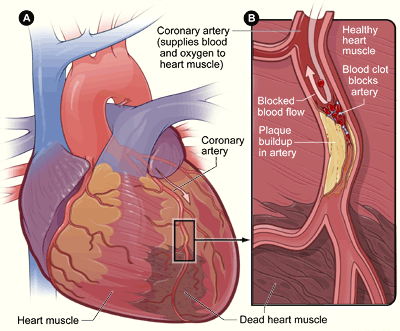
A myocardial infarction (MI), commonly known as a heart attack, occurs when blood flow stops to a part of the heart causing damage to the heart muscle and the death of myocardial cells. An MI usually occurs because of complete blockage of a coronary artery, often due to a blood clot or the rupture of a plaque (Figure \(\PageIndex{5}\)). An MI typically causes chest pain and pressure, among other possible symptoms, but at least one-quarter of MIs do not cause any symptoms.
In the worst case, an MI may cause sudden death. Even if the patient survives, an MI often causes permanent damage to the heart. This puts the heart at risk of heart arrhythmias, heart failure, and cardiac arrest.
- Heart arrhythmias are abnormal heart rhythms, which are potentially life-threatening. Heart arrhythmias often can be interrupted with a cardiac defibrillator, which delivers an electrical shock to the heart, in effect “rebooting” it.
- Heart failure occurs when the pumping action of the heart is impaired so tissues do not get adequate oxygen. This is a chronic condition that tends to get worse over time, although it can be managed with medications.
- Cardiac arrest occurs when the heart no longer pumps blood or pumps blood so poorly that vital organs can no longer function. This is a medical emergency requiring immediate intervention.
Other Cardiovascular Diseases
Hypertension and atherosclerosis often cause other cardiovascular diseases. These commonly include stroke and peripheral artery disease.
Stroke
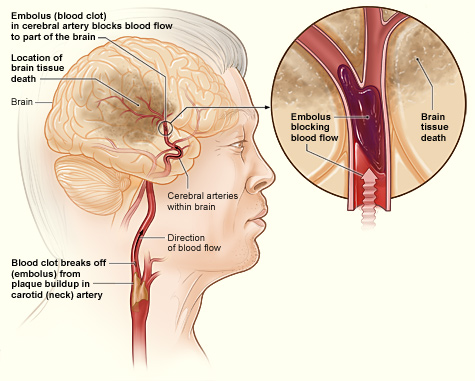
A stroke, also known as a cerebrovascular accident or brain attack, occurs when blocked or broken arteries in the brain result in the death of brain cells. There are two main types of stroke: ischemic stroke and hemorrhagic stroke. Ischemic storke is illustrated in Figure \(\PageIndex{6}\).
- An ischemic stroke occurs when an embolus (blood clot) breaks off from a plaque or forms in the heart because of arrhythmia and travels to the brain where it becomes lodged in an artery. This blocks blood flow to the part of the brain that is served by arteries downstream from the blockage. Lack of oxygen causes the death of brain cells. Treatment with a clot-busting drug within a few hours of the stroke may prevent permanent damage. Almost 90 percent of strokes are ischemic strokes.
- A hemorrhagic stroke occurs when an artery in the brain ruptures and causes bleeding in the brain. This deprives downstream tissues of adequate blood flow and also puts pressure on brain tissue. Both factors can lead to the death of brain cells. Surgery to temporarily open the cranium may be required to relieve the pressure. Only about 10 percent of strokes are hemorrhagic strokes, but they are more likely to be fatal than ischemic strokes.
In both types of stroke, the part of the brain that is damaged loses is the ability to function normally. Signs and symptoms of stroke may include an inability to move, feel, or see on one side of the body; problems understanding speech or difficulty speaking; memory problems; confusion; and dizziness. Hemorrhagic strokes may also cause a severe headache. The symptoms of a stroke usually occur within seconds or minutes of the brain injury. Depending on the severity of the stroke and how quickly treatment is provided, the symptoms may be temporary or permanent. If the symptoms of a stroke go away on their own in less than an hour or two, the stroke is called a transient ischemic attack. Stroke is the leading cause of disability in the United States, but rehabilitation with physical, occupational, speech, or other types of therapy may significantly improve functioning.
The main risk factor for stroke is high blood pressure. Therefore, keeping blood pressure within the normal range, whether with lifestyle changes or medications, is the best way to reduce the risk of stroke. Another possible cause of stroke is the use of illicit drugs such as amphetamines or cocaine. Having had a stroke in the past greatly increases one’s risk of future strokes. Men are also more likely than women to have strokes.
Peripheral Artery Disease
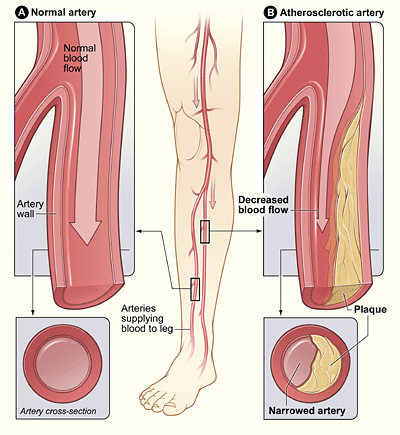
Peripheral artery disease (PAD) is the narrowing of the arteries other than those that supply the heart or brain due to atherosclerosis. Figure \(\PageIndex{7}\) shows how the PAD occurs. PAD most commonly affects the legs, but other arteries may also be involved. The classic symptom is leg pain when walking, which usually resolves with rest. This symptom is known as intermittent claudication. Other symptoms may include skin ulcers, bluish skin, cold skin, or poor nail and hair growth in the affected leg(s). However, up to half of all cases of PAD do not have any symptoms.
The main risk factor for PAD is smoking. Other risk factors include diabetes, high blood pressure, and high blood cholesterol. The underlying mechanism is usually atherosclerosis. PAD is typically diagnosed when blood pressure readings taken at the ankle are lower than blood pressure readings taken at the upper arm. It is important to diagnose PAD and treat underlying atherosclerosis because people with this disorder have a four to five times higher risk of myocardial infarction or stroke. Surgery to expand the affected arteries or to graft vessels in order to bypass blockages may be recommended in some cases.
Feature: My Human Body
You read in this concept about the many dangers of hypertension. Do you know whether you have hypertension? The only way to know for sure is to have your blood pressure measured. Measuring blood pressure is quick and painless, but several measurements are needed to accurately diagnose hypertension. Some people have what is called “white coat disease.” Their blood pressure rises just because they are being examined by a physician (in a white coat). Blood pressure also fluctuates from time to time due to factors such as hydration, stress, and time of day. Repeatedly measuring and recording your own blood pressure at home can provide your doctor with valuable diagnostic data. Digital blood pressure monitors for home use, like the one pictured in Figure \(\PageIndex{8}\), are relatively inexpensive, easy to use, and available at most pharmacies.

Review
- What is cardiovascular disease? How much mortality do cardiovascular diseases cause?
- List risk factors for cardiovascular disease.
- What is hypertension?
- Define atherosclerosis.
- What is coronary artery disease?
- Identify two specific coronary artery diseases.
- Explain how a stroke occurs and how it affects the patient.
- Describe the cause of peripheral artery disease.
- What are two cardiovascular diseases that can be caused by atherosclerosis? Explain specifically how atherosclerosis contributes to each of them.
- True or False. A heart attack is the same thing as cardiac arrest.
- True or False. Plaques in arteries can cause blood clots.
- What are the similarities between angina and ischemic stroke?
- How can kidney disease be caused by problems in the cardiovascular system?
- In peripheral artery disease, the blood pressure at the ankle is typically ________ the blood pressure at the upper arm.
A. erratic compared to B. the same as
C. higher than D. lower than
- Name three components of the plaque that can build up in arteries.
Explore More
Attributions
- Bacon Cheeseburger by Like_the_Grand_Canyon licensed CC-BY 2.0 via Wikimedia Commons
- Main complications of persistent high blood pressure Häggström, Mikael (2014). "Medical gallery of Mikael Häggström 2014". WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.008. ISSN 2002-4436. Public Domain. via Wikimedia Commons
- Coronary heart disease-atherosclerosis by NIH: National Heart, Lung and Blood Institute. Public Domain.
- Angina by Blausen.com staff (2014). "Medical gallery of Blausen Medical 2014". WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436. licensed CC BY 3.0 via Wikimedia Commons.
- Heart Attack by NIH: National Heart, Lung and Blood Institute; public domain via Wikimedia Commons.
- Stroke Ischemic by National Heart Lung and Blood Insitute (NIH); Public domain via Wikimedia Commons
- Peripheral Arterial Disease by National Heart Lung and Blood Institute; public domain via Wikimedia Commons
- Wrist style blood pressure monitor by Weeksgo licensed https://creativecommons.org/publicdomain/zero/1.0/deed.enCC0 via Wikimedia commons.
- Text adapted from Human Biology by CK-12 licensed CC BY-NC 3.0
- Some text is adapted from Health Care Disparities Among Lesbian, Gay, Bisexual, and Transgender Youth: A Literature Review; Hudaisa Hafeez, Muhammad Zeshan, Muhammad A Tahir, Nusrat Jahan, and Sadiq Naveed; Cureus. 2017 Apr; 9(4): e1184. Published online 2017 Apr 20. doi: 10.7759/cureus.1184; CC By 4.0.


