15.6.1.10: Hormones of Kidney, Skin and Heart
- Page ID
- 5484
Kidney
The human kidney secretes two hormones:
- Erythropoietin (EPO)
- Calcitriol (1,25[OH]2 Vitamin D3)
as well as the enzyme renin.
Erythropoietin (EPO)
Erythropoietin is a glycoprotein that acts on the bone marrow to increase the production of red blood cells. Stimuli such as bleeding or moving to high altitudes (where oxygen is scarcer) trigger the release of EPO. People with failing kidneys can be kept alive by dialysis, which only cleanses the blood of wastes. Without a source of EPO, these patients suffer from anemia. Now, thanks to recombinant DNA technology, recombinant human EPO is available to treat these patients.
Some other uses for recombinant EPO:
- Some of the drugs used to treat AIDS, zidovudine (AZT) for example, cause anemia as a side effect. Recombinant EPO helps AIDS patients cope with this one of the many problems that the disease creates.
- Recombinant EPO improves the anemia that is such a frequent side effect of cancer chemotherapy.
- Severe blood loss in Jehovah's Witnesses, whose religion forbids them to receive blood transfusions, can also be helped with recombinant EPO.
Because EPO increases the hematocrit, it enables more oxygen to flow to the skeletal muscles. Some cyclists (and distance runners) have used recombinant EPO to enhance their performance. Although recombinant EPO has exactly the same sequence of amino acids as the natural hormone, the sugars attached by the cells used in the pharmaceutical industry differ from those attached by the cells of the human kidney. This difference can be detected by a test of the athlete's urine.
Another problem: since recombinant EPO became available, over two dozen young competitive cyclists have died unexpectedly (usually during the night). Perhaps an EPO-induced increase in their hematocrit — leading to a reduction in heart rate — is responsible. Prolonged exposure to reduced oxygen levels (e.g., living at high altitude) leads to increased synthesis of EPO. In mice, and perhaps in humans, this effect is mediated by the skin. Mouse skin cells can detect low levels of oxygen ("hypoxia") and if this persists, blood flow to the kidneys diminishes leading to increased synthesis of EPO by them.
EPO is also synthesized by osteoblasts in mice that have been made anemic and in the brain when oxygen becomes scarce there (e.g., following a stroke), and helps protect neurons from damage. Perhaps recombinant human EPO will turn out to be useful for stroke victims as well.
Calcitriol
Calcitriol is 1,25[OH]2 Vitamin D3, the active form of vitamin D. It is derived from
- calciferol (vitamin D3) which is synthesized in skin exposed to the ultraviolet rays of the sun
- precursors ("vitamin D") ingested in the diet.
Calciferol in the blood is converted into the active vitamin in two steps:
- calciferol is converted in the liver into 25[OH] vitamin D3
- this is carried to the kidneys (bound to a serum globulin) where it is converted into calcitriol. This final step is promoted by the parathyroid hormone (PTH).
Calcitriol Action
Calcitriol acts on
- the cells of the intestine to promote the absorption of calcium and phosphate from food
- bone to mobilize calcium from the bone to the blood
Calcitriol enters cells and, if they contain receptors for it (intestine cells do), it binds to them. The calcitriol receptors are zinc-finger transcription factors. The receptor-ligand complex bind to its response element, the DNA sequence:
5' AGGTCAnnnAGGTCA 3'
This sequence of nucleotides (n can be any nucleotide) is found in the promoters of genes that are turned on by calcitriol. Once the hormone-receptor complex is bound to its response element, other transcription factors are recruited to the promoter and transcription of the gene(s) begins.
Deficiency disorders
Insufficient calcitriol prevents normal deposition of calcium in bone.
- In childhood, this produces the deformed bones characteristic of rickets.
- In adults, it produces weakened bones causing osteomalacia.
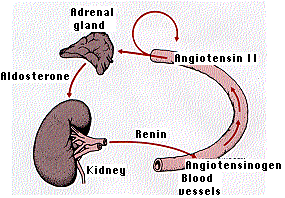
Angiotensin II modulates all of the below actions to increase in blood pressure:
- constricts the walls of arterioles closing down capillary beds
- stimulates the proximal tubules in the kidney to reabsorb sodium ions
- stimulates the adrenal cortex to release aldosterone. Aldosterone causes the kidneys to reclaim still more sodium and thus water.
- increases the strength of the heartbeat
- stimulates the pituitary to release the vasopressin
Skin
When ultraviolet radiation strikes the skin, it triggers the conversion of dehydrocholesterol (a cholesterol derivative) into calciferol (vitamin D3). Calciferol travels in the blood to the liver where it is converted into 25[OH] vitamin D3. This compound travels to the kidneys where it is converted into calcitriol (1,25 [OH]2 vitamin D3). This final step is promoted by the parathyroid hormone (PTH). Although called a vitamin, calciferol and its products fully qualify as hormones because they are
- made in certain cells
- carried in the blood
- affect gene transcription in target cells
Heart
Natriuretic Peptides
In response to a rise in blood pressure, the heart releases two peptides:
- A-type Natriuretic Peptide (ANP)
This hormone of 28 amino acids is released from stretched atria (hence the "A").
- B-type Natriuretic Peptide (BNP)
This hormone (29 amino acids) is released from the ventricles. (It was first discovered in brain tissue; hence the "B".)
Both hormones lower blood pressure by
- relaxing arterioles
- inhibiting the secretion of renin and aldosterone
- inhibiting the reabsorption of sodium ions by the kidneys.
The latter two effects reduce the reabsorption of water by the kidneys. So the volume of urine increases as does the amount of sodium excreted in it. The net effect of these actions is to reduce blood pressure by reducing the volume of blood in the circulatory system. These effects give ANP and BNP their name (natrium = sodium; uresis = urinate).


